There are many studies examining the efficacy of antipsychotic drugs and a large number of prescribing guidelines that broadly recommend atypical antipsychotics as first-line agents for people with schizophrenia (National Institute for Clinical Excellence, 2002; Reference Lehman, Lieberman and DixonLehman et al, 2004). Recently, the Clinical Antipsychotic Trials of Intervention Effectiveness (CATIE) suggested that differences in effectiveness can be discerned, with patients more likely to stay on olanzapine compared with quetiapine and risperidone (Reference Lieberman, Stroup and McEvoyLieberman et al, 2005).
Of course clinicians cannot simply prescribe ‘atypical antipsychotics’ but need repeatedly to choose an individual drug for individual patients. In clinical situations, choice may be influenced by local guidelines or restrictions and other considerations such as cost and formulation. One possible way to obviate considerations of these non-drug factors is to ask prescribers which drug they would like to be prescribed if, in a hypothetical situation, they developed psychosis.
A previous study suggested that when 54 psychiatrists were confronted with a hypothetical situation where they, their partner or child became ill with schizophrenia 94% would choose an atypical antipsychotic medication (Reference SteinertSteinert, 2003). We aimed to update and expand this study by asking nurses, pharmacists and psychiatrists which antipsychotic they would choose if diagnosed with schizophrenia.
Method
We designed a semi-structured questionnaire to investigate factors which influence the decision process when choosing antipsychotics. We collected demographic data on grade of professional, years since qualification, gender, age and area of speciality. Participants were then asked how many patients they have seen with schizophrenia over the past year and which antipsychotic they had prescribed or, in the case of nurses and pharmacists, had most experience with. We then asked professionals to imagine a hypothetical situation in which they themselves developed schizophrenia and asked them to choose an antipsychotic for themselves. Finally they were asked to give a simple reason for their choice from seven available options: adherence, dosing, efficacy, interactions, safety, tolerability, kinetic profile and cost.
Between November 2005 and February 2006 we approached staff on in-patient wards that admit patients with schizophrenia across South London and the Maudsley NHS Foundation Trust (Southeast London) for inclusion in the study. We also approached all psychiatric pharmacists employed by the trust. Registered psychiatric nurses, senior house officers, psychiatrists and pharmacists were included in the study. We piloted the questionnaire on ten psychiatric pharmacists and amended the questionnaire for clarity. We interviewed individuals in private and participants were given the option of passing on any question they did not wish to answer.
Results
Staff on 40 wards were approached for inclusion in the study. Three wards (2 general adult and 1 forensic ward) were unable to participate because of a high workload. From the 37 participating wards, 95 registered psychiatric nurses, 30 senior house officers and 35 psychiatrists (senior registrars and consultants) were entered into the study; 28 psychiatric pharmacists also participated. No one refused to take part.
