The Mental Health Policy Implementation Guide (Department of Health, 2001) outlines how early intervention in psychosis services should function. At the time the guidelines were issued, there was little evidence for the effectiveness of these services (Reference Pelosi and BirchwoodPelosi & Birchwood, 2003) but evidence is now accumulating. The early onset randomised controlled trial in Lambeth showed that assertive early intervention reduced the relapse and hospital readmission rates compared with usual community mental healthcare (Reference Craig, Garety and PowerCraig et al, 2004), improved service users’ social and vocational functioning, quality of life and medication adherence (Reference Garety, Craig and DunnGarety et al, 2006). Petersen et al (Reference Petersen, Jeppensen and Thorup2005) found in a randomised trial that assertive integrated community treatment in Denmark compared with usual community mental healthcare led to reduced bed days and improved clinical outcomes and treatment adherence. In a Canadian study (Reference Goldberg, Norman and HochGoldberg et al, 2006), in-patients with non-affective first-episode psychosis were assessed before and after the introduction of an early intervention in psychosis service. When early intervention was used, there was a smaller number of hospital admissions and reduced violent behaviour.
We used the same design in our study as Cullberg et al (Reference Cullberg, Mattsson and Levander2006), comparing a prospective group that received care from an early intervention psychosis service with a historical group that received treatment as usual. The early intervention in psychosis service was based on a hub and spoke model adapted from the Department of Health's guidelines (Reference Paxton, Chaplin and SelmanPaxton et al, 2003) for a mixed urban/rural area. Some staff were based within community mental health teams, but the service was functionally compliant with the Department of Health's guidelines. We aimed to replicate the emerging findings indicating the advantages of early intervention in psychosis compared with usual care, and to investigate the effects on hospital readmission (generally the most expensive element of mental healthcare) and service users’ engagement with services.
Method
Participants
In September 2002, an early intervention in psychosis team was established in Northumberland. The service aimed to take on all individuals with first-episode psychosis in the county. Participants were service users under 36 years of age who presented between October 1998 and September 2005. The first group (n=114) were individuals who presented between October 1998 and September 2002 (i.e. before the service had been established), but who would have met the acceptance criteria for the service. The other group (n=75) were all individuals who received treatment from the service between September 2002 and October 2005 (Table 1).
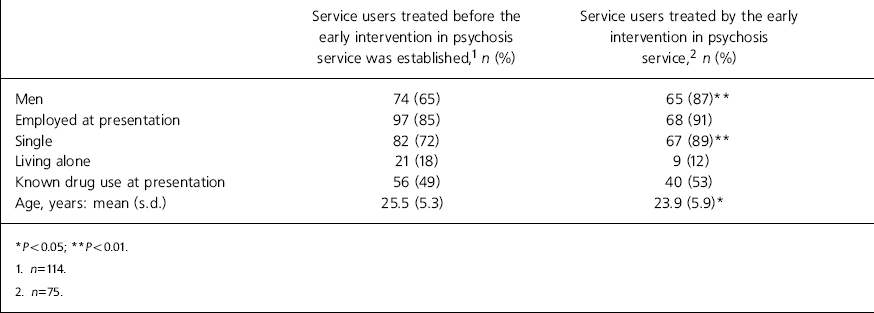
Table 1. Demographics
| Service users treated before the early intervention in psychosis service was established, 1 n (%) | Service users treated by the early intervention in psychosis service, 2 n (%) | |
|---|---|---|
| Men | 74 (65) | 65 (87) ** |
| Employed at presentation | 97 (85) | 68 (91) |
| Single | 82 (72) | 67 (89) ** |
| Living alone | 21 (18) | 9 (12) |
| Known drug use at presentation | 56 (49) | 40 (53) |
| Age, years: mean (s.d.) | 25.5 (5.3) | 23.9 (5.9) * |
* P<0.05
** P<0.01
1. n=114
2. n=75
We compared the two groups using a χ2-test and found significant differences linked with a poor prognosis, male gender (Reference Murray and Van OsMurray & Van Os, 1998), marital status (Farnia et al, 1963), and younger age at onset (Reference Jablensky, Sartorius and ErnbergJablensky et al, 1992). This suggests a worse prognosis would be expected in the group who received early intervention treatment.
Procedure
Data were obtained from the Population-Adjusted Clinical Epidemiology database (PACE; Reference Proctor, Mitford and PaxtonProctor et al, 2004). The database recorded prospective information on the presentation, management and outcomes of all individuals with first-episode psychosis in Northumberland.
