Use of combined antipsychotics is generally considered to reflect poor prescribing practice and has been termed psychiatry's ‘dirty little secret’ (Reference StahlStahl, 1999). Use is not recommended in the Royal College of Psychiatrists’ Consensus Statement (Reference ThompsonThompson, 1994). National Institute for Clinical Excellence guidance states that for schizophrenia, atypical and conventional antipsychotics should not be prescribed concurrently (National Institute for Clinical Excellence, 2002a), and nor should combinations of any antipsychotics, except clozapine augmentation when clozapine alone has proved insufficient (National Institute for Clinical Excellence, 2002b). There is a paucity of clinical trials to support the practice of prescribing antipsychotic combinations, apart from clozapine augmentation with a more tightly bound D2 receptor antagonist (Reference Freudenreich and GoffFreudenreich & Goff, 2002). A further concern is the risks posed by combined antipsychotics: the possible association with torsade de pointes and sudden death, the likely increased incidence of side-effects and the potential for adverse drug interactions (Reference TaylorTaylor, 2002). Despite this, use of combined antipsychotics is common and appears to be increasing (Reference Clark, Bartels and MellmanClark et al, 2002; Reference Lelliott, Paton and HarringtonLelliott et al, 2002).
The aims of this study were to examine the reasons given by the responsible medical officer (RMO) for initiating and continuing with combined antipsychotics for ‘difficult-to-manage’ patients with schizophrenia and those with a forensic history in a tertiary referral centre. Where antipsychotic combinations were considered beneficial, we sought to determine which aspects of the patient's mental state and behaviour the RMO rated as improved.
Method
St Andrew's Hospital is a 500-bed charitable specialist psychiatric hospital. The forensic and rehabilitation service is led by four consultant psychiatrists and comprises seven wards, six of which are of low- or medium-security, for the treatment of adult patients, many of whom exhibit challenging behaviour. These patients are referred from prison or other psychiatric hospitals (including special hospitals) throughout the UK. Pharmacists examined the current prescription charts of all inpatients of this service and identified those regularly prescribed two or more antipsychotics. For patients prescribed combined antipsychotics, the RMO was asked to provide an ICD-10 clinical diagnosis (World Health Organization, 1992). Consent was obtained from RMOs to take part in the study. For those patients diagnosed with schizophrenia and prescribed multiple antipsychotics, pharmacists interviewed the RMO using a structured questionnaire. Responsible medical officers were questioned about the patient's medication history, the reasons for initiating and continuing with combined antipsychotics and whether or not the patient had improved on combined antipsychotics compared with monotherapy. Detailed medication histories, including the patients’ response to treatment, were prepared by pharmacists from the patients’ medical records to assist the RMO. For each patient, the total antipsychotic dose was calculated as a percentage as follows (Reference Yorston and PinneyYorston & Pinney, 2000). Each regular prescribed dose was converted to a percentage of the British National Formulary (BNF; British Medical Association & Royal Pharmaceutical Society of Great Britain, 2002) recommended maximum dose for that drug, and then the percentages were added. If the sum exceeded 100%, the patient was considered to be receiving a high dose. Data collection complied with the Data Protection Act 1998.
Results
Of the 117 patients audited, 101 (86%) were regularly prescribed antipsychotics. Forty-one (35%) out of 117 patients were regularly receiving multiple antipsychotics. Forty of the 41 had a diagnosis of schizophrenia and these 40 formed the basis of this study. All four RMOs agreed to be interviewed.
Of the 40 patients, 35 (88%) were male and 5 (12.5%) were female. Their mean age was 37 years (range 23-56, s.d.=8.8). The mean length of stay at St Andrew's was 4.8 years (range 0.1-20.5, s.d.=4.5). Thirty-eight (95%) were detained under the Mental Health Act 1983, 24 (60%) on Section 3 and 14 (35%) under Part III of the Act. The mean length of detention under the Mental Health Act 1983 was 6.7 years (range 1-18, s.d.=4.1). Thirty-four (85%) patients were on locked wards.
