There is extensive international evidence of the substantial burden of severe mental illness in prisoners. For example, in a study of 16 prisons and institutions for young offenders in the UK, Brooke et al found that 5% of the remand population had a psychotic or affective disorder. Reference Brooke, Taylor, Gunn and Maden1 In a systematic review of 62 surveys based on interviews of unselected prison populations in Europe, Australia, New Zealand, Canada and the USA, Fazel & Danesh found consistent evidence that prisoners were several times more likely to have psychosis or major depression than the general population. They also found that comorbidity between mental illness, substance misuse and personality disorder was the norm, rather than the exception. Reference Fazel and Danesh2
Harty et al used systemic needs assessment instruments to demonstrate that mentally disordered prisoners at London's HM Prison Belmarsh differed from general adult patients living in the community: they had significantly more needs, and more unmet needs, in relation to mental health. Their unmet needs were in the domains of psychotic symptoms, psychological distress, company and daytime activities. Reference Harty, Tight, Reese, Parrott and Thornicroft3
Although there have been considerable improvements in mental health services for prisoners in the UK over the past decade, prison healthcare centres do not provide equivalent healthcare to that available in in-patient units, Reference Wilson4 nor are they recognised as places where compulsory treatment can be given under the provisions of the Mental Health Act. Mental health teams in prison expect to be able to support prisoners with stable mental illness during a period in custody, but require support from local mental health providers for the provision of in-patient care when necessary.
The care pathway for prisoners requiring in-patient treatment is fraught with difficulties and most prison healthcare centres in London are used to accommodate prisoners at various stages of the transfer process. They have therefore become, for large numbers of prisoner-patients, waiting rooms for hospital admission.
In recognition of this problem, the Department of Health produced an invitation to pilot a national waiting time standard for the transfer of acutely mentally ill prisoners, 5 and published practice guidelines in which an ambitious 7-day target for transfer to hospital was set (later amended to 14 days). 6 This invitation has since been taken up by a number of National Health Service (NHS) providers within the London area, and an outcome is awaited.
Method
Data collection
The London prison estate contains seven prisons (including one prison for women, HM Prison Holloway, and one young offender institution, HM Prison and Young Offender Institution Feltham) and has an overall capacity of just under 7000. This study involved two central London prisons with differing functions: HM Prison Brixton and HM Prison Belmarsh.
HM Prison Brixton is one of the oldest correctional facilities in the UK, dating from 1819. It presently functions as a category B, or medium secure, local remand prison. Serving a variety of local courts, it has an operational capacity of almost 800. HM Prison Belmarsh became operational in 1991 and has an operational capacity of just over 900. It also serves local courts but has an additional function as a high secure prison involving the detention of category A prisoners.
Prospective audit data were collected from clinical records at both prisons for all prisoners transferred to psychiatric facilities under Part III of the Mental Health Act 1983 during the period 1 June 2003 to 31 October 2004 (a total of 17 months). Prison transfer records were cross-checked to ensure accuracy and entered into a referral database (set up as an Excel spreadsheet). The collected data comprised referral, assessment, acceptance and transfer times, along with the level of security of the accepting unit and the section of the Mental Health Act used.
For the purpose of this study, the transfer period began when a referral was made by the prison's mental health service to a receiving unit and continued until the date when actual transfer took place. Although this system was not the same as the prison service's ‘traffic lights’ measuring system, which measured transfer time from date of acceptance rather than date of referral, it provided a more accurate account of waiting times.
Results
There were a total of 149 transfers from both prisons to NHS mental health facilities during the 17 months under examination (just under nine transfers per month): 92 from Brixton and 57 from Belmarsh (four individuals were excluded from the study because their medical records could not be located). During the same period, six of those transferred to hospital were remitted to prison under section 50 of the Mental Health Act. Two of those remitted required immediate re-referral and re-admission.
