Depersonalisation was described clinically over 100 years ago, yet there has been little research into this interesting but distressing psychiatric disorder. The symptom of depersonalisation can occur alone or in the context of other psychiatric and neurological illnesses and is characterised by the experience of detachment from one's senses and the outside environment, and may be present for several years without remission. Two years after the establishment of the depersonalisation research unit at the Maudsley Hospital, London, we report on current neurobiological and clinical research findings, including functional magnetic resonance imaging, psychophysiology and neuroendocrinology and progress regarding the development of effective treatments.
Depersonalisation
Depersonalisation was first comprehensively described by the French psychiatrist, Dugas (Reference Dugas1898). It is an unpleasant alteration in the perception or experience of the self. According to DSM—IV, depersonalisation disorder (DPD) is characterised by persistent or recurrent episodes of
“A feeling of detachment or estrangement from one's self… There may be the sensation of being an outside observer on one's own mental processes…Various types of sensory anaesthesia, lack of affective response…are often present.” (American Psychiatric Association, 1994)
Derealisation (the sense that the external world is strange or unreal) may also be present.
Such symptoms have been found in 2.4% of the general population (Reference Ross and LoewensteinRoss, 1991) and 80% of psychiatric in-patients, of whom 12% had severe and persistent depersonalisation (Reference Brauer, Harrow and TuckerBrauer et al, 1970). Depersonalisation can occur as a primary disorder, or as a feature of depression, anxiety states and schizophrenia. It also occurs in neurological conditions such as the aura to temporal lobe epilepsy, and in healthy individuals during fatigue, meditation, extreme stress or after use of hallucinogenic drugs. Classical descriptions emphasise reduced, ‘numbed’, or even absent emotional reactions, for example, ‘all my emotions are blunted’, and ‘the emotional part of my brain is dead’ (Reference Mayer-GrossMayer-Gross, 1935; Reference ShorvonShorvon, 1946; Reference AcknerAckner, 1954). Historically, a neuropsychological basis for depersonalisation has been considered, stimulated by clinical observations on patients with neurological disorders, and psychophysiological studies (Reference Sierra and BerriosSierra & Berrios, 1998).
The depersonalisation research unit clinic at the Maudsley Hospital
The remit of the unit is: (a) research into depersonalisation disorder; (b) the development of treatments, both pharmacological and psychological; and (c) to increase awareness and knowledge of the condition.
Since 1998 we have established a national depersonalisation research clinic that takes referrals from within the local NHS trust, throughout the UK and even internationally. This is currently funded from grants thanks to the generosity of the Pilkington Family Charitable Trusts, who first proposed such a unit, with some additional funding for specific research projects from the Medical Research Council. Following the decision to fund the unit, a small publicity campaign was launched. The centrepiece was an article in The Times (12 March 1998, p. 20), and an announcement in the Psychiatric Bulletin (1998, vol 22 p. 399). The clinic now sees one to two new patients per week and several follow-ups. To date, approximately 100 cases have been given a full assessment. The DPD unit has a website that receives up to 1000 hits per month and we have sent information leaflets to over 300 callers. Patients are given a thorough evaluation and offered the chance to participate in research and future treatment trials. A full report is sent to the patient's general practitioner.
Research
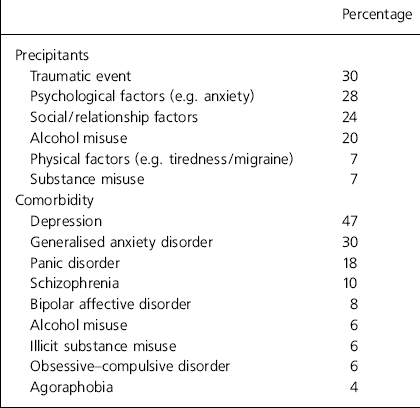
Using data collected from a total of 88 patients attending the clinic and those contacted through the DPD unit website, we have examined the demographic, clinical and neuropsychological features of DPD. Our findings indicate that the disorder is experienced equally by men and women, with a mean age of onset of 21 years and a mean illness duration of 16 years, which is mostly chronic and continuous (see Table 1). Although many patients are unable to recall an initial precipitant at onset, 30% of our sample have reported the experience of a traumatic event, and other important factors including social and relationship problems and substance misuse (e.g. ecstasy). Many patients also report that physical factors, including tiredness and migraine, and situational factors such as bright lights and noise, have contributed to the onset of symptoms. In this sample other psychiatric illnesses were present, in particular depression (47%) and generalised anxiety (30%) (Table 2). The results are in line with data from a specialised clinic at the Mount Sinai Hospital, New York (Reference Simeon, Gross and GuralnikSimeon et al, 1997).
