Attention-deficity hyperactivity disorder (ADHD) (DSM-IV; American Psychiatric Association, 1994) occurs in 3-5% of school-aged children and the number of referrals to child and adolescent psychiatric services is increasing annually. Hyperactivity in primary school aged children is a risk factor for conduct disorder (Reference Taylor, Chadwick and HeptinstallTaylor et al, 1996) and those with ADHD have a higher risk of developing substance misuse problems (Reference Goldman, Genel and BezmanGoldman et al, 1998), probably mediated through conduct disorder. The presence of ADHD has also been found to be higher in the prison population (Reference Eyestone and HowellEyestone & Howell, 1994). It is therefore imperative that children with ADHD are appropriately diagnosed and adequately treated. Stimulant medication, most commonly methylphenidate, has been found to be clearly effective in the treatment of ADHD (Reference Spencer, Biederman and WilensSpencer et al, 1996) and, for example, when the dosage is carefully tailored, shown to be superior to behavioural treatment (MTA Cooperative Group, 1999). Despite this evidence, concern about the use of stimulant medication in children continues to attract public interest, for example as high-lighted in the recent Panorama programme ‘Kids on Pills’ (April 2000).
Guidelines on the treatment of ADHD have now been produced in both the US and Europe (Reference DulcanDulcan, 1997; Reference Taylor, Sergeant and DoepfnerTaylor et al, 1998). In the UK there are no clear guidelines on who is responsible for the prescribing and monitoring of methylphenidate. Despite an increased expectation of general practitioners' (GPs) involvement in the ‘sharedcare’ of children with ADHD, little is known in relation to their views of ADHD and the prescribing and monitoring of methylphenidate. Hyperactivity has been found to be one of the presenting problems, seen by GPs, most in need of a child psychiatric service. It is also an area that GPs are most concerned about or feel least experienced in (Reference Adamson and KilleleaAdamson & Killelea, 1996). In order to develop guidelines at a service level it would be advantageous to have a better understanding of the views of GPs, thereby enabling child and adolescent mental health services (CAMHS) to work collaboratively with primary care in the management of ADHD.
The study
A questionnaire to assess GPs' views on ADHD and the use of methylphenidate was devised and sent to 221 GPs in the Swansea, Neath and Port Talbot area in South Wales between May and September 1999. The questionnaire included items on the GPs' experience and familiarity with ADHD and methylphenidate, the perception of the role of various professionals in the initiating, monitoring and prescribing of methylphenidate, whether their prescribing practice would change under different circumstances and the need for further training.
The questionnaires were sent with an explanatory letter and a prepaid envelope. Initial non-responders were sent a second questionnaire.
Findings
Of 221 questionnaires sent out, 150 responses (68%) were received. Of those responding, 30% were women and 70% were men. Eight per cent of respondents were aged 25-35 years, 50% were aged 36-45 years, 31% were aged 45-56 years and 11% over the age of 56 years. The mean length in gractice was 15.5 years.
Experience of ADHD
Eighty-five per cent of GPs had a child or children in their practice with a diagnosis of ADHD. A further 13% believed that they had a child in the practice that they suspected might have ADHD.
Only 6% had received formal training on ADHD, for example during their vocational training scheme, and a further 4.5% had attended a conference or course on the subject. However, 28.5% had read journal articles and 21% had gained information from the media, including television, magazine and newspaper articles.
Current prescribing practice
Eighty-nine per cent of GPs prescribed methylphenidate, with 98% of these being supervised by a specialist — the majority by a child psychiatrist (69%) or by child psychiatry and paediatrics (19%).
Of the 11% who did not prescribe, reasons given included not having enough experience or knowledge of the drug, with only one GP stating it should not be used at all and no one giving cost as the reason for not prescribing.
The role of professionals
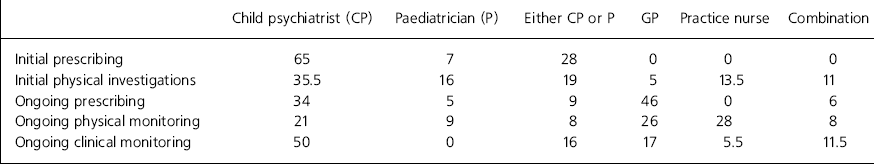
Perception of the role that various professionals, namely child psychiatrists, paediatricians, GPs and practice nurses, can play in the initiation, monitoring and regular prescribing of methylphenidate is shown in Table 1.
