Until recently people with mental health problems in crisis had few options other than admission to an acute ward. However, falling bed numbers have restricted even this option (Reference Hodgson and BoardmanHodgson & Boardman, 1996). Audits of acute units indicate that between 29% and 42% of patients could be accommodated more appropriately elsewhere (Reference Flannigan, Glover and FeeneyFlannigan et al, 1994; Reference Beck, Croudace and SinghBeck et al, 1997). Shepherd et al (Reference Shepherd, Beardsmore and Moore1997) indicated that increasing the number of acute psychiatric beds would not necessarily result in an enhanced service. As a result, there is an increasing recognition of the need to provide a ‘spectrum of care’ (Department of Health, 1996). However, there are few publications describing and evaluating residential alternatives to acute psychiatric wards (Reference Boardman, Hodgson and LewisBoardman et al, 1999).
Stroul (Reference Stroul1988) has suggested that crisis housing should fulfil a number of roles including the provision of short-term accommodation. The accommodation should only serve small groups of clients and it should provide an alternative to hospitalisation. The interpretation of these criteria can lead to apparently differing provision. For example, Bond et al (Reference Bond, Witheridge and Wasmer1989) described and evaluated two crisis housing schemes in Chicago. One service had a dedicated eight-bedded facility and the other relied on renting accommodation in hotels and boarding houses. The emphasis was on a cost outcome, which revealed no significant difference between the two services. The authors noted a high staff turnover and suggested that this was related to the stressful nature of the work.
Brunswick House
Brunswick House is the hub of North Staffordshire's Safe Spaces Network and became fully operational in January 1999. The house is of normal domestic stock and is sited centrally in Hanley, Stoke-on-Trent. The accommodation comprises four bedrooms, kitchen, lounge and dining area. It offers communal facilities for meals and refreshments at no cost to the resident. The house is staffed and managed by the Potteries Housing Association. Six professionals from the non-statutory sector staff the unit, with two staff members being on duty at any time. Both recreational and therapeutic activities are offered and include arts, crafts and relaxation techniques. The unit is open only between 13.00 h on Friday and 13.00 h on Monday. These hours are extended over the Christmas period. The restricted operational hours were chosen to emphasise the role of Brunswick House as a crisis centre rather than as a unit offering respite, and to respond to a perceived service gap: users indicated that the weekend was the most difficult time to cope with if they were in crisis. There are other services in North Staffordshire for those who need interventions over a longer time-scale. The target population are people with mental health problems who are known to social or health services and who are in acute crisis. Professional keyworkers normally make referrals, self-referrals are generally only accepted from those who have previously used the unit. Staff and service users take their meals together, offering clients the opportunity to benefit from this social activity.
Although Brunswick House was not commissioned specifically to offer a direct alternative to acute ward admission, our hypothesis was that it would reduce the use of acute wards for those in crisis with mental health problems. We set out to investigate the impact of Brunswick House on the use of psychiatric acute wards and accident and emergency services.
Method
The sample consisted of all Brunswick House service users between March 1999 and December 1999. A mirror design was employed, using a 1-year time frame before and after the first admission to Brunswick House. Data on admissions to acute psychiatric wards were collected from Korner returns (Reference Hodgson, Lewis and BoardmanHodgson et al, 2000). Attendances to the area's only accident and emergency department for mental health-related problems were obtained from a local case register. Costs were based on 1997 figures for North Staffordshire (Reference Haycox, Unsworth and AllenHaycox et al, 1999). Also, data were collected on the outcome of users who could not be accommodated when they requested admission to Brunswick House. These were derived from examination of accident and emergency records in the month preceding and following the failure to accommodate. Data analysis was carried out using the Statistical Package for the Social Sciences version 7.5.
Results
Sixty-four people were admitted to Brunswick House in the study period. Of these, 58 could be identified in sufficient detail to allow further data collection. Twenty-three (39%) were women and 35 (61%) were men. The mean age was 39 years (range 21-65 years). Diagnostic information was available on 49 users (Table 1). Patients with schizophrenia and personality disorder accounted for most admissions.