Table 1. Demographic variables of the patients included in the study (n=88)

| Variable | |
|---|---|
| Age | 39 years (16-83) |
| Education | 67% Higher Education |
| Male:female | 51%:49% |
| Illness duration (range) | 16 years (0.5-69) |
| Age of onset (range) | 21 years (5-69) |
| Depersonalisation only | 25% |
| Derealisation | 4% |
| Both | 71% |
| Course | Episodic 15% |
| Chronic 77% | |
| Remainder not specified |
Table 2. Precipitants and co-morbidity
| Percentage | |
|---|---|
| Precipitants | |
| Traumatic event | 30 |
| Psychological factors (e.g. anxiety) | 28 |
| Social/relationship factors | 24 |
| Alcohol misuse | 20 |
| Physical factors (e.g. tiredness/migraine) | 7 |
| Substance misuse | 7 |
| Comorbidity | |
| Depression | 47 |
| Generalised anxiety disorder | 30 |
| Panic disorder | 18 |
| Schizophrenia | 10 |
| Bipolar affective disorder | 8 |
| Alcohol misuse | 6 |
| Illicit substance misuse | 6 |
| Obsessive-compulsive disorder | 6 |
| Agoraphobia | 4 |
Rating and quantifying the phenomenology and severity of the disorder has been improved by refinements in various scales such as items from the Dissociative Experiences Scale (see Reference Simeon, Gross and GuralnikSimeon et al, 1998a ; Reference Sierra and BerriosSierra & Berrios, 2000). We have found that it is probably not possible to distinguish primary and secondary depersonalisation on these grounds alone and that some level of depression and anxiety is frequently observed even in primary cases (Reference Lambert, Senior and PhillipsLambert et al, 2001a ).
Internet study
Depersonalisation disorder is frequently misdiagnosed, with the average time from misdiagnosis to correct diagnosis being approximately 7-10 years (Reference Steinberg, Cicchetti and BuchananSteinberg et al, 1993). This results in many sufferers not reaching the attention of specialists in this field. Patients often resort to the internet to determine or verify their diagnosis (http://www.iop.kcl.ac.uk ). We placed a request for volunteers to take part in a psychometric study on the depersonalisation website. Twenty-one subjects completed a battery of questionnaires. Twelve were contacted by telephone and underwent a clinical interview. The subjects were from developed countries mainly; 62% were male. The demographic details and psychiatric variables were compared with 29 patients assessed in the depersonalisation research clinic. There were no significant differences in terms of age, gender, duration or severity of depersonalisation between the groups. In addition, a series of questions were posted on the depersonalisation bulletin board. The responses were typical of those published in the literature (Reference Simeon, Gross and GuralnikSimeon et al, 1997), but additional information about the association with alcohol and the sometimes adverse effects of various treatments including selective serotonin reuptake inhibitors was obtained. This study supported the validity of using the internet for clinical research in psychiatry (Reference Senior, Phillips and DavidSenior et al, 1997; Reference Lambert, Fewtrell and PhillipsLambert et al, 2001b ).
Biological research
Investigation of the neuropsychological features of the disorder is underway. A main focus of the research of the unit has been the investigation of the neurobiological basis of DPD. We have been able to employ functional magnetic resonance imaging (fMRI) to demonstrate abnormal neural responses to presentation of emotional stimuli in patients with depersonalisation. Patients suffering from the disorder fail to activate brain regions associated with perception of emotion (e.g. the insula) during presentation of scenes depicting unpleasant events and objects. Furthermore, our findings have indicated that in these patients the ‘emotion centres’ appear to be inhibited by activation of other brain regions (e.g. prefrontal cortex) associated with the performance of executive functions.