Participants were identified by consultant psychiatrists and referred to the PACE team. The team gathered information on demographics, ICD-10 diagnosis, hospital admissions, medication, contact status, risk assessment and use of services, but we used only patient information on demographics, hospital admissions and employment status for the study. Data were gathered from in-patient and out-patient secondary care medical notes at presentation and annually on a continuing basis. The PACE staff had no contact with patients and were not involved in their care or management. They also screened the local National Health Service (NHS) computerised patient information system and sent monthly reminders to consultant psychiatrists to ensure comprehensive data.
Analysis
Data on 253 individuals were collected between October 1998 and October 2005; 64 individuals were excluded from the main analysis as they did not meet the acceptance criteria for the early intervention. Of the excluded service users, 20 presented before the service had been established; 44 presented after that but were not accepted for treatment by the service. They were excluded for the following reasons: a diagnosis of borderline personality disorder at any stage of follow-up; a predominant diagnosis of organic psychosis across the 3-year follow-up; drug/alcohol-induced psychosis that did not persist 5 days after the intoxication; having moved out of area or transferred care within the first year after referral; a diagnosis of bipolar disorder without psychotic symptoms.
Excluded service users were compared with those included in the study to ensure that their exclusion did not bias the analysis. An analysis of variance (ANOVA) showed no significant differences between the two groups.
We analysed differences between the groups in hospital bed usage, engagement with services, and as a possible confounding factor - differences in atypical antipsychotic medication.
Data were analysed using SPSS version 14.0 for Windows.
Results
Hospital admissions
We used a one-way between-groups ANOVA to see whether the early intervention had any effect on the service users’ number of admissions in the first 3 years of receiving mental health treatment, the number of readmissions and the total number of days in hospital (Table 2). There were significant differences between the two groups in each case respectively: P<0.001 [F (1, 187)=10.8], P<0.001 [F (1, 187)=9.2], P<0.01 [F (1, 187)=5.8].
Table 2. Hospital admission data

| Admissions in first 3 years Mean (s.d.) | Readmissions in first 3 years Mean (s.d.) | Bed days in first 3 years Mean (s.d.) | |
|---|---|---|---|
| Service users treated before the early intervention in psychosis service was established (n=114) | 1.9 (2.58) | 1.3 (2.35) | 96.7 (167.5) |
| Service users treated by the early intervention in psychosis service (n=75) | 0.9 (1.25) | 0.4 (0.99) | 44.9 (100.3) |
Engagement with services
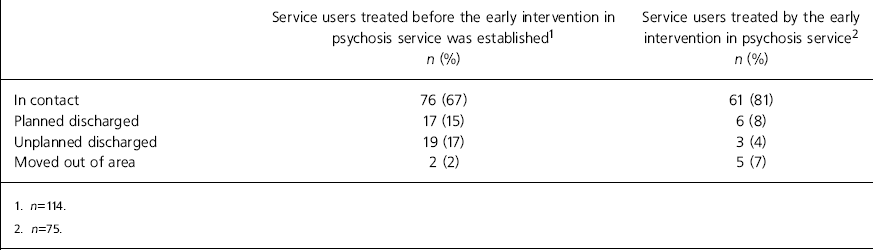
Engagement with services 1 year after first presentation was compared in the two groups using a χ2-test (Table 3). The group who used the early intervention service were significantly more likely to still be engaged with services at 1 year follow-up (P<0.05).
Table 3. Engagement with services at one year
| Service users treated before the early intervention in psychosis service was established 1 n (%) | Service users treated by the early intervention in psychosis service 2 n (%) | |
|---|---|---|
| In contact | 76 (67) | 61 (81) |
| Planned discharged | 17 (15) | 6 (8) |
| Unplanned discharged | 19 (17) | 3 (4) |
| Moved out of area | 2 (2) | 5 (7) |
1. n=114
2. n=75
Discussion
This is the first naturalistic study to report significantly improved outcomes for individuals who used a standard NHS early intervention in psychosis service functionally compliant with the Department of Health's guidelines.