Table 1. Primary diagnosis for Brunswick House users

| Primary diagnosis | n = 49 (%) |
|---|---|
| Anxiety and non-psychotic affective disorders | 7 (14) |
| Affective psychoses | 2 (4) |
| Schizophrenia and allied states | 18 (37) |
| Personality disorders | 14 (29) |
| Substance misuse | 6 (12) |
| Learning disability | 2 (4) |
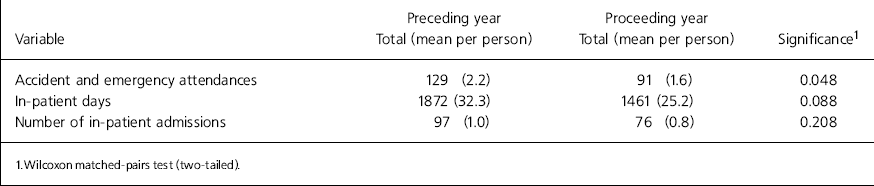
In the study period Brunswick House provided 620 bed days with a mean occupancy period of 10.7 days. There were 217 admissions (mean 3.7 per person). Bed occupancy was 100% at the start of the study period and throughout it. Less than half the sample (48.3%) used the accident and emergency department in the study period for mental health problems. There was a 30% reduction in number of attendances in the following year. This reduction was statistically significant at 6 months (Wilcoxon signed ranks, Z=-1.973, P=0.048) but not at 1 year (Table 2). Forty-three per cent of users were admitted to acute psychiatric wards, with a reduction in in-patient stays of 411 days (Table 2). The actual number of admissions fell by 22%.
Table 2. Use of NHS facilities
| Variable | Preceding year Total (mean per person) | Proceeding year Total (mean per person) | Significance1 |
|---|---|---|---|
| Accident and emergency attendances | 129 (2.2) | 91 (1.6) | 0.048 |
| In-patient days | 1872 (32.3) | 1461 (25.2) | 0.088 |
| Number of in-patient admissions | 97 (1.0) | 76 (0.8) | 0.208 |
Thirty-six people could not be accommodated when they requested admission during the first operational year. This is an underestimate, as it does not include informal enquiries. As Brunswick House is a crisis facility we examined accident and emergency records to ascertain any direct consequence of an inability to accommodate. For these 36 people there were five accident and emergency department contacts in the month following the failure to accommodate them at Brunswick House. However, there were also five contacts in the month preceding the failure to obtain accommodation. There was no recorded act of deliberate self-harm in the initial week after such failure, nor was there any admission to a psychiatric ward within that period.
During the study period there was no episode of serious deliberate self-harm or act of violence to either other people or property at Brunswick House. There were three episodes of superficial wrist scratching. One resident was banned for persistent substance misuse. There was no suicide in the study period. One resident was admitted to an acute psychiatric ward directly from Brunswick House following an assessment under the 1983 Mental Health Act. The service was less likely to be used by people living more than 8 km from Brunswick House and by people from ethnic minorities.
Using costing from Haycox et al (Reference Haycox, Unsworth and Allen1999), the direct cost to the NHS (acute psychiatric bed use and attendance at accident and emergency costs) was £195 456 in the preceding year. The cost in the following year was £152 443, representing a reduction of £43 013. In reality the cost difference is likely to be greater, as we were unable to factor in the cost of subsequent medical admission or psychiatric liaison service use following attendance at the accident and emergency department. However, the running costs for Brunswick House in the first operational year were £125 000.
Discussion
The results of this study must be interpreted with caution, as the design is naturalistic and retrospective. The use of residents as their own controls may result in an apparent improvement in service utilisation due to regression towards the mean if the resident's first admission was during a particularly bad period for that individual. However, randomised, controlled trials of facilities such as Brunswick House are likely to remain impractical for a variety of reasons. Given the relatively small numbers of residents, such a trial would require collaboration between a number of crisis houses, all of which would have to operate in a similar manner. Nevertheless, Brunswick House appears to offer safe, acceptable accommodation to those in crisis. It is an attractive alternative to seeking admission to an acute ward for many users, as demonstrated by the reduction in acute bed use. Our evaluation started within a month of Brunswick House becoming fully operational. Within the first few months a number of people with schizophrenia in the later stages of relapse were accommodated in an effort to avoid their hospitalisation. In these cases the patients were subsequently transferred directly to an acute psychiatric ward from Brunswick House. With the benefit of experience, patients in a similar position are now less likely to be accommodated. These few patients heavily bias the results and their inclusion (to a certain extent) balances the regression towards the mean argument. There is also a reduction in accident and emergency attendance, which may be a consequence of the acceptability of Brunswick House to those with self-harming behaviours. The absence of serious self-harming behaviour and violence to others while at Brunswick House contrasts with the prevalence of such behaviours on acute wards. This cannot be accounted for solely by admission bias, as many prolific self-harming patients have been accommodated at Brunswick House. Indeed, this observation has led to the development of a self-help group for people with this problem, based at Brunswick House.
Since it opened Brunswick House has been fully occupied, and an increasing number of potential users have not been accommodated. As a result restrictions have been placed on the number of times a person can be accommodated in a year. This has led to many previous residents receiving telephone support from Brunswick House staff. These pressures have resulted in discussions about opening another crisis house in the county. Even though the unit is fully occupied, efforts have been made to attract ethnic minority users who are significantly underrepresented. Our results and the increased demand for accommodation at Brunswick House suggest that the unit provides a valuable service to the people of North Staffordshire and demonstrates an effective partnership between non-statutory and statutory services.
Declaration of interest
None.







eLetters
No eLetters have been published for this article.