Table 1. General practitioners' (GPs) views of which professionals should have the primary responsibility for different aspects of care (%)
| Child psychiatrist (CP) | Paediatrician (P) | Either CP or P | GP | Practice nurse | Combination | |
|---|---|---|---|---|---|---|
| Initial prescribing | 65 | 7 | 28 | 0 | 0 | 0 |
| Initial physical investigations | 35.5 | 16 | 19 | 5 | 13.5 | 11 |
| Ongoing prescribing | 34 | 5 | 9 | 46 | 0 | 6 |
| Ongoing physical monitoring | 21 | 9 | 8 | 26 | 28 | 8 |
| Ongoing clinical monitoring | 50 | 0 | 16 | 17 | 5.5 | 11.5 |
Sixty-five per cent of GPs felt that a child psychiatrist should initiate prescribing, with no GPs believing that they should start a child on methylphenidate themselves. The majority also felt that initial physical investigations should be conducted by a specialist — either a child psychiatrist (35.5%), a paediatrician (16%) or in combination (19%).
However, only 34% thought that a child psychiatrist should continue prescribing thereafter, with 46% of GPs happy to take over sole prescribing and a further 6% in combination with secondary care.
With reference to ongoing physical monitoring, 54% of GPs felt that the primary care team could perform this, with only 21% believing this was a role for the child psychiatrist.
In contrast, most GPs (66%) felt that clinical monitoring should be carried out by secondary care professionals (child psychiatrist, either individually or in combination with a paediatrician), with only 22.5% believing it could be carried out by the primary care team alone.
Factors influencing prescribing practice among GPs
Sixty-four per cent felt that they would change their views on prescribing if there was clearer advice from specialists, with 67% stating that they would be influenced if there was a clear protocol on monitoring while a child was on medication.
Training
Eighty-four per cent felt they wanted further training in ADHD in general and 88% wanted training specifically in the drug treatment of ADHD. The majority expressed a preference for this to be delivered by a tutorial or lecture (68%), with 27% requesting written information, 5% felt advice on the telephone would be sufficient.
Discussion
The response rate of the survey was 68%, which is encouraging for a postal survey, particularly for GPs — who frequently feel that they are swamped by questionnaires (Reference Macpherson and BissetMacPherson & Bisset, 1995). This may indicate that the management of ADHD in general practice is topical, relevant and important. The high number of respondents who had a child/children with ADHD or suspected ADHD in their practice supports this view.
With reference to the use of methylphenidate, nearly all respondents believed that initial prescribing should be by a specialist, a view supported by Levy (Reference Levy1997). However, almost half (46%) of GPs then felt happy to take over prescribing once a child was stabilised on methylphenidate. In a study of child psychiatrists with a special interest in ADHD, 87% felt that GPs could continue prescribing until the next specialist review (Reference Sayal and TaylorSayal & Taylor, 1997).
With physical monitoring (such as height, weight, blood pressure and blood tests, where necessary), 70.5% of GPs felt this should be performed by a specialist initially, but thereafter the majority of respondents concluded that it could be carried out in primary care, with 28% indicating that the practice nurse could perform this.
In contrast, most GPs perceived that clinical monitoring is the domain of secondary care, generally the child psychiatrist.
It is interesting that among the GPs who did ot prescribe methylphenidate at all, cost did not feature as a reason and only one felt that methylphenidate should not be part of the treatment package for ADHD. The most common reasons for not prescribing were either a lack of knowledge or experience about the drug. This highlights the need for more training in ADHD and in the use of medication, which is supported by the findings in this study that showed that 84% of respondents would value further training in the former and 88% in the latter. Few had received any formal training on ADHD, although more had read relevant journal articles. A significant number of respondents had gained information from the media, which could be misleading or biased depending on the source.
In order to treat children with ADHD effectively there needs to be consensus on optimal management and it is important that GPs are involved in this discussion. In a climate where GPs are feeling under increased pressure, there is the danger that they will not want to contribute to the management of often difficult and complex cases as seen in mental health services (Reference Watters, Gannon and MurphyWatters et al, 1994). This view was supported by additional comments, for example, “GPs will be asked to take over yet another duty monitoring and clinical supervision programme — marvellous idea for the secondary sector doctor but it never comes with resources” and “my workload is overwhelming, I do not have the time or resources to monitor yet another new specialist treatment”. However, many comments included the general principle of “diagnosis and initial prescribing done by the child psychiatrist or specialist, then shared-care for monitoring with consultant advice readily available”. As suggested by one GP, “to empower GP colleagues as partners in the management” could be the way forward in devising management strategies that would satisfy all professionals.
Although the survey was of only one area of the UK, it suggests that CAMHS needs to provide training for GPs and actively engage in discussions of shared-care for the management of ADHD.
Limitations of the study
The study included only one area of the country and therefore may not represent the views of GPs in general. There may also be a bias of interest, as 32% did not respond and these may be GPs who have differing views to the respondents.
Acknowledgements
I wish to thank all the GPs for their participation.






eLetters
No eLetters have been published for this article.