For child and adolescent psychiatry, the advent of Certificates of Completion of Specialist Training (CCSTs) has meant a reduction in the duration of specialist training from four years to three and a thorough review of training objectives and guidance on how to organise training. The Child and Adolescent Psychiatry Specialist Advisory Committee (CAPSAC) of the Higher Specialist Training Committee (HSTC) of the Royal College of Psychiatrists makes recommendations concerning training objectives and carries out regular inspections of training schemes in the UK and Republic of Ireland. It has the power to insist on changes to training schemes if, in its view, training is not being properly organised, and can if necessary remove approval for training.
Training in child and adolescent psychiatry has been the subject of systematic review twice in the last 20 years. In 1979, a postal questionnaire was sent to all 107 senior registrars in training (Reference Garralda, Wieselberg and MrazekGarralda et al, 1983). In 1988, following a revision of training guidelines a further questionnaire survey was conducted (Reference Bools and CottrellBools & Cottrell, 1990). Given the major changes in higher training since this last survey, it seemed timely to conduct another survey.
Method
The programme director for each training scheme in the UK and Ireland was asked to distribute questionnaires to trainees on their scheme between September and December 1998. One reminder was sent via programme directors if there was no response after three months. The questionnaire was based as far as possible on the 1990 questionnaire. Changes in training guidelines and in service provision meant that some changes had to be made. A small group of trainers and trainees were consulted about the additional content and revised format. The questionnaire covered five main areas:
-
(a) demographics;
-
(b) therapeutic orientation;
-
(c) present training scheme;
-
(d) availability and importance of training experiences;
-
(e) knowledge of training guidelines and representation.
Results
Of 234 higher trainees in post at the time of the survey, 207 returned questionnaires, giving a response rate of 88%. Two of the Dublin schemes, each of which had only one trainee and one Scottish scheme with two trainees did not have any respondents, but most trainees in other schemes responded, making this survey representative of training nationally.
Demographics
One hundred and one (49%) of trainees were senior registrars, and 80 were (39%) specialist registrars. Eighteen were lecturers (9%) and eight in other posts such as research fellowships (4%). The majority were female (60%), full-time trainees (75%). Fifty-seven per cent had prior paediatric experience.
Therapeutic orientation
Systemic therapies were most frequently ranked most favoured (44%) and biological therapies most frequently ranked least favoured (29%). This compares with the 1988 and 1979 surveys, in which psychodynamic therapies were ranked as most favoured (34% and 55% of respondents respectively), from psychodynamic, social community, behavioural and biological therapies.
Present training scheme
The mean number of hours of patient contact per week for full-time trainees was 16.3 (range 1-32) and for part-time trainees 11.5 (range 2-32). Case-loads varied widely, with a mean of 26 cases in treatment for full-timers (range 2–110) and 16.5 for part-timers (range 4–42). Eight per cent of trainees had less than the equivalent of one hour per week of individual consultant supervision.
Five respondents reported they did not have a formal academic training programme, including the majority of trainees on one scheme. This is extremely concerning and if correct, this should lead to loss of accreditation of this scheme. Thirty-one per cent reported no formal teaching in research methods. Since trainees on the same scheme disagreed about the content of academic programmes, there may be inadequate dissemination of information. One hundred and sixteen trainees (56%) had no papers published in peer-reviewed journals. Nine per cent had published more than two papers. One hundred and eighty-two (88%) had a research project in progress and 33% (n=68) were registered for or had obtained a higher degree.
Only 11 trainees reported they did not have regular reviews with their programme director, but 33% said they did not get feedback on their performance from their programme director. Thirty-three respondents (17%) were not satisfied with the organisation of training by the programme director. Lack of planning of placements by the programme director was a frequent complaint among these trainees.
Availability and importance of training experiences
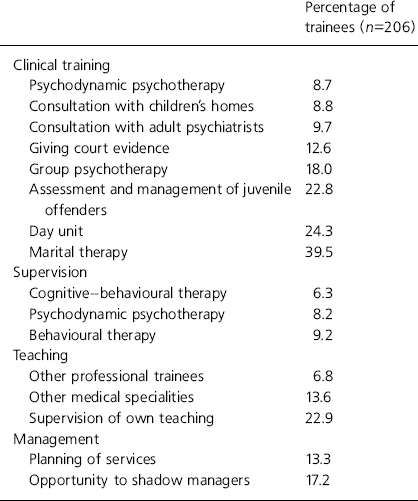
Most trainees were confident they would obtain most recommended training experiences during their training. The percentage of trainees reporting that they would definitely not obtain certain training experiences, where this is greater than 5% is displayed in Table 1.
