Body dysmorphic disorder (BDD) is characterised by a preoccupation with an imagined defect or a markedly excessive concern, where there is a slight physical anomaly (DSM-IV; American Psychiatric Association, 1994). Many patients with BDD crave to change their appearance by cosmetic surgery or by dermatological treatments. I have previously reported that in 50 patients with BDD in the UK, 26% had managed to obtain one or more cosmetic operations (Reference Veale, Boocock and GournayVeale et al, 1996a ). There are no outcome studies of cosmetic surgery in BDD apart from Phillips et al (Reference Phillips, McElroy and Keek1993) who reported on eight patients who had between them undergone 25 plastic or dental surgery procedures. Only two procedures led to an improvement of remission of symptoms while 20 procedures resulted in an exacerbation of symptoms. BDD is not uncommon in cosmetic surgery clinics. In a recent survey of 100 women seeking cosmetic surgery in the USA, 5% met the diagnostic criteria for BDD (Reference Sarwer, Wadden and PertschukSarwer et al, 1998). This paper reports both on BDD patients seen in the UK about their experience of cosmetic surgery and on the occurrence of DIY cosmetic surgery in patients unable to obtain the surgery they crave.
The study
Data were collected on 25 patients with BDD who reported at the time of psychiatric assessment that they had had cosmetic surgery in the past. Referrals were from their general practitioner (n=8), a consultant psychiatrist (n=7), or self-referral or via a patient support group (n=10). Patients were asked to rate:
-
(a) the degree of satisfaction with the outcome of each operation they had had on a scale between zero and 10, where zero represented extreme dissatisfaction and 10 extreme satisfaction;
-
(b) any change in the overall amount of time they took and distress they experienced thinking about their appearance after the operation on a scale between one and seven where one represented ‘very much less’ and seven was ‘very much more’ (Reference GuyGuy, 1976);
-
(c) any change in the overall degree of handicap in relation to their occupational and social life after the operation on the same scale as above.
Patients were also asked if after an operation the preoccupation transferred to another area of the body.
Findings
The sample consisted of 25 patients with BDD who had had a total of 46 procedures. Ten patients had undergone one procedure, 10 patients had undergone two procedures, four patients had undergone three procedures, and one patient had undergone four procedures. They had a mean age of 36.0 years (range 22-63) and 12% of the sample was male. The operations had occurred a mean of 5.6 years ago. Twenty-six per cent of the operations were performed on the NHS. Many of those who had had private cosmetic surgery had taken out loans or borrowed from relatives.
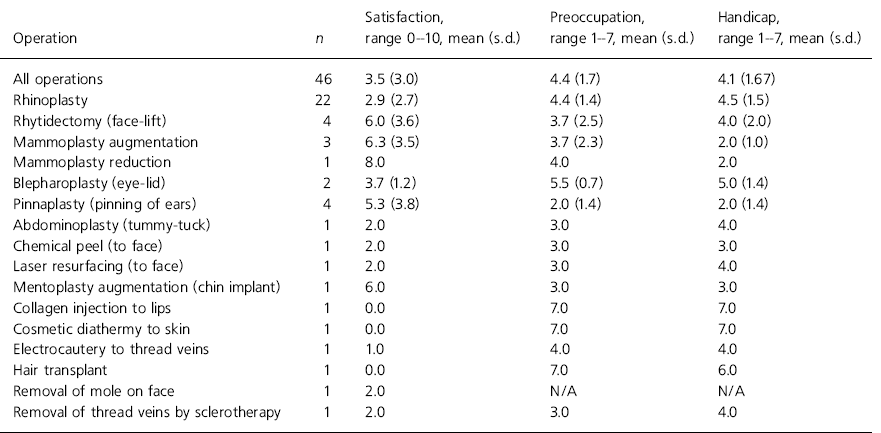
Three patients claimed that they were not preoccupied by their appearance prior to the surgery and that their symptoms of BDD developed only after surgery, which they believed had been done badly. The satisfaction ratings and any change in preoccupation and overall handicap are listed in Table 1. The numbers of several procedures are small but the satisfaction ratings tended to be higher for mammoplasty, rhytidectomy (face-lift) and pinnaplasty. Mammoplasty and pinnaplasty (but not rhytidectomy) tended to lead to an overall decrease in preoccupation and handicap.
