Smoking and substance misuse during pregnancy are known to adversely affect foetal outcome by a reduction in birth weight associated with intra-uterine growth retardation, preterm birth and an increased rate of perinatal death (Reference BennedsenBennedsen, 1998). It is also known that psychiatric patients smoke more than other patients or the general public (Reference McCreadieMcCreadie, 2002) and that women with schizophrenia have an increased risk of obstetric and perinatal complications (Reference Sacker, Done and CrowSacker et al, 1996; Reference BennedsenBennedsen, 1998; Reference Howard, Goss and LeeseHoward et al, 2003). This increased risk has not been definitively accounted for; it is not known whether lifestyle differences such as smoking and substance misuse are explanatory, whether psychotropic medication is the causal factor or whether it is a result of genetic factors. There is only limited evidence supporting the assertion that pregnant women with mental illness are more likely to smoke and misuse substances than other pregnant women (Reference Maughan, Taylor and CaspiMaughan et al, 2004), so we decided to investigate this at a routine antenatal clinic.
Method
Women were identified from computer records as having booked their pregnancies during the period January 2001 to December 2002. Women with a psychiatric history according to the computer records were matched for age with a control group who had no psychiatric history. Information recorded included demographic data, obstetric and psychiatric history, and smoking and alcohol intake. Marital status was obtained from the booking record, but this did not specify whether unmarried partners were cohabiting. We were therefore unable to include this variable owing to the inaccuracy of these data.
Data analysis was carried out using Stata version 6 for Windows; P values are all two-tailed. A descriptive analysis was carried out.
Results
Booking data were recorded for 156 women (mean age 30.1 years, s.d.=6). Psychiatric diagnosis was recorded by midwives and is given in Table 1. The psychotropic medications taken by the women at the time of booking were selective serotonin reuptake inhibitors (n=11, 14.4%), tricyclic antidepressants (n=3, 4.0%), antipsychotic drugs (n=2, 2.6%), mood stabilisers (n=3, 4.0%) and others (n=2, 2.6%). None of the women was taking atypical antipsychotic medication.
Table 1. Psychiatric diagnoses (n=76)

| Psychiatric diagnosis | n (%) |
|---|---|
| Depression | 47 (62) |
| Bipolar affective disorder | 2 (3) |
| Schizophrenia | 0 (0) |
| Schizoaffective disorder | 3 (4) |
| Postnatal depression | 10 (13) |
| Substance misuse | 4 (5) |
| Eating disorder | 4 (5) |
| Anxiety disorder | 3 (4) |
| Other psychotic illness | 2 (3) |
| Puerperal psychosis | 1 (1) |
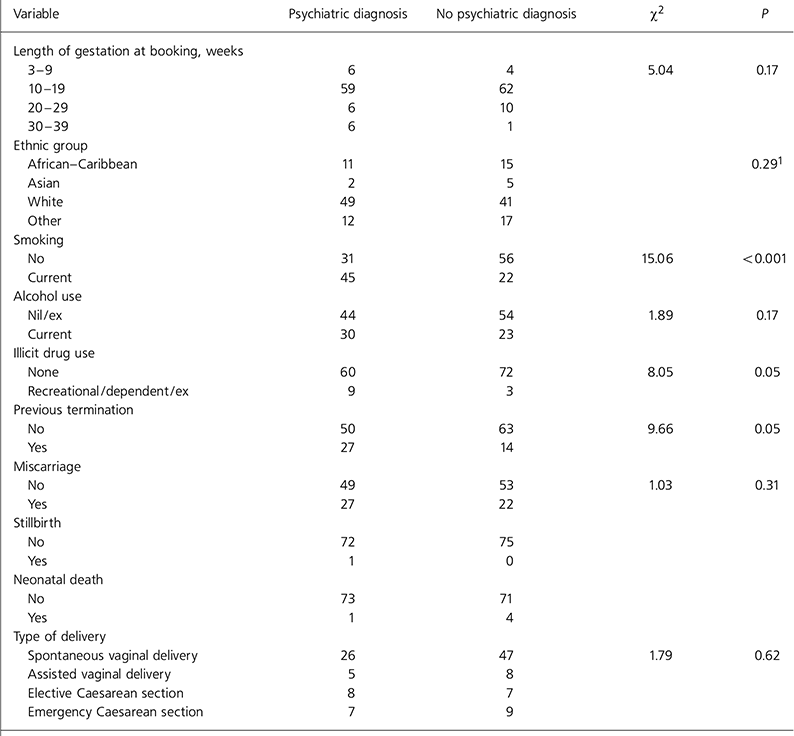
There was no significant difference in ethnicity between women with and without a psychiatric diagnosis. Weeks of gestation at the time of booking did not differ significantly, but more very late bookers had a diagnosis of mental illness (Table 2). Women with a psychiatric diagnosis were significantly more likely to be smokers (P<0.001), although the smokers in each group did not differ significantly in the amount smoked (Kruskal-Wallis test P=0.55). The median number of cigarettes consumed per day was 10 (interquartile range 5-15).