We have also been able to confirm that patients suffering from DPD do not demonstrate the normal pattern of increased skin conductance response, first discovered by Lader (Reference Lader1975), during the viewing of these emotionally-salient stimuli, but instead demonstrate a flattened response reminiscent of the normal skin conductance response to neutral stimuli. This occurs in the face of intact recognition of the emotion in question. The results of these studies are compelling evidence for the presence in DPD of an inhibition of the normal neural response to emotion. Further studies employing fMRI and skin conductance measures are underway to investigate these findings and their specificity in more detail.
Finally, in collaboration with colleagues at Newcastle University School of Medicine we have carried out a pilot study of diurnal cortisol secretion using salivary samples in patients suffering from DPD. Preliminary results suggest a pattern of hypocortisolaemia, quite unlike depression but similar to disorders such as post-traumatic stress disorder (Reference YehudaYehuda, 1998).
Treatment
A central aim of the depersonalisation research unit is to develop effective therapeutic interventions for the treatment of depersonalisation disorder. Many treatments have been tried but few have been consistently successful. Fluoxetine has been prescribed with limited success (Reference Hollander, Liebowitz and DecariaHollander et al, 1990) and the only controlled trial to date showed that clomipramine was effective in some patients (Reference Simeon, Stein and HollanderSimeon et al, 1998b ). Lamotrigine, an anticonvulsant that blocks voltage-dependent sodium channels and inhibits glutamate release, is useful not only in the treatment of epilepsy, but also resistant bipolar disorder. Furthermore, lamotrigine has been demonstrated to reduce the intensity of depersonalisation-like symptoms induced by sub-anaesthetic doses of ketamine, a N-methyl-D-aspartate reception antagonist that also induces glutamate release (Reference Anand, Charney and OrenAnand et al, 2000). Given this background we have conducted a placebo-controlled, double-blind treatment trial with lamotrigine in 12 patients suffering from DPD, and results will be reported shortly. Open clinical use has yielded promising results with a combination of lamotrigine and antidepressant medication.
We have also attempted to develop non-pharmacological interventions. Published clinical research in this area has largely been limited to case studies of psychodynamic psychotherapy and behaviour therapy that claimed some success in alleviating symptoms. Cognitive—behaviour therapy (CBT) has been found to be highly effective in the treatment of a wide variety of psychiatric disorders, but to our knowledge no studies of CBT have been conducted with DPD. A pilot study is currently being conducted with patients who have been referred to the unit.
To date, nine patients suffering from primary DPD have been included in this study. The sample comprises seven men and two women with a mean age of 34 years, and a duration of 21 years. In the majority of cases the depersonalisation has resulted in unemployment, social avoidance and low mood. In the initial phase of treatment techniques are employed that are non-specific to the depersonalisation, but which aim to increase activity, motivation and mood (e.g. activity scheduling, graded exposure to social situations and challenging negative automatic thoughts through the use of cognitive diaries). Comorbid disorders, such as panic or obsessive—compulsive disorders, are addressed during this initial phase.
The final phase of therapy involves the use of more specific interventions. In many patients depersonalisation seems to develop as a coping mechanism to avoid painful negative emotions, which may have arisen from a variety of traumatic or aversive situations. The resulting avoidance of emotional arousal appears to lead to a global blunting of emotional response. Many sufferers state that a major goal of treatment is to regain the ability to experience emotions. Treatment involves enabling the patient to gain confidence in experiencing negative emotions by the grading of exposure to emotional arousal. A second intervention, attention training (Reference Wells, White and CarterWells et al, 1997), specifically addresses alterations in attentional focus that are apparent in depersonalisation, and that may act as maintaining factors. Attention training consists of exercises in switching, dividing and selecting attention to encourage control and focus to external, rather than internal, stimuli. This outward shift in attention may also improve the sense of connection to the external world, which people suffering from depersonalisation often lack.
Preliminary results appear promising, with improvements in general functioning and depersonalisation severity.
The future
The establishment of the depersonalisation research unit clinic has served to focus a multi-disciplinary research effort towards this under-researched psychiatric disorder. In particular, we are now in a position to report research findings that further our understanding of the neurobiological basis of the disorder and the control and subjective experience of emotional responses in general. We are also beginning to be able to offer specific treatments for patients suffering from one or more of the symptoms of depersonalisation, which will soon be amenable to controlled evaluation.







eLetters
No eLetters have been published for this article.