Table 1. Ratings of satisfaction, preoccupation and handicap for each type of operation
| Operation | n | Satisfaction, range 0-10, mean (s.d.) | Preoccupation, range 1-7, mean (s.d.) | Handicap, range 1-7, mean (s.d.) |
|---|---|---|---|---|
| All operations | 46 | 3.5 (3.0) | 4.4 (1.7) | 4.1 (1.67) |
| Rhinoplasty | 22 | 2.9 (2.7) | 4.4 (1.4) | 4.5 (1.5) |
| Rhytidectomy (face-lift) | 4 | 6.0 (3.6) | 3.7 (2.5) | 4.0 (2.0) |
| Mammoplasty augmentation | 3 | 6.3 (3.5) | 3.7 (2.3) | 2.0 (1.0) |
| Mammoplasty reduction | 1 | 8.0 | 4.0 | 2.0 |
| Blepharoplasty (eye-lid) | 2 | 3.7 (1.2) | 5.5 (0.7) | 5.0 (1.4) |
| Pinnaplasty (pinning of ears) | 4 | 5.3 (3.8) | 2.0 (1.4) | 2.0 (1.4) |
| Abdominoplasty (tummy-tuck) | 1 | 2.0 | 3.0 | 4.0 |
| Chemical peel (to face) | 1 | 2.0 | 3.0 | 3.0 |
| Laser resurfacing (to face) | 1 | 2.0 | 3.0 | 4.0 |
| Mentoplasty augmentation (chin implant) | 1 | 6.0 | 3.0 | 3.0 |
| Collagen injection to lips | 1 | 0.0 | 7.0 | 7.0 |
| Cosmetic diathermy to skin | 1 | 0.0 | 7.0 | 7.0 |
| Electrocautery to thread veins | 1 | 1.0 | 4.0 | 4.0 |
| Hair transplant | 1 | 0.0 | 7.0 | 6.0 |
| Removal of mole on face | 1 | 2.0 | N/A | N/A |
| Removal of thread veins by sclerotherapy | 1 | 2.0 | 3.0 | 4.0 |
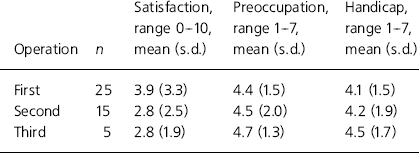
The satisfaction rating was relatively low for rhinoplasty, which was the most common procedure. The nose is also the most usual location for complaint by patients with BDD (Reference Veale, Boocock and GournayVeale et al, 1996a ). Rhinoplasty tended to be associated with an increase in preoccupation and handicap. Most of the patients in the study had multiple concerns about their appearance and reported that after 50% of the procedures the preoccupation transferred tc another area of their body. After one procedure, the mean satisfaction rating was 3.9 (see Table 2). By the second or third procedure, this had dropped to 2.8. The second or third procedure was not always a revision of the first procedure. For example, of the 17 patients who had rhinoplasty, only three underwent one or more revisions and 14 had a different procedure when their preoccupation moved to a different area of the body. When patients were dissatisfied with their operation, they often felt guilty or angry with themselves or the surgeon for having made their appearance worse, thus further fuelling their depression and a failure to achieve their ideal. This in turn tended to increase mirror gazing and craving for more surgery. Six patients rated themselves as satisfied with their procedure (defined as a rating of 7-10). Four of these patients went on to have one or more further procedures or were dissatisfied with another area of their body but did not have further surgery.
Table 2. Satisfaction with repeated operation
| Operation | n | Satisfaction, range 0-10, mean (s.d.) | Preoccupation, range 1-7, mean (s.d.) | Handicap, range 1-7, mean (s.d.) |
|---|---|---|---|---|
| First | 25 | 3.9 (3.3) | 4.4 (1.5) | 4.1 (1.5) |
| Second | 15 | 2.8 (2.5) | 4.5 (2.0) | 4.2 (1.9) |
| Third | 5 | 2.8 (1.9) | 4.7 (1.3) | 4.5 (1.7) |
‘DIY’ cosmetic surgery
Nine patients with BDD (of whom two were included in the sample above) reported performing their own cosmetic surgery in which they attempted to alter their appearance dramatically. This was either in desperation at being turned down for cosmetic surgery or because they could not afford it. The procedures were often associated with many hours of mirror gazing and intense disgust at their perceived defect. Examples of the procedures that were undertaken are shown in the Appendix. All cases were dissatisfied with the results of their own attempts at surgery.