Table 1. Percentage of trainees reporting they would definitely not obtain specific training experiences (where the percentage is greater than 5%)
| Percentage of trainees (n = 206) | |
|---|---|
| Clinical training | |
| Psychodynamic psychotherapy | 8.7 |
| Consultation with children's homes | 8.8 |
| Consultation with adult psychiatrists | 9.7 |
| Giving court evidence | 12.6 |
| Group psychotherapy | 18.0 |
| Assessment and management of juvenile offenders | 22.8 |
| Day unit | 24.3 |
| Marital therapy | 39.5 |
| Supervision | |
| Cognitive–behavioural therapy | 6.3 |
| Psychodynamic psychotherapy | 8.2 |
| Behavioural therapy | 9.2 |
| Teaching | |
| Other professional trainees | 6.8 |
| Other medical specialities | 13.6 |
| Supervision of own teaching | 22.9 |
| Management | |
| Planning of services | 13.3 |
| Opportunity to shadow managers | 17.2 |
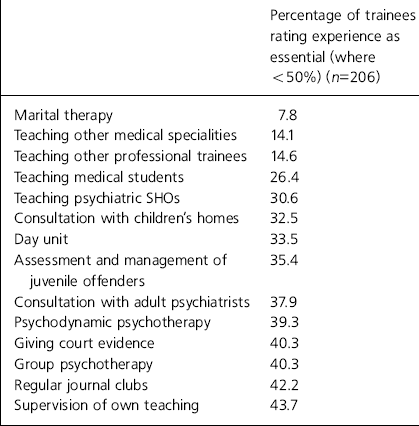
Since the training experiences were derived largely from training guidelines, it was expected that the vast majority of trainees would view them as essential. For most experiences this was the case. Table 2 shows the experiences that less than 50% of trainees thought were essential to their training.
Table 2. Experiences that were rated essential by less than 50% of trainees
| Percentage of trainees rating experience as essential (where <50%) (n = 206) | |
|---|---|
| Marital therapy | 7.8 |
| Teaching other medical specialities | 14.1 |
| Teaching other professional trainees | 14.6 |
| Teaching medical students | 26.4 |
| Teaching psychiatric SHOs | 30.6 |
| Consultation with children's homes | 32.5 |
| Day unit | 33.5 |
| Assessment and management of juvenile offenders | 35.4 |
| Consultation with adult psychiatrists | 37.9 |
| Psychodynamic psychotherapy | 39.3 |
| Giving court evidence | 40.3 |
| Group psychotherapy | 40.3 |
| Regular journal clubs | 42.2 |
| Supervision of own teaching | 43.7 |
Knowledge of representation and training guidelines
Twelve per cent of trainees had not seen CAPSAC's training advisory papersFootnote 1 and 20% had not seen the HSTC Handbook (NHS Executive, 1998). Eighty-eight per cent of trainees knew of CAPSAC, but 24% were unaware of comments made about their scheme on previous CAPSAC visits. Seventy per cent were not aware who the chair of the trainees' group was and 59% did not know who the trainee representative on CAPSAC was.
Discussion
Clinical experiences
Most clinical experiences are well provided, those that are less well provided being those which are rated as less important. While this may simply reflect the changing role of child psychiatrists, in the cases of marital and psychodynamic psychotherapies, it is of concern where experiences may form an important part of future consultants' work. Specifically, the assessment and management of juvenile offenders is relatively poorly provided and unvalued, yet is likely to form an increasing part of consultant workload with the introduction of Youth Offending Teams. Similarly teaching, while a common experience, is relatively unvalued. However, it shares core skills with the psychoeducational psychotherapies and provides one way that child and adolescent psychiatrists can help to disseminate good practice within tiered child and adolescent mental health services.
Research
Training guidelines allow for one day per week to be spent on research. Thirty-one per cent of trainees reported they did not receive formal research training. Twelve per cent of trainees were not certain they would have the equivalent of one day per week for research and 18 trainees appear to be taking research time without having a project. Given the cost of providing one day per week as research time, it is questionable whether this is the most efficient way of promoting either research in child and adolescent mental health or trainees' understanding of research methodology. While registration for a higher degree or publication of papers cannot be taken as absolute indicators of the quality of research, a significant number of trainees appear to be undertaking research which does not result in published papers and are doing so without formal teaching.
Knowledge of training guidelines
It is particularly concerning that many trainees had not seen the CAPSAC advisory papers or the HST Handbook, since these set out training requirements. At this advanced stage in training, it may be argued that trainees should be taking more responsibility for ensuring their training meets the guidelines. The confusion apparent between trainees on the same scheme as to what is available and trainees' generally poor knowledge of CAPSAC and training issues suggest this may not be the case.
In conclusion, despite clear guidelines, trainees are not universally and consistently receiving the training experiences expected. Improvements have been made since 1990, notably in provision of supervision and access to a range of clinical experiences. Clearer dissemination of information on available training experiences is important but also trainees' personal responsibility for ensuring their training meets guidelines and equips them to be child psychiatrists of the future.
Acknowledgements
The authors are grateful to Mrs Susanna Gray for her help in distributing the questionnaire and to all the trainees who responded.







eLetters
No eLetters have been published for this article.