Table 2. Variables in pregnant women with and without a psychiatric diagnosis
| Variable | Psychiatric diagnosis | No psychiatric diagnosis | χ 2 | P |
|---|---|---|---|---|
| Length of gestation at booking, weeks | ||||
| 3-9 | 6 | 4 | 5.04 | 0.17 |
| 10-19 | 59 | 62 | ||
| 20-29 | 6 | 10 | ||
| 30-39 | 6 | 1 | ||
| Ethnic group | ||||
| African-Caribbean | 11 | 15 | 0.291 | |
| Asian | 2 | 5 | ||
| White | 49 | 41 | ||
| Other | 12 | 17 | ||
| Smoking | ||||
| No | 31 | 56 | 15.06 | < 0.001 |
| Current | 45 | 22 | ||
| Alcohol use | ||||
| Nil/ex | 44 | 54 | 1.89 | 0.17 |
| Current | 30 | 23 | ||
| Illicit drug use | ||||
| None | 60 | 72 | 8.05 | 0.05 |
| Recreational/dependent/ex | 9 | 3 | ||
| Previous termination | ||||
| No | 50 | 63 | 9.66 | 0.05 |
| Yes | 27 | 14 | ||
| Miscarriage | ||||
| No | 49 | 53 | 1.03 | 0.31 |
| Yes | 27 | 22 | ||
| Stillbirth | ||||
| No | 72 | 75 | ||
| Yes | 1 | 0 | ||
| Neonatal death | ||||
| No | 73 | 71 | ||
| Yes | 1 | 4 | ||
| Type of delivery | ||||
| Spontaneous vaginal delivery | 26 | 47 | 1.79 | 0.62 |
| Assisted vaginal delivery | 5 | 8 | ||
| Elective Caesarean section | 8 | 7 | ||
| Emergency Caesarean section | 7 | 9 |
Women with a psychiatric diagnosis were not significantly more likely to drink alcohol, although a trend was observed (P=0.17). The median number of units consumed per week was 3 (interquartile range 2-4). Twelve women had a history of current or previous illicit drug use, and these were significantly more likely to have a psychiatric diagnosis (P=0.05). Those with a psychiatric history were significantly more likely to have a history of previous termination of pregnancy (P=0.05), although there was no difference in history of miscarriage, stillbirth or neonatal death. Mode of delivery was compared between the two groups but no significant difference was found.
Discussion
We demonstrated a strong association between psychiatric history and smoking in pregnant women. We also found a significant association of psychiatric history with misuse of illicit drugs, but the numbers were small. No association was demonstrated between late booking and psychiatric history, confirming a similar finding in a UK study of women with psychotic disorders (Reference Howard, Goss and LeeseHoward et al, 2003). This may reflect the nature of healthcare delivery in the UK, which is integrated and should prevent late booking in women with psychotic disorders once they have presented to their general practitioner.
The pattern of psychiatric diagnoses identified at the time of booking does not represent the epidemiological pattern. The absence of any women with schizophrenia could be a result of altered fertility in this group (Reference Howard, Kumar and LeeseHoward et al, 2002), inaccurate recording of psychiatric diagnoses by a relatively undertrained group of health professionals, and the stigma of such diagnoses leading to their underreporting by pregnant women.
Appropriately trained midwives might be able to correctly differentiate women with a psychiatric diagnosis from those suffering milder forms of distress, which is common in pregnancy. Having identified women with a psychiatric diagnosis they would need to be aware of potential stigmatisation, which would be likely to reduce the uptake of any help offered.
Interventions for smoking cessation should be tailored to this vulnerable group: just recycling the package offered to other women smokers is unlikely to be effective. Smoking cessation programmes are known to be of limited efficacy in pregnancy (Reference ColemanColeman, 2004). Other issues such as illicit drug misuse, alcohol misuse, misuse or appropriate use of prescribed psychotropic medication, and psychological or socio-economic risk factors (poor housing, lack of childcare) which may be associated with smoking and drug use might require specific intervention. It is unlikely that midwives could provide all the help required, but because the midwife is often the person who has most engaged the women, particularly when there are child protection issues resulting in distrust of mental health and social services, they could act in a liaison capacity with support services provided by other health professionals. Joint clinics between obstetricians and psychiatrists might be another opportunity for liaison between the disciplines caring for these patients.
Patient education regarding the harmful effects of smoking during pregnancy will influence the uptake of any intervention. The message that some psychotropic substances such as prescribed medication can have benefits that outweigh the risks in pregnancy must be disseminated by obstetricians, midwives and all other services involved in antenatal care. Finally, the interventions need to be appropriate for the educational level and cognitive function of the service user.
Limitations
Some information was incomplete and could not be included in the statistical analysis (marital status gave no indication of whether unmarried partners were cohabitees and the only indications of socio-economic status were address and occupation). The methodology did not account for differences in midwives' knowledge of mental illness. The stigma associated with psychiatric diagnoses might influence self-reporting of psychiatric history, especially with its implications of impaired abilities to care for the expected infant. Similarly, women might underreport smoking and other behaviours that are commonly known to impact negatively on foetal development.
Uptake of antenatal care is known to be lower in women with a history of substance misuse and therefore it is likely that there is an underrepresentation of this group. Many of the case records listed could not be found at the time of data collection, and if these notes were of more complex cases with other hospital appointments, there is the possibility of sample bias.
All data were collected by a single researcher, making it impossible to validate the reliability of the information gleaned. However, they were recorded exactly as they appeared in the midwives' booking records, were recorded on a purpose-designed form and entered onto the computer by the same researcher, thus limiting the possibility of misinterpretation.
Implications
Specific interventions to reduce smoking by pregnant women with mental illness are warranted, and would be likely to improve outcomes of pregnancy in terms of birth weight, preterm birth and neonatal morbidity and mortality. In turn, these outcomes are likely to result in increased well-being of this vulnerable group of women. Such interventions may have to be delivered opportunistically and psychiatrists may be best placed to do so. Therefore there is an onus on each of us to consider the physical well-being of our patients during pregnancy and to offer advice and education regarding smoking and other drug use.
Declaration of interest
None.







eLetters
No eLetters have been published for this article.