Of those transferred from Brixton, 60% were charged with, or had committed, some form of violent offence (including grievous bodily harm, actual bodily harm, assault or common assault). Of those transferred from Belmarsh, 73% were detained in respect of a violent offence (of which over 50% included murder, attempted murder or manslaughter). The offence spread was therefore more serious at HM Prison Belmarsh, as might be expected from its category A function.
Although the majority of those transferred from both prisons were already known to mental health services (74% at HM Prison Brixton and 75% at HM Prison Belmarsh), a substantial number from both groups (25%) had no history of contact (being provided with services for the first time within the prison system). The past psychiatric history of four prisoners was not known.
The majority of prisoners were transferred to one of four different levels of security within NHS hospitals and a small number were transferred to facilities with a specialist function (e.g. learning disability services). The levels of security involved were:
-
• general adult wards
-
• psychiatric intensive care units
-
• medium secure units
-
• high-security hospitals.
The transfer details are quantified in Table 1.
Table 1. Facilities where the prisoners were transferred, by the level of security

| Facility | HM Prison Brixton, % | HM Prison Belmarsh, % |
|---|---|---|
| General adult ward | 8 | 3 |
| Psychiatric intensive care unit | 54 | 23 |
| Medium secure unit | 34 | 54 |
| High secure unit | 1 | 19 |
| Specialist facility | 3 | 2 |
Legal provisions
Part III of the Mental Health Act 1983 allows for a number of sections to be used to facilitate prisoner transfer to mental health facilities. Of the sections available for use, the following were the most relevant:
-
• section 48 (allowing the clinical transfer of remand prisoners without court involvement)
-
• section 47 (allowing the clinical transfer of sentenced prisoners without court involvement)
-
• section 49 (restricting the discharge of prisoners transferred to hospital)
-
• section 35 (a remand order issued by the court)
-
• section 37 (a hospital order issued by the court)
-
• section 38 (an interim hospital order, allowing a period of evaluation in hospital before definitive disposal).
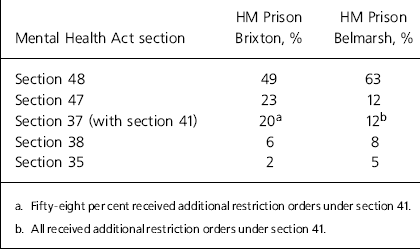
Of the main Mental Health Act sections used, sections 47 and 48 were administered by the mental health department at the Home Office (now the Ministry of Justice), all such prisoners receiving a parallel order restricting their discharge under section 49. The remainder came under the determination of the courts (with the option of adding a restriction order under section 41 of the Mental Health Act to those whose cases were finally disposed of via a hospital order under section 37). Results are presented in Table 2.
Table 2. Mental Health Act sections used to facilitate prisoners’ transfer to mental health services
| Mental Health Act section | HM Prison Brixton, % | HM Prison Belmarsh, % |
|---|---|---|
| Section 48 | 49 | 63 |
| Section 47 | 23 | 12 |
| Section 37 (with section 41) | 20a | 12b |
| Section 38 | 6 | 8 |
| Section 35 | 2 | 5 |
Waiting time
The 92 mentally disordered prisoners at HM Prison Brixton waited, in aggregate, some 22 years (8428 days) in prison for a hospital bed over the 17 months of the study. The average wait per prisoner was 102 days. Of those transferred, only 20% were referred, assessed and transferred within 1 month, 38% were transferred within 3 months, 42% waited longer than 3 months and a further 10% waited longer than 6 months.
Meanwhile, the 57 mentally disordered prisoners at HM Prison Belmarsh waited, in aggregate, some 14.5 years (5285 days) for a hospital bed, with an average wait per prisoner of 93 days. Of those, 21% were referred, assessed and transferred within 1 month and 37% within 3 months. In keeping with the figures from Brixton, 42% waited longer than 3 months for a hospital bed and the remaining 10% waited in excess of 6 months.