Participant characteristics are shown in Table 1. Table 2 shows the antipsychotics most often used in the health professionals’ practice.
Table 1. Participants’ characteristics

| Nurse (n=95) | Pharmacist (n=28) | Senior house officer (n=30) | Consultant and specialist registrar (n=36) | |
|---|---|---|---|---|
| Male gender, % | 35.8 | 32.1 | 40 | 82.9 |
| Age, years, mean: (range) | 39.6 (24-64) | 32 (23-52) | 31.3 (27-50) | 44.5 (32-61) |
| Years since qualification, mode | <5 | <5 | <5 | 16-20 |
| Number of patients seen per year, mode | 11-50 | > 100 | 50-100 | 11-50 |
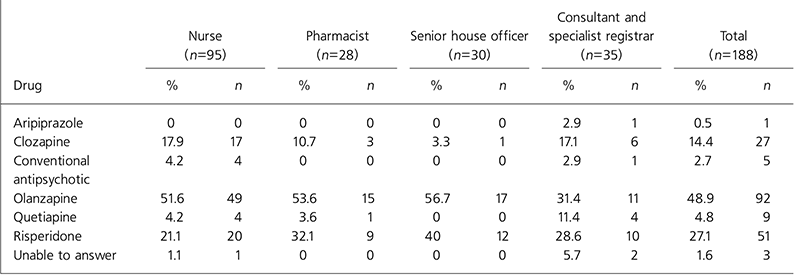
Table 2. Antipsychotic with which health professionals had the most experience
| Nurse (n=95) | Pharmacist (n=28) | Senior house officer (n=30) | Consultant and specialist registrar (n=35) | Total (n=188) | ||||||
|---|---|---|---|---|---|---|---|---|---|---|
| Drug | % | n | % | n | % | n | % | n | % | n |
| Aripiprazole | 0 | 0 | 0 | 0 | 0 | 0 | 2.9 | 1 | 0.5 | 1 |
| Clozapine | 17.9 | 17 | 10.7 | 3 | 3.3 | 1 | 17.1 | 6 | 14.4 | 27 |
| Conventional antipsychotic | 4.2 | 4 | 0 | 0 | 0 | 0 | 2.9 | 1 | 2.7 | 5 |
| Olanzapine | 51.6 | 49 | 53.6 | 15 | 56.7 | 17 | 31.4 | 11 | 48.9 | 92 |
| Quetiapine | 4.2 | 4 | 3.6 | 1 | 0 | 0 | 11.4 | 4 | 4.8 | 9 |
| Risperidone | 21.1 | 20 | 32.1 | 9 | 40 | 12 | 28.6 | 10 | 27.1 | 51 |
| Unable to answer | 1.1 | 1 | 0 | 0 | 0 | 0 | 5.7 | 2 | 1.6 | 3 |
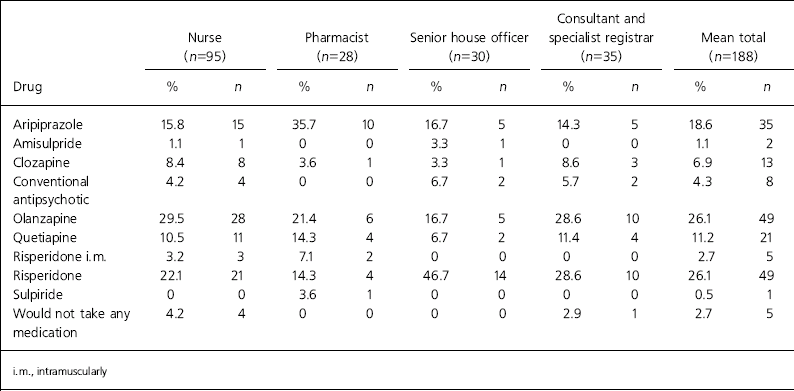
Table 3 lists the choice of antipsychotics for the hypothetical situation. Risperidone (n=49, 26.1%) and olanzapine (n=49, 26.1%) were the antipsychotics most likely to be chosen, followed by aripiprazole (n=35, 18.6%) and quetiapine (n=21, 11.2%). Only 8 participants (4.3%) would choose a conventional antipsychotic. Also of note is that 5 staff (2.7%) indicated they would not take any medication.
Table 3. Antipsychotic health professionals would choose for themselves
| Nurse (n=95) | Pharmacist (n=28) | Senior house officer (n=30) | Consultant and specialist registrar (n=35) | Mean total (n=188) | ||||||
|---|---|---|---|---|---|---|---|---|---|---|
| Drug | % | n | % | n | % | n | % | n | % | n |
| Aripiprazole | 15.8 | 15 | 35.7 | 10 | 16.7 | 5 | 14.3 | 5 | 18.6 | 35 |
| Amisulpride | 1.1 | 1 | 0 | 0 | 3.3 | 1 | 0 | 0 | 1.1 | 2 |
| Clozapine | 8.4 | 8 | 3.6 | 1 | 3.3 | 1 | 8.6 | 3 | 6.9 | 13 |
| Conventional antipsychotic | 4.2 | 4 | 0 | 0 | 6.7 | 2 | 5.7 | 2 | 4.3 | 8 |
| Olanzapine | 29.5 | 28 | 21.4 | 6 | 16.7 | 5 | 28.6 | 10 | 26.1 | 49 |
| Quetiapine | 10.5 | 11 | 14.3 | 4 | 6.7 | 2 | 11.4 | 4 | 11.2 | 21 |
| Risperidone i.m. | 3.2 | 3 | 7.1 | 2 | 0 | 0 | 0 | 0 | 2.7 | 5 |
| Risperidone | 22.1 | 21 | 14.3 | 4 | 46.7 | 14 | 28.6 | 10 | 26.1 | 49 |
| Sulpiride | 0 | 0 | 3.6 | 1 | 0 | 0 | 0 | 0 | 0.5 | 1 |
| Would not take any medication | 4.2 | 4 | 0 | 0 | 0 | 0 | 2.9 | 1 | 2.7 | 5 |
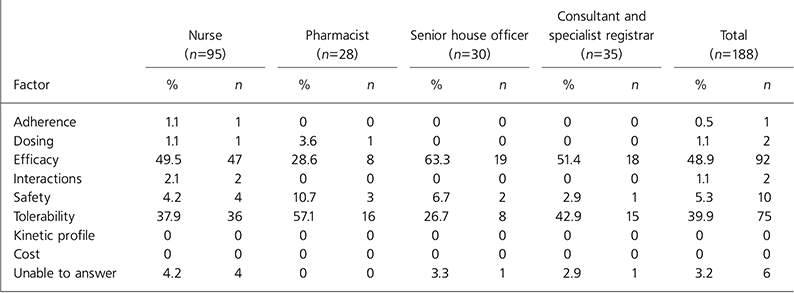
The main factors that participants considered paramount in choosing an antipsychotic for themselves are shown in Table 4. Efficacy and tolerability were most frequently reported.