Thirty-five (88%) patients were regularly prescribed two antipsychotics and five were prescribed three (13%). Fourteen (35%) were prescribed oral atypical combinations, 13 (33%) oral atypicals with oral conventionals and 13 (33%) were prescribed a depot with an oral conventional and/or an oral atypical. The most commonly prescribed antipsychotics were clozapine (18 cases; median daily dosage 550 mg, range 37.5-800 mg), olanzapine (14 cases, median daily dosage 20 mg, range 10-40 mg) and haloperidol (12 cases, median daily dosage 12.5 mg, range 5-50 mg). Twenty-four (60%) patients were prescribed high-dose antipsychotics, including 5 (13%) who were prescribed an antipsychotic at above the BNF maximum recommended dose.
For 36 (90%) patients, the RMO believed that the diagnosis was treatment-resistant schizophrenia (in most cases, documentation confirmed the patient had received sequential trials of ≥2 different antipsychotics for ≥ 8 weeks without improvement), 1 (3%) was not treatment-resistant and for 3 (8%) a full medication history was not available. Thirty-two (80%) had been prescribed clozapine and 23 (58%) had received a trial of ≥3 months of clozapine monotherapy. Ten of the 32 prescribed clozapine later refused to continue with clozapine or the associated blood tests and another two stopped clozapine because of neutropenia.
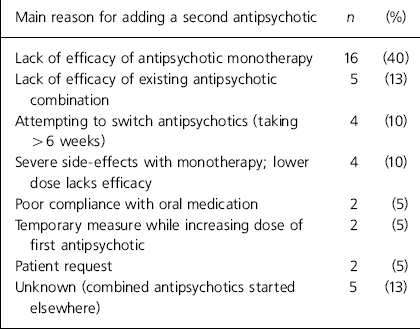
The main reason given by the RMO for adding a second antipsychotic fell into one of seven categories, but there were also five cases where the reason was unknown (see Table 1). The most common reason was lack of efficacy of monotherapy. Reasons for adding a third antipsychotic were: to calm the patient at a particular time of day (two cases), poor compliance with oral medication (two cases), and lack of efficacy of existing combined antipsychotics (one case). The RMO completed a checklist of reasons for continuing with combined antipsychotics. More than one reason could be given, and each reason could be rated as major or minor (Table 2). The main reasons were that a trial of monotherapy had given a poor outcome, and that the patient was reasonably well and stable on the current medication. Concerns about further deterioration if the regimen were changed to monotherapy, and about staff and patient safety, also featured.
Table 1. Main reason given by the responsible medical officer for adding a second antipsychotic (n=40)
| Main reason for adding a second antipsychotic | n | (%) |
|---|---|---|
| Lack of efficacy of antipsychotic monotherapy | 16 | (40) |
| Lack of efficacy of existing antipsychotic combination | 5 | (13) |
| Attempting to switch antipsychotics (taking >6 weeks) | 4 | (10) |
| Severe side-effects with monotherapy; lower dose lacks efficacy | 4 | (10) |
| Poor compliance with oral medication | 2 | (5) |
| Temporary measure while increasing dose of first antipsychotic | 2 | (5) |
| Patient request | 2 | (5) |
| Unknown (combined antipsychotics started elsewhere) | 5 | (13) |
Table 2. Reasons given by the responsible medical officer for continuing to prescribe combined antipsychotics (n=40)

| Major reason | Minor reason | |||
|---|---|---|---|---|
| Reason | n | (%) | n | (%) |
| Trial of monotherapy gave poor outcome | 17 | (43) | 7 | (18) |
| Patient reasonably well and stable; no reason to change medication | 14 | (35) | 11 | (28) |
| Patient not well; concern about further deterioration if the regimen were changed to monotherapy | 12 | (30) | 10 | (25) |
| Difficult and assaultive patient; safety concerns | 10 | (25) | 10 | (25) |
| Very serious nature of index offence | 6 | (15) | 4 | (10) |
| Severe side-effects on higher dose of monotherapy | 6 | (15) | 1 | (3) |
| Prolonged attempt (>6 weeks) to switch antipsychotics | 3 | (7) | 3 | (8) |
| Patient preference for current medication | 3 | (7) | 3 | (8) |
| Need to calm the patient at a particular time of day | 2 | (5) | 2 | (5) |
For 29 patients, the RMO was able to compare mental state and behaviour on combined antipsychotics with the most efficacious monotherapy previously prescribed. The patient was rated as better overall on combined antipsychotics than monotherapy in 26 cases (90%), no different in 1 case (3%) and better on monotherapy in 2 cases (7%). For the 26 cases where combined antipsychotics were rated as superior, the RMO said the patient had improved as follows: fewer positive symptoms (24 cases, 92%), less disturbed behaviour (19; 73%), less aggression (15; 58%), improved overall functioning (14; 54%), fewer side-effects (9; 35%) and fewer negative symptoms (8; 31%).
