Nepal has a short and slowly developing history of psychiatry. Recent political turmoil has crippled Nepalese healthcare in rural areas. Although the final quarter of the 20th century saw some development of psychiatric services in Nepal, the majority of Nepalese people remain deprived of such services even today. There is no national health programme or Mental Health Act. Psychiatric services are hospital based and most are centralised in the capital. Nepalese psychiatrists need urgent help, but they have been unable to form a strong professional body. This report presents the historical background, current state of affairs and suggestions for modernising mental health services in Nepal.
The country
Nepal is a small Himalayan kingdom (desperate to be a republic) sandwiched between India and China. The United Nations classifies Nepal as one of the least developed countries in the world, with a per capita income of just £ 150. Nearly two-fifths of the population lives on less than 90p a day. It is predominantly a rural country where only 15% of the population live in urban areas. Less than 3% of gross domestic product is spent on the healthcare system and only 0.8% of the healthcare budget is spent on mental health.
Nepalese psychiatrists and other mental health professionals deserve a huge round of applause for hosting the second international conference of the South Asian Association for Regional Cooperation (SAARC) Psychiatric Federation (SPF) in Kathmandu on 17-19 November 2006. Established in 1985, the SAARC is a political and economic organisation of (currently) eight countries in southern Asia. The theme of the conference was ‘Social conflicts and mental health challenges to psychiatrists’. Delegates from the neighbouring countries had their stories to tell, ideas to share and papers to present, but Nepalese psychiatrists were conspicuous by their absence at the podium.
Mental health problems
Nepal is a rural country. The majority of its population depend on agriculture and farming. The complete absence of a social welfare net is a major obstacle to the development and delivery of mental healthcare. The approximate financial burden that falls on a family when one of its members becomes mentally ill is around 25 000 Nepalese rupees (equivalent to nearly £ 200) per year. Most people think that mental illness means becoming crazy or lunatic, being possessed by spirits or losing control of oneself (Reference REGMI, POKHREL and OJHARegmi et al, 2004). Although healthcare professionals are becoming more aware of mental health problems (Reference SHYANGWA, SINGH and KHANDELWALShyangwa et al, 2003), the majority of rural Nepalese people still believe that mental illness is caused by bad fortune.
There are no national morbidity data for mental illness either in primary or secondary care. The prevalence of mental disorders in Nepal apparently does not differ from that of other countries in the south Asia region. According to Dr Kan Tun (personal communication, 2006), the World Health Organization (WHO) representative to Nepal, around 1% of the population has severe mental illness and 10-20% milder mental health problems. A survey of two developing towns in western Nepal in 1998 revealed a high point prevalence (35%) of ‘ conspicuous psychiatric morbidity’ (Reference UPADHYAYA and POLUpadhyaya & Pol, 2003). About 2% of people with that degree of morbidity have been reported to suffer from incapacitating illnesses requiring continuous support. The current situation would certainly be different as a decade-long Maoist insurgency has caused immense social upheaval.
Janakpur Mental Health Camp
Holding ‘mobile camps’ to assess and treat patients in areas without specialist medical facilities is a common means of offering medical help in the deprived communities of low-income countries. ‘ Ashadeep’, a non-governmental organisation, provides a similar service outside Kathmandu by running free monthly mental health clinics in three districts. In January 2006, the psychiatry section of the Nepalese Doctors’Association (UK) organised a 3-day mental health camp at Janakpur, a provincial town in south-east Nepal, in collaboration with the local Red Cross Society. There is no mental healthcare for a population of over 1 million in Janakpur province. The nearest psychiatric unit is a 4-hour drive away. There were five qualified psychiatrists including the author. The event was advertised by national and local media.
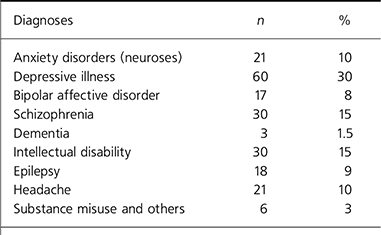
Total number of patients seen at the camp was 290, double the expected number. Data for only 202 patients were available for analysis. The majority of patients were female; there were only 90 males. The age ranged from 4 to 89 years. Table 1 describes the common clinical diagnoses and their frequency at the camp. The data are close to those reported previously (Reference NEPAL, GURUNG and JHANepal et al, 1986). A high proportion attending with epilepsy and headache (about one-fifth) simply reflects the absence of a neurological service in a country where there is no concept of family physicians.
Table 1. The nature and frequency of psychiatric illnesses in 202 patients at the Janakpur Mental Health Camp
| Diagnoses | n | % |
|---|---|---|
| Anxiety disorders (neuroses) | 21 | 10 |
| Depressive illness | 60 | 30 |
| Bipolar affective disorder | 17 | 8 |
| Schizophrenia | 30 | 15 |
| Dementia | 3 | 1.5 |
| Intellectual disability | 30 | 15 |
| Epilepsy | 18 | 9 |
| Headache | 21 | 10 |
| Substance misuse and others | 6 | 3 |
A 17-year-old girl was brought to the camp by her relatives. She exhibited classical signs of an acute manic episode. She was admitted to a medical ward, tied to the cot and treated with up to 20 mg haloperidol intra-muscularly over a period of 24 hours. The following day she became sedated and dehydrated, requiring intravenous fluid. As there is no psychiatric follow-up care available in that province, her family would have to travel several hours by public transport for psychiatric review. This scenario is not uncommon in Nepal.