Based on unit costs, 7 we estimate the total saving to the NHS for both prisons over the period under examination at £6 757 644. Costs have been calculated for prisoners transferred under all Mental Health Act orders, not merely the ‘urgent’ sections, as in our experience court orders often simply expedite the transfer process for individuals who have already been referred on an urgent basis. A breakdown of costs and savings is given in Table 3.
Table 3. Savings to the NHS over the study period (June 2003–October 2004)

| Savings, £ | ||||
|---|---|---|---|---|
| Transfer facility | Unit cost per patient per day, £ | HM Prison Belmarsh | HM Prison Brixton | Total |
| General adult ward | 258 | 40 906 | 173 954 | 214 860 |
| Psychiatric intensive care unit | 542 | 658 828 | 2 466 707 | 3 125 535 |
| Medium secure unit/specialist facility | 453 | 1 340 699 | 1 412 618 | 2 753 317 |
| Maximum secure hospital | 610 | 612 531 | 51 411 | 663 942 |
Discussion
NHS and prison service align
The way in which mental healthcare is provided for prisoners in England and Wales has changed substantially over the past decade, since serious problems with earlier provision (including poor quality care and professional isolation) were identified by HM Chief Inspector of Prisons in 1996. 8 Before then, visiting psychiatrists received referrals from resident prison medical officers and service provision was patchily available. In an attempt to solve the problems, mental health in-reach services, intended to be similar in design to community mental health teams, were introduced to the prison estate in 2001. More recently, local primary care trusts have taken responsibility for commissioning services (full primary care trust commissioning came online in 2006).
With this new formal relationship between the prison service and the NHS has come a new form of scrutiny. By virtue of its new location inside the walls of the prison, the NHS becomes increasingly responsible for the healthcare needs of prisoners and for monitoring whether those needs are, or are not, being met.
London's recent transfer history
Earlier research at HM Prison Brixton has described frustration, difficulties and delays with the referral and assessment process. In the early 1990s, an average 5- to 6-week delay between a prisoner being offered a bed and being admitted to hospital was standard. Reference Robertson, Dell, James and Grounds9 Although a later study into the effectiveness of a psychiatric diversion scheme from HM Prison Belmarsh suggested some cause for optimism, Reference Banerjee, O'Neill-Byrne, Exworthy and Parrott10 a subsequent audit identified lengthy delays before a hospital bed was found. Reference Isherwood and Parrott11 Multiple problems were identified in the second audit, including differences in opinion, legal disputes, diagnostic disagreements, long delays before initial assessments and NHS catchment area disputes.
More recently, in recognition of the problem, the Department of Health has produced new administrative procedures to reduce delays. 6 These procedures, designed to ensure that the commissioning primary care trusts are aware of their financial responsibilities at an early stage, have since been cascaded through the prison estate. One London prison (HM Prison Pentonville) has described a subsequent reduction in transfer waiting times. Reference McKenzie and Sales12 However, the significance of these results for the wider prison estate remains uncertain. Reductions in waiting times have apparently been minimal (from 77 to 53 days), remaining far short of the Department of Health's target, as the 7-day target has since been replaced by a 14-day target. This seems to indicate that that problem has, if anything, become worse since the early 1990s.
Implications
We remain concerned about the transfer delays described in this paper. We are particularly concerned about those who wait untreated in prison, without the protection of the Mental Health Act, for whom the only recourse to treatment used to be Common Law but may now involve the Mental Capacity Act 2005. Reference Wilson and Forrester13 Although we do not yet know the numbers involved, many are unable to make decisions for themselves because they lack capacity. The Mental Capacity Act 2005 requires individuals and services to act in the best interests of such individuals; delaying hospital admission does not meet this aim. In the case of Jean-Luc Riviere v. France, the European Court of Human Rights ruled that Riviere's continued detention in prison when he required treatment for mental illness contravened his Article 3 right to freedom from inhuman and degrading treatment. 14 We therefore think that the delays described in this paper could be subject to legal challenge.
Declaration of interest
None.








eLetters
No eLetters have been published for this article.