Table 4. Factor considered most important in choosing antipsychotic for self
| Nurse (n=95) | Pharmacist (n=28) | Senior house officer (n=30) | Consultant and specialist registrar (n=35) | Total (n=188) | ||||||
|---|---|---|---|---|---|---|---|---|---|---|
| Factor | % | n | % | n | % | n | % | n | % | n |
| Adherence | 1.1 | 1 | 0 | 0 | 0 | 0 | 0 | 0 | 0.5 | 1 |
| Dosing | 1.1 | 1 | 3.6 | 1 | 0 | 0 | 0 | 0 | 1.1 | 2 |
| Efficacy | 49.5 | 47 | 28.6 | 8 | 63.3 | 19 | 51.4 | 18 | 48.9 | 92 |
| Interactions | 2.1 | 2 | 0 | 0 | 0 | 0 | 0 | 0 | 1.1 | 2 |
| Safety | 4.2 | 4 | 10.7 | 3 | 6.7 | 2 | 2.9 | 1 | 5.3 | 10 |
| Tolerability | 37.9 | 36 | 57.1 | 16 | 26.7 | 8 | 42.9 | 15 | 39.9 | 75 |
| Kinetic profile | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 |
| Cost | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 |
| Unable to answer | 4.2 | 4 | 0 | 0 | 3.3 | 1 | 2.9 | 1 | 3.2 | 6 |
Discussion
This study has shown that mental health professionals would largely choose olanzapine, risperidone or aripiprazole as treatments for themselves and consider efficacy and tolerability to be the most important factors in this choice. These preferences are, in some cases, in contrast to the drugs’ use in this unit; olanzapine seemed to be most often prescribed and aripiprazole was most often prescribed by very few psychiatrists.
It is notable that very few mental health professionals chose quetiapine, amisulpride or sulpiride: three popular antipsychotics in practice with a good reputation for tolerability. Also of interest is that only 5 of 188 participants claimed they would not take medication if diagnosed with schizophrenia. This is reassuring given that the prescription of antipsychotics is almost universal for this condition. It was also reassuring that professionals were willing to take drugs such as olanzapine which has profound adverse metabolic effects (Reference Lieberman, Stroup and McEvoyLieberman et al, 2005). It is also of note that many of the factors emphasised in the marketing of antipsychotics (dosing, interactions and cost) were not considered important when choosing for oneself.
In choosing an antipsychotic for themselves mental health professionals are likely to have taken into account their personal observations of the effects of the drugs as well as, perhaps to a lesser extent, published comparative data. This study asked healthcare workers to nominate what they considered to be the ‘best’ antipsychotic. The fact that very few people chose conventional agents presents support for the widespread use of the second-generation antipsychotics in practice. Interestingly, the primacy of olanzapine and risperidone in this study is in agreement with recently published effectiveness studies (Reference Volavka, Czobor and SheitmanVolavka et al, 2002; Reference Lieberman, Stroup and McEvoyLieberman et al, 2005; Reference McEvoy, Lieberman and StroupMcEvoy et al, 2006; Reference Stroup, Lieberman and McEvoyStroup et al, 2006). Each of these drugs has been shown to have effectiveness advantages over conventional antipsychotics and other drugs such as quetiapine and ziprasidone. Professionals’ choice is thus very much in line with the latest evidence on comparative effectiveness: a measure which includes efficacy and tolerability. Importantly, however, this preference for olanzapine and risperidone pre-dates publication of the most compelling evidence supporting the use of these two drugs (Reference Stroup, Lieberman and McEvoyStroup et al, 2006). Professionals’ choice of antipsychotic for themselves might therefore be a sensitive indicator of the most effective antipsychotics.
Declaration of interest
D.T. has received research funding and/or honoraria from Bristol-Myers Squibb, Sanofi-Synthelabo, Lundbeck, AstraZeneca and Novartis.









eLetters
No eLetters have been published for this article.