Healthcare and mental health services in Nepal
Healthcare in Nepal is delivered through hospitals in the urban areas, and health centres and health posts in the rural areas. There are over 3200 physicians in Nepal - 4 per 100 000 population. During the decade-long Maoist-armed insurgency, hundreds of community health posts have been destroyed, dozens of healthcare workers have lost their lives and many fled their posts. Unfortunately, health services in Nepal are organised in such a complex and bureaucratic manner that reforming the Nepalese National Health Service would require a total culture change.
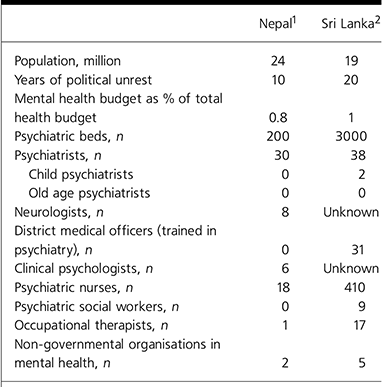
The situation of mental healthcare in Nepal is worse than in its neighbouring countries (for example Sri Lanka, which has a comparable population and an equally turbulent history, but a high health status; Reference MENDISMendis, 2004). In 1986, there were only 10 psychiatrists in Nepal. In the past 20 years, the number has trebled to 30 but is still less than in Sri Lanka which has a smaller population (Table 2). In both countries, most psychiatrists working for the government or for a university have a lucrative private practice after their contractual hours. Almost all patients prefer to seek private consultation for both general medical and psychiatric services as long as they can afford to do so financially. The most remarkable difference is in the number of psychiatric nurses, over 400 in Sri Lanka and only 18 in Nepal.
Table 2. Comparison of mental health services in Nepal and Sri Lanka
| Nepal1 | Sri Lanka2 | |
|---|---|---|
| Population, million | 24 | 19 |
| Years of political unrest | 10 | 20 |
| Mental health budget as % of total health budget | 0.8 | 1 |
| Psychiatric beds, n | 200 | 3000 |
| Psychiatrists, n | 30 | 38 |
| Child psychiatrists | 0 | 2 |
| Old age psychiatrists | 0 | 0 |
| Neurologists, n | 8 | Unknown |
| District medical officers (trained in psychiatry), n | 0 | 31 |
| Clinical psychologists, n | 6 | Unknown |
| Psychiatric nurses, n | 18 | 410 |
| Psychiatric social workers, n | 0 | 9 |
| Occupational therapists, n | 1 | 17 |
| Non-governmental organisations in mental health, n | 2 | 5 |
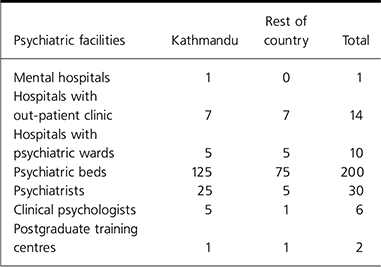
Unfortunately, almost all mental health professionals and services are based at urban centres, mostly in the capital, Kathmandu (Table 3). Although private medical schools with an attached psychiatric unit are being opened all over the country, the entire process is patchy and unplanned.
Table 3. Current mental health facilities in Nepal inside and outside Kathmandu
| Psychiatric facilities | Kathmandu | Rest of country | Total |
|---|---|---|---|
| Mental hospitals | 1 | 0 | 1 |
| Hospitals with out-patient clinic | 7 | 7 | 14 |
| Hospitals with psychiatric wards | 5 | 5 | 10 |
| Psychiatric beds | 125 | 75 | 200 |
| Psychiatrists | 25 | 5 | 30 |
| Clinical psychologists | 5 | 1 | 6 |
| Postgraduate training centres | 1 | 1 | 2 |
The way forward
The number of psychiatrists and other mental health professionals has been steadily growing in Nepal since the author came to the UK in 1986 for higher psychiatric training. A few extra psychiatric wards and postgraduate psychiatric training programmes have been added during the past 20 years but a lot remains to be done. To improve mental healthcare in Nepal, efforts should be focused on raising awareness, making existing services available to the general public and monitoring mental health delivery systems (Reference REGMI, POKHREL and OJHARegmi et al, 2004). Nepalese psychiatrists have to start talking to each other and to their neighbours and colleagues across the world, not just to satisfy their personal ambitions but also to address the grossly neglected mental health programme of their country. Nepalese psychiatrists living in the UK are conscious of their obligation towards Nepal, and are determined to turn the tide of brain drain into a gentle flow of brain circulation.
To maintain their morale and motivation, they will have to set up research projects. Alternative routes to healing need to be identified to suit local needs. Recent advances in psychiatry, as reflected by research and practice in the Western world, cannot be applied directly to meet the mental health needs of the non-Western world. George Hsu (Reference GEORGE HSU2004) suggests that some of us in the low-income countries should make an effort to channel our research into four main areas: rehabilitation of those with chronic mental illness; treatment of major depression by primary care physicians; developing a more culturally acceptable form of psychotherapy; and reducing stigma associated with mental illness. Non-governmental organisations such as the South Asia Forum on Psychiatry and Mental Health and the Nepalese Doctors’ association (UK) are anxious to help Nepalese psychiatrists.
Declaration of interest
None.
Acknowledgements
I thank the Nepalese psychiatrists Dr Pramod Shyngwa, Dr Shailendra Adhikary, Dr C. P. Sedain and Dr Ranjan Thapa as well as the physicians Dr Gaurang Mishra and Dr Vijay Kumar Singh, and all the Red Cross staff for their help at the Janakpur Mental Health Camp.








eLetters
No eLetters have been published for this article.