‘Children with a parent with mental illness often fall through the professional net and are seen as nobody's responsibility. Nothing is explained to them, and they often receive no help at all to deal with the effects of the parent's illness’ (Royal College of Psychiatrists, 2004).
It is usual psychiatric practice to assess the risk that might be posed to a child by a mentally ill parent and for trusts to provide guidance on child visiting. However, little attention has been paid to relations between detained forensic in-patients and their children, either from the parent's or the child's point of view, beyond simple statements of principle (Royal College of Psychiatrists, 2002). In particular, the potential impact of parental mental illness on children tends to receive little consideration from psychiatric services. They generally restrict their interest to whether or not it is safe for the children to visit or to have other contact with the detained parents. As the Fallon inquiry demonstrated, the focus of concern has been about protecting children from victimisation from their parents and other patients (Reference Fallon, Bluglass and EdwardsFallon et al, 1999). Meanwhile, there has been little interest in the negative impact of separation on both parents and children.
This is a problematic area to tackle in all psychiatric in-patients. There are added complications within the forensic setting, as the issue of offending may need to be addressed in addition to mental illness. There may be difficulties in terms of revealing or understanding the offending, which complicates the already sensitive issue of a serious mental disorder and the impact that this may already have had on the development or maintenance of relationships between parent and child. In some cases, the offending will have involved another family member as a victim, which is likely to have a particularly destructive effect on relationships within the family. Yet, adult mental health services do not have responsibility for their patients’ children, whereas the role of social services (where these are involved) is strictly focused on the child. Child and adolescent mental health services, which arguably would have the expertise to deal with the parent–child relationship, are over-stretched and reluctant to become involved with children who do not have mental illness or severe psychological problems.
We wished to explore these issues in a sample of in-patients in two medium secure units who had children aged 18 or under. The aim was to find out the proportion of patients who had children in this age group, whether or not they were in contact with them and the extent to which the services treating the parent had offered any support to the children.
Method
This descriptive retrospective study was conducted at two medium secure units in London. A census of in-patients in each unit was conducted and those with children aged 18 or under were identified. Further details were then recorded using a standard form: basic information about the parent, children, contact between the child and the parent and details of any support provided by the multidisciplinary team (see the online data supplement to this paper). Information was obtained from in-patient notes and missing data were obtained from social workers and responsible medical officers.
Results
There were 324 in-patients in the two medium secure units surveyed: 69 had children (21%; 12 (38%) of the 32 female and 57 (20%) of the 292 male patients). The patients were ethnically diverse. Almost all had a diagnosis of psychotic illness, were commonly detained under Part III of the Mental Health Act 1983 and had often committed offences of interpersonal violence (physical violence, including homicide) (Table 1).
Table 1. In-patient characteristics

| Female patients | Male patients | |
|---|---|---|
| Total, n | 12 | 57 |
| Age, years: range (mean) Ethnicity, % | 27-45 (37) | 20-48 (37) |
| White | 42 | 21 |
| African—Caribbean | 25 | 44 |
| Asian | 8 | 19 |
| Mixed | 25 | 16 |
| Diagnosis of psychotic illness, % | 100 | 90 |
| Detained under Part III of the Mental Health Act 1983, % | 75 | 88 |
| Convictions for interpersonal violence, % | 66 | 60 |
Children
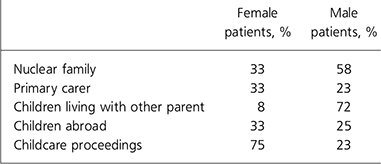
On average, the patients had two children each. Many of the male patients, but fewer female patients, had lived in a nuclear family at some time prior to their admission to hospital. A minority had been primary carers of their children – more likely, if they had been part of a nuclear family (χ2=9.6, d.f.=1, P=0.02) and if they were not born in the UK (χ2=3.9, d.f.=1, P=0.048). The great majority of the children of the male patients lived with their other parent, but this was not the case for female patients; several children lived abroad. Childcare proceedings were much more common for the female patients (χ2=10.2, d.f.=1, P=0.001) than male patients and more likely when the patient was not the primary carer (χ2=5.8, d.f.=1, P=0.016) (Table 2).
Table 2. Children and families
| Female patients, % | Male patients, % | |
|---|---|---|
| Nuclear family | 33 | 58 |
| Primary carer | 33 | 23 |
| Children living with other parent | 8 | 72 |
| Children abroad | 33 | 25 |
| Childcare proceedings | 75 | 23 |
Contact and support
Female patients had more contact with their children, including supervised visits. Support was offered in a minority of cases. It was more likely to be offered when the children had supervised visits (χ2=11.7, d.f.=1, P=0.01) and where the parents were still in a relationship together (χ2=4.2, P=0.04). When offered, support was usually accepted. In most cases, it was provided by the hospital social worker (Table 3).
Table 3. Child contact and support

