In recent years, psychological therapies have become an integral component of Government strategy for mental health (Mental Health National Service Framework: Department of Health, 2000). In this context, cognitive therapy has been cited as the preferred treatment for a wide range of mental health problems (Department of Health, 2001). The Royal College of Psychiatrists (1997) holds that all psychiatrists should have some knowledge and understanding of cognitive therapy.
In line with the above policies, it is becoming increasingly common for psychiatrists to undergo indepth training in cognitive therapy. A recent survey of graduates from the year-long cognitive therapy diploma course in Newcastle found that of 52 graduates, 17 were doctors; four (8%) were general practitioners and 12 (23%) were psychiatrists (Reference Ashworth, Williams and BlackburnAshworth et al, 1999).
The extent to which cognitively trained psychiatrists apply cognitive therapy skills remains unclear. Ashworth et al (Reference Ashworth, Williams and Blackburn1999) found that doctors saw significantly fewer clients for cognitive therapy as compared with other professional groups that underwent identical training. Le Fevre & Goldbeck (Reference Le Fevre and Goldbeck2001) surveyed cognitive therapy practice among all Scottish consultant psychiatrists. They reported that 39 of 268 (15%) carried out formal cognitive-behavioural therapy, but that only 12 (4%) were able to devote more than 2 hours to this activity.
Neither Ashworth et al (Reference Ashworth, Williams and Blackburn1999) nor Le Fevre and Goldbeck (Reference Le Fevre and Goldbeck2001) enquired as to whether psychiatrists are using their cognitive training in areas other than clinical practice. Our aim was to examine how psychiatrists trained to be cognitive therapists apply cognitive therapy skills clinically and in other areas of work.
Method
The British Association for Behavioural and Cognitive Psychotherapies (BABCP) have established stringent minimum training standards for accreditation of cognitive therapists. These standards include taking part in a minimum of 450 hours training, of which 50% must be skills-based; having a minimum of 200 hours of supervised assessment and therapy; seeing a minimum of eight clients for therapy; and maintaining an agreed level of continuing professional development. All psychiatrists living in the UK and accredited by the BABCP were asked to complete a postal questionnaire similar to that developed by Ashworth et al (Reference Ashworth, Williams and Blackburn1999) but including additional questions on non-clinical use of cognitive therapy. We enquired about demographic details; training in cognitive therapy; impact of cognitive therapy training on development of posts; use of cognitive therapy clinically and in other areas of practice; and finally about the views of psychiatrists on the desirability of cognitive therapy training for psychiatric trainees.
After 4 weeks, addresses of non-respondents were cross-checked, and reminders were sent. Results were analysed using the Statistical Package for the Social Sciences (SPSS version 10).
Results
A total of 35 psychiatrists are currently accredited members of the BABCP and are living in the UK or Ireland. Of these 33 (94%) returned the questionnaire, of whom 17 (52%) were female. These formed the study population.
Respondents had been practising cognitive therapy for a median of 7 years (inter-quartile range (IQR)=6-12 years), although it is unclear whether this period was all following training. Twenty-six respondents (79%) held consultant posts, of whom 15 were in specialised psychotherapy posts and 17 were working in other areas (including general adult, liaison and child and adolescent psychiatry). One respondent did not provide information on this parameter. A total of 20 (52%) had obtained a diploma in cognitive therapy, whereas the remainder fulfilled BABCP requirements through a combination of various courses and supervision.
In terms of the impact on their job, 12 (37%) respondents indicated that their current post had developed on account of training in cognitive therapy. One example given was acting as a tutor in cognitive therapy to senior house officers. Seven respondents (21%) stated that they had changed posts because of their cognitive therapy training, either to work in psychotherapy, or in one case, to work in private practice. Another three respondents indicated that they were currently looking for posts in psychotherapy.
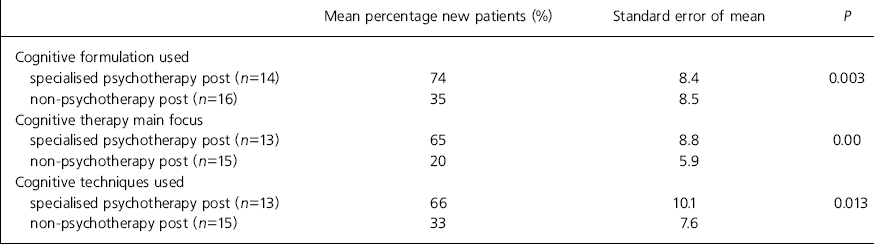
Respondents were seeing between 0 and 30 new patients a month (median=10; IQR 6-15). A cognitive formulation was used in 55% of patients on average, and cognitive therapy was described as the main focus of treatment in 43% of cases. There were, however, significant differences between subgroups - respondents in psychotherapy posts made significantly more use of cognitive therapy, cognitive therapy formulation and specific cognitive therapy skills (Table 1). Respondents in non-psychotherapy posts were also significantly less satisfied with the extent to which they were able to use their cognitive therapy skills: 4 of 17 (24%) were satisfied, compared with 12 of 15 (80%) of those in psychotherapy posts (Fisher’s exact test: P=0.002). In response to an open question about the reason for not using cognitive therapy, respondents emphasised lack of protected time and pressure of other clinical commitments.