Comparison with previous research
Despite the recent inconclusive Cochrane review (Reference Marshall and RathboneMarshall & Rathbone, 2006) and the scarce number of available randomised controlled trials, several recent findings on the effectiveness of early intervention in psychosis services have been encouraging. The present study confirms the findings of Craig et al (Reference Craig, Garety and Power2004) and Goldberg et al (Reference Goldberg, Norman and Hoch2006) in demonstrating reduced bed days, and Petersen et al (Reference Petersen, Jeppensen and Thorup2005) in demonstrating improved engagement. McCrone & Knapp (Reference McCrone and Knapp2007) have developed a model to estimate the economic impact of early intervention services and they have suggested that such services can save costs. In the present study the savings on reduced bed days were significantly greater than the cost of operating the service - 4755 bed days were saved in the early intervention. When multiplied by the trust tariff for an adult acute bed day (£258), this led to an estimated saving of £1226 790. The total cost of the service was estimated at £804 122, giving a net saving of £422 668 over the period of the study. This does not include the treatment-as-usual costs of community mental health teams and other elements.
The Northumberland early intervention in psychosis service covers an area of nearly 2000 square miles and has an expected incidence of 30 new cases per year. The model of service delivery had to be adapted - instead of the recommended specialist team, a hub and spoke model was used where care coordinators were embedded within community mental health teams. As the service developed, more staff, including care coordinators, were embedded in the hub. This is the first study to show the effectiveness of a hub and spoke model of early intervention in psychosis and that the service can be effectively delivered in rural areas.
Limitations
There are some limitations owing to the service model and service design. The PACE database selected 44 individuals that did not meet the inclusion criteria for the early intervention; the early intervention group had to be retrospectively assessed to exclude those who would not have been accepted by the service. This suggests that the early intervention in psychosis team, which functioned according to the Department of Health's model, had narrower acceptance criteria and was targeted at the more unwell. This is also supported by the significant differences in gender, age and marital status between the two groups, which suggest that the early intervention group should have had a poorer prognosis.
The quasi-experimental design used here is vulnerable to potential confounding factors. One is a possible difference in prescribing of atypical antipsychotics between the two groups - in our study, 85% of the early intervention group and 63% of the treatment-as-usual group were prescribed atypical antipsychotics as first-line antipsychotic medication. We are not aware of any research suggesting that the use of atypical antipsychotics reduces bed days and so it is unlikely that their greater use in the first group affected the results.
Another possible confounding factor is the development of crisis resolution and home treatment services. In Northumberland it was staged by both locality and function. In the west of Northumberland, a limited hours crisis service was operational throughout the period of our study (it only became a 24-h service in 2006). In the more densely populated south-east region, the service was developed in 1999 but only started operating for 24 h, 7 days a week in 2005 (that is, during the last 16 months of the data collection for our study). Glover et al (Reference Glover, Arts and Babu2006) suggested that only the crisis resolution services operating in this latter system have an effect on admissions for young people. This staged development may explain the low usage of crisis resolution services, with only 25% of the pre-early intervention group and 42% of the treatment-as-usual group using the crisis resolution service. Moreover, some researchers suggest that the crisis resolution service has limited effectiveness for men (Reference Dean and GaddDean & Gadd, 1990; Reference Schnyder, Klaghofer and LuetholdSchnyder et al, 1999) and people with a functional psychosis (Reference Schnyder, Klaghofer and LuetholdSchnyder et al, 1999; Reference Guo, Biegel and JohnsenGuo et al, 2001; Reference Abas, Vanderpyl and Le ProuAbas et al, 2003). Thus, the limited development of crisis resolution service in Northumberland during the period of this study and the evidence of its relative ineffectiveness with our main participant group (young men experiencing psychosis) make it unlikely that it was responsible for the highly encouraging results reported.
Implications
The study has several important implications, although because of the limitations of the before/after design the findings should be interpreted with caution. Still, the results suggest that early intervention in psychosis services based on the Department of Health's guidelines can lead to significant cost savings. They are, alongside crisis resolution services, an ‘invest to save’ opportunity. More significantly, reducing hospital admissions which can often be traumatic (Reference Morrison, Frame and LarkinMorrison et al, 2003) is an important outcome for service users. The study supports the usefulness of the Mental Health Policy Implementation Guide, and shows that it can be modified successfully in a mixed urban/rural area using a hub and spoke model with the hub having a key role in ensuring functional fidelity to the guidelines. We believe that this mechanism is crucial for effectiveness.
Randomised controlled trials remain the gold standard for research on the effectiveness of different interventions. However, in the absence of credible alternative intervention packages, the ethical difficulties in with-holding interventions with proven efficacy from the control group, then quasi-experimental, naturalistic designs can be of value.








eLetters
No eLetters have been published for this article.