Discussion
Use of combined antipsychotics was common in the population surveyed (35%). This group of patients poses a therapeutic challenge. They are tertiary referrals who have required treatment under Section 3 (a minority had been referred from the courts) for several years in conditions of low- or medium-security because of disturbed behaviour. For most patients, documentation confirmed treatment-resistance (most had been tried on a large number of different antipsychotics) and 80% had been tried on clozapine (45% currently on clozapine and 35% no longer on clozapine, mainly because of intolerance or refusal). Lack of efficacy of monotherapy was the prime reason for prescribing antipsychotic combinations, as was reported by two studies of combined antipsychotics in out-patients (Reference Taylor, Mir and MaceTaylor et al, 2002; Reference Tapp, Wood and SecrestTapp et al, 2003). In our study, the RMOs reported that in most cases combined antipsychotics had brought improvements over monotherapy. In addition, some patients receiving clozapine were thought to have benefited from the addition of a second antipsychotic, as this had enabled the dose of clozapine to be reduced, leading to a reduction in side-effects (e.g. resolution of secondary diabetes mellitus). This study cannot, and does not, purport to offer evidence for the efficacy of combined antipsychotics. It is not a therapeutic trial, but a retrospective survey of the RMO's reasons and opinions. Although the RMOs reported combined antipsychotics to be beneficial, they had not carried out objective ratings to confirm this.
In this survey, 60% of patients prescribed combined antipsychotics met the study definition of high-dose treatment. Had we included when required prescriptions in the calculation the proportion would have been even higher. In only five instances was an individual antipsychotic being prescribed at above its BNF maximum recommended dosage. One danger of prescribing combined antipsychotics is that covert prescription of high dosages may occur without full staff or patient knowledge or without appropriate monitoring.
The problem facing clinicians is that there is virtually no evidence base for the efficacy of combined antipsychotics. Indeed, there is great difficulty in carrying out good studies in this area. The patients in this study could not have been included in a clinical trial - most are unable to give informed consent and many exhibit severely disturbed and assaultive behaviour. Yet what does the clinician do when faced with such severely disturbed treatment-resistant patients? Is it ethical to breach National Institute for Clinical Excellence guidance and prescribe combined antipsychotics to patients who lack mental capacity?
Clearly, there are complex issues for the RMO and multi-disciplinary team to consider and it may be helpful to obtain a second opinion. The early use of clozapine is highly desirable, but may not be possible for all patients. Where clozapine fails, a wide range of therapeutic approaches is needed (Reference Williams, Newton and RobertsWilliams et al, 2002). If all evidence-based treatments have been explored without a satisfactory clinical response, it may be reasonable to carry out a time-limited therapeutic trial, preferably using rating scales, of an antipsychotic combination. An alternative approach, similarly lacking an evidence base, would be to increase the dose of a single antipsychotic into the high-dose range. However, the numbers of patients for whom these actions are justifiable are likely to be small (Reference TaylorTaylor, 2002).
Declaration of interest
None.
Acknowledgements
We thank the consultants and pharmacists at St Andrew's Hospital for their assistance with data collection and Professor T. R. E. Barnes for his comments on the manuscript.







eLetters
No eLetters have been published for this article.