Table 1. Comparison of use of cognitive therapy in clinical practice: psychiatrists in psychotherapy posts v. others
| Mean percentage new patients (%) | Standard error of mean | P | |
|---|---|---|---|
| Cognitive formulation used | |||
| specialised psychotherapy post (n=14) | 74 | 8.4 | 0.003 |
| non-psychotherapy post (n=16) | 35 | 8.5 | |
| Cognitive therapy main focus | |||
| specialised psychotherapy post (n=13) | 65 | 8.8 | 0.00 |
| non-psychotherapy post (n=15) | 20 | 5.9 | |
| Cognitive techniques used | |||
| specialised psychotherapy post (n=13) | 66 | 10.1 | 0.013 |
| non-psychotherapy post (n=15) | 33 | 7.6 |
With regards to using cognitive therapy skills in non-clinical areas, 28 (85%) respondents stated that they were involved in supervision and in teaching; 26 (79%) agreed their training had improved their ability to select patients for cognitive therapy and 14 (42%) believed that training also had an impact on referrals for other forms of psychotherapy. A total of 19 (58%) respondents described an impact on service development, e.g. setting up a new programme for eating disorders. There were 15 (46%) respondents who felt that training in cognitive therapy had changed their prescribing patterns. Many comments indicated that respondents felt more able to offer alternatives to medication.
All respondents except one described themselves as accessing some form of continuous professional development in cognitive therapy. A total of 29 (88%) respondents said that they were reading in the field and 28 (85%) were benefiting from ongoing supervision (usually in a multidisciplinary setting). Thirty-one (94%) respondents reported that they were attending conferences and workshops in cognitive therapy.
There were 25 (76%) psychiatrists who believed that training in cognitive therapy is desirable for trainees and seven (21%) felt it should be compulsory. Many respondents added comments to the effect that such training is invaluable in terms of improving understanding and in forming collaborative relationships with patients, even when formal cognitive therapy is not undertaken.
Discussion
Psychiatrists appear to use cognitive techniques with a substantial minority of patients but, unless in full-time psychotherapy posts, they spend little time in the formal practice of cognitive therapy. Despite the limitations on their clinical practice, respondents see themselves as having a significant role in teaching, training and supervision of cognitive therapy. Respondents find training in cognitive therapy useful but those in non-psychotherapy posts are frustrated by the lack of opportunity to use their skills.
These findings reflect those reported previously in the literature (Reference Ashworth, Williams and BlackburnAshworth et al, 1999; Le Fevre et al, 2001) but provide added information on non-clinical areas in which psychiatrists use their cognitive therapy training. It could be questioned whether psychiatrists should play a major role in teaching, training and supervising colleagues in a modality that they do not habitually use.
The 94% response rate in this study is high for a postal survey and suggests that the findings are likely to be representative of psychiatrists who are accredited members of the BABCP. Nevertheless, numbers surveyed are small and findings are based upon self-reporting. High levels of cognitive dissonance might render negative appraisal of the value of cognitive training difficult, given extensive investment in such training.
Psychiatrists who are accredited members of the BABCP might not be representative of other psychiatrists who have also completed formal training in cognitive therapy. However, the BABCP is the main regulating body for cognitive therapy in the UK. It seems likely that those psychiatrists who are sufficiently motivated to become accredited members would also be particularly well motivated to practise cognitive therapy. In this respect, the finding of significant obstacles to the practice of cognitive therapy by psychiatrists is worrying.
Conclusion
Although our sample was highly selected, we hope this study raises interesting questions about the way in which cognitive therapy training for psychiatrists could impact on service delivery. Even if many psychiatrists do not practise cognitive therapy in a formal way, could cognitive therapy skills have a significant effect on clinical practice? Further research might profitably look at patient satisfaction and patient-clinician relationship in the year prior to, and after, completion of cognitive therapy training. Such information would help individual clinicians and the health service to decide if extensive investment in cognitive therapy training for psychiatrists is likely to be worthwhile.
Acknowledgement
With thanks to Mr Howard Lomas, secretary of the BABCP, for his enthusiastic help in identifying psychiatrists accredited by the BABCP.






eLetters
No eLetters have been published for this article.