| Female patients, % | Male patients, % | |
|---|---|---|
| Any contact with children | 58 | 32 |
| Supervised visits | 42 | 21 |
| Support offered | 33 | 18 |
| Support accepted | 75 | 70 |
Common reasons for absence of contact (and support) were a lack of knowledge of the children's whereabouts and adoption. Other reasons included: children living abroad; the nature of the offence, particularly sexual offences against a child under the age of 16 or where a family member was the victim; and the children being frightened of their parent. Several of the children were too young to be offered support.
Discussion
It is striking that less than a third of patients with children had any contact with them. There are many reasons for this. Many of the patients came from unstable backgrounds, with a history of dysfunctional relationships and a resultant loss of contact with both partners and children. In some, there was a history of abuse and others may not have been capable of parenting, such that the only option was for their children to be put up for adoption. However, for those children of forensic in-patients that can be contacted, it is important that they have the opportunity to ask questions. They may have built up a frightening picture of their mentally ill parent which may or may not be based in reality.
In those patients where it was possible to contact the children, the question arose as to whose responsibility it was to address the children's needs. Child and adolescent mental health services are stretched and reluctant to become involved with children who are unlikely to meet their referral criteria, whereas adult forensic services have concerns that they lack expertise in dealing with children. Additionally, adult forensic services may be perceived as leaning towards the interests of their patients. Certainly, comprehensive knowledge of the patient is essential in being able adequately to discuss and explain, but not necessarily justify, the difficulties the parent may have. For this reason, it was common for a member of the multidisciplinary team, usually the social worker involved in the care of the patient, to provide this input.
The offer of support from forensic mental health services may not be deemed acceptable, particularly where a member of the family was the victim and may feel that the patient has escaped punishment. Similarly, if the primary carer, for whatever reason, does not consent to contact with the team, the children may not be able to clarify uncertainties about their mentally ill parent, and may not feel able to discuss their parent with their carer for fear of causing them distress. In these situations, a member of the multidisciplinary team can attempt to speak to the carer and offer to meet them. The patient too should provide consent prior to discussion with the family.
The catchment areas of the two units studied here cover some of the most ethnically diverse inner-city boroughs in the country (Office for National Statistics, 2003). Several patients and their partners did not speak English, although their children were generally fluent in English. Family welfare organisations may be able to assist in such cases as they have an understanding of various languages and cultures. However, they should only be used in consultation with the multidisciplinary team, as such organisations are unlikely to have sufficient familiarity with the case in order adequately to address the needs of the child or be sufficiently knowledgeable about issues of confidentiality. Patients and families may resist support from cultural organisations for fear of the local community becoming aware of their situation. Stigma and discrimination surrounding mental illness are prevalent and this may be more so among ethnic minority groups (Office of the Deputy Prime Minister, 2004).
The children of forensic in-patients are a difficult population group to access. Although we are encouraged to consider ‘patients as parents’, guidance given to forensic psychiatrists places an emphasis on risk assessment and working with the parent, but not the child (Royal College of Psychiatrists, 2002). Even so, although child protection procedures and the best interests of the child are central to the regulation of visits to patients in secure psychiatric units, it would seem that the responsibility of forensic mental health services towards the children may extend beyond this, and that offering support where possible is good practice. A collaborative approach involving other agencies may be the best way to undertake this.
Declaration of interest
None.
Acknowledgements
We thank the social workers for their assistance in data collection and Dr David James for his helpful comments.








eLetters
No eLetters have been published for this article.