Comment
Most patients with BDD reported a high degree of dissatisfaction with cosmetic surgery and an increase in their symptoms of BDD or overall handicap. Repeated surgery tended to lead to increasing dissatisfaction. Some operations, such as rhinoplasty appear to be associated with higher degrees of dissatisfaction. Mammoplasty and pinnaplasty tended to have relatively higher satisfaction ratings. These operations tend to be unambiguous in that the patient can usually describe the problem that concerns them and their desired outcome and the cosmetic surgeon can understand their expectations.
Even when patients were partially or wholly satisfied with the results then the preoccupation transferred to a different area of the body and they remained significantly handicapped in their symptoms of BDD. There is a suggestion that the onset of BDD for some patients occurred after cosmetic surgery although this needs confirmation in a larger prospective study of patients before cosmetic surgery.
The main weaknesses of this study and that of Phillips et al (Reference Phillips, McElroy and Keek1993) are:
-
(a) The data are retrospective and there is a selection bias of patients in favour of treatment failures. Mental health practitioners are unlikely to see patients with BDD who might be satisfied with their cosmetic surgery and have overcome their symptoms of BDD. However, at this stage, it is not known what factors might predict satisfaction in patients with BDD who undergo surgery and in whom the preoccupation does not transfer repeatedly to another area of the body.
-
(b) A variety of different cosmetic operations were under scrutiny and it is difficult to interpret the success of some operations which have only one or two procedures in this sample.
-
(c) There is no control group of psychiatric patients who have undergone cosmetic surgery but do not have BDD. However, the majority of individuals (who do not have BDD) are very satisfied with cosmetic surgery and their self-esteem and other psychological measures improve (Reference Klassen, Fitzpatrick and JenkinsonKlassen et al, 1996; Reference Carr, Harris and JamesCarr et al, 2000).
There is, however, never likely to be a randomised-controlled trial of cosmetic surgery in patients with BDD comparing, for example, cognitive-behavioural therapy (Reference Veale, Gournay and DrydenVeale et al, 1996b ) or a serotonin reuptake inhibitor (Reference Hollander, Allen and KwonHollander et al, 1999). At best, a prospective study of patients with BDD undergoing specific cosmetic surgery operations with a long-term follow-up is required to determine efficacy in the long term and whether patients eventually become satisfied after several operations.
The motivation for DIY surgery is complex, but it appears primarily either to camouflage a perceived defect or to try to achieve an unrealistic ideal. It does not fit the existing classification of self-harm by Favazza & Rosenthal (Reference Favazza and Rosenthal1993). It has a similar poor psychological outcome in so far as nearly all the patients were dissatisfied with their handiwork and found their symptoms of BDD were exacerbated. It reflects the extreme measures that some patients take and is mirrored in the high rate of attempted suicide in this population (Reference Veale, Boocock and GournayVeale et al, 1996a ).
Appendix
Examples of DIY cosmetic surgery
A man preoccupied by his skin who believed that it was too ‘loose’. He used a staple gun on both sides of his face to try to keep his skin taut. The staples fell out after 10 minutes and he narrowly missed damaging his facial nerve.
A woman preoccupied by her skin and the shape of her face. She filed down her teeth in order to alter the appearance of her jaw-line.
A man who was preoccupied with the appearance of his chin deliberately cycled into the back of a lorry in an attempt to fracture his jaw so that it could be reset in a way that he wanted. At the last moment, he decided against the plan, dropped his head, cut his forehead and fractured his skull.
A man preoccupied by his facial skin said he had used sandpaper as a form of dermabrasion to remove scars and to lighten his skin.
A man who was preoccupied by redness on his skin repeatedly exsanguinated himself by a syringe and needle or when he was accepted, by going to blood transfusion clinics to ‘make himself look paler’.
A woman who was preoccupied by the ugliness of multiple areas of her body who desired liposuction but could not afford it, used a knife to cut her thighs and attempted to squeeze out the fat.
Acknowledgement
I would like to thank Susan Riley, Assistant Psychologist, for help in collection of the data and Dr Marc Serfaty for his comments.







eLetters
No eLetters have been published for this article.