Electroconvulsive therapy (ECT) is effective in the treatment of major depression but can also cause problems, especially memory impairment (National Institute for Health and Clinical Excellence, 2003). In the UK, the National Institute for Health and Clinical Excellence (NICE) has recommended restricting its use to severe depression, catatonia or severe mania when other treatments have failed (National Institute for Health and Clinical Excellence, 2003). Globally, ECT has been in decline but the variability between countries is marked and related to socio-political factors such as unfavourable public perception and professional attitude (Reference Eranti and McLoughlinEranti & McLoughlin, 2003).
In the UK, ECT data were routinely collected by the National Health Service (NHS) until 1991, when specific ECT reporting was replaced by Hospital Episode Statistics, considered to significantly underreport ECT activity (Department of Health, 2003). In response, the Department of Health conducted two retrospective surveys (Department of Health, 1999, 2003). Questionnaires were sent to all NHS trusts and private hospitals with mental health facilities in England for collation of information. Many trusts were able to return data after minimal adjustments to the manual record kept in ECT suites. Both surveys demonstrated a steady decline of ECT, a trend which began in 1985 (Department of Health, 1999). The latest survey from 2002 (Department of Health, 2003) showed an additional 5% of patients receiving ECT had been treated at private facilities. Limitations in the quality of the data were acknowledged: retrospective design, primary focus on demographic factors and a lack of qualitative enquiry in either of the studies. However, the studies were considered by the Department of Health to be ‘broadly representative’ of ECT treatment patterns. The reports also provided data from previous Department of Health reports in 1985 and 1991, which are cited below for purposes of ECT data comparison.
The ECT Accreditation Service (ECTAS) was launched in May 2003 to ensure quality and continual improvement of the administration of ECT (Reference Cresswell, Fortune and LelliottCresswell et al, 2005). The service was set up by the Royal College of Psychiatrists with the support of the Royal College of Anaesthetists and the Royal College of Nursing. Since the 2002 survey, there have been observations that ECT has declined, following the closure of small ECT clinics and centralisation of provision. This study aims to estimate current ECT activity in England using improved method and a similar time period and compare it with previous reports.
Method
A postal survey was sent to all NHS ECT clinics in England via the medical directors of NHS mental health trusts. The lead psychiatrist or nurse from each clinic was asked to complete a questionnaire that enquired about details of each ECT session to be carried out between January 2006 and the end of March 2006. Respondents were asked to provide the following: the number of ECT applications on each session, the number of ECT sessions, the total number of patients commencing ECT and the total number of patients finishing ECT. They were asked to add data to the questionnaire prospectively at the end of each ECT session. Electroconvulsive therapy clinic staff were not asked for patient details or identifiers because of patient confidentiality. Therefore, the length of the ECT course could not be measured directly and had to be estimated using the following equation.
This calculation provides the mid-point (mean) of two estimates of the length of the course of ECT.
In addition to data on the quantity of ECT administered, qualitative questions enquired about changes to the provision of ECT in the trust over past 5 years and what changes the staff anticipated in the next 5 years. Non-responders were contacted by post and encouraged to return the completed questionnaire. Chi-squared analysis was applied to the proportions of patients in successive studies receiving ECT with either informal status or detained under the Mental Health Act. Lack of access to the full data-sets for the previous studies precluded statistical comparisons using parametric tests, for example comparing the mean number of applications per course of treatment.
Results
Responses were obtained from 56 of the 76 (74%) trusts providing ECT at 109 clinics. Not all mental health trusts provided ECT. Three trusts commissioned services from neighbouring trusts and transported patients as necessary. The number of clinics per trust varied from 0 to 5 with a mean of 2. The level of clinical activity showed considerable range with the busiest clinics having up to 12 patients treated per session and several clinic sessions having no patients.
A total of 986 patients were recorded as having a first treatment and 899 a final treatment over the 3-month study period. They received a total of 5019 applications of ECT. To estimate the total ECT activity in England over that period, it is necessary to assume that clinics not responding to the questionnaires had similar rates of ECT activity to those that responded. With this estimation we calculated that approximately 6782 applications of ECT would have been given to 1276 patients in England over the study period; 30% of patients received it when detained compulsorily under the Mental Health Act.
Even if double the rates of ECT administration had been given in the non-responding clinics, our data would still show a sharp decline in its use (the number of ECT applications would be 8725 and the number of patients treated 1608).
The mean length of the ECT course during the 3-month study period was estimated: 5019 treatments were given, 986 of these were first treatments and 899 were last treatments, (5019/986 + 5019/899) ÷ 2 = 5.3.
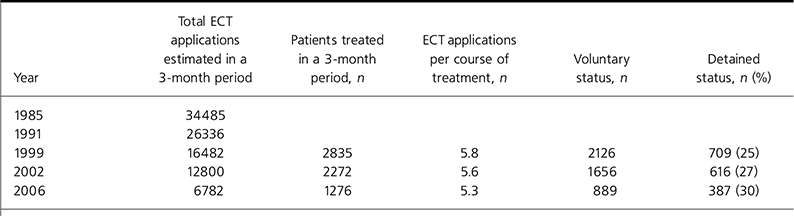
Data from our 2006 study were compared with those from the previous Department of Health studies of 1999 and 2002. They show an overall decline in the number of ECT applications and the number of patients treated over the 7-year period (Table 1). The number of ECT applications per course of treatment has shown only a slight decline with means of 5.8 in 1999 and 5.6 in 2002, although our estimation of 5.3 in this study allows no further conclusions to be drawn. The numbers of patients treated when detained under the Mental Health Act were compared between the three studies. Between 1999 and 2002 the increase was not significant (χ2=2.98, d.f.=1, P=0.084), but the proportion of detained individuals significantly increased between 2002 and 2006 (χ2=4.17, d.f.=1, P=0.041), and overall a highly significant increase occurred between 1999 and 2006 (χ2=12.74, d.f.=1, P=0.0004).
Table 1. Estimated numbers of patients treated over 3-month study periods
| Year | Total ECT applications estimated in a 3-month period | Patients treated in a 3-month period, n | ECT applications per course of treatment, n | Voluntary status, n | Detained status, n (%) |
|---|---|---|---|---|---|
| 1985 | 34485 | ||||
| 1991 | 26336 | ||||
| 1999 | 16482 | 2835 | 5.8 | 2126 | 709 (25) |
| 2002 | 12800 | 2272 | 5.6 | 1656 | 616 (27) |
| 2006 | 6782 | 1276 | 5.3 | 889 | 387 (30) |
Qualitative data were provided by 84 clinics (77% of 109 responding clinics). Over the past 5 years, 27 clinics had closed, 4 services had centralised and 1 had reduced from three- to two-weekly treatment sessions. However, 19 mentioned improved organisation and management, 5 dedicated consultant time, 2 IT investment and 15 mentioned the value of ECTAS in enhancing the service. When respondents were asked what changes they anticipated happening in the future, many cited a further reduction in the number of clinics due to centralisation (6 people), amalgamations (8 people) and closure (1 person). One person thought ECT could be administered by an external provider.
Discussion
The strengths of the study include a high response rate from a large geographical sample of ECT clinics and the prospective nature of data collection. The main drawback was the difficulty in accurately measuring the length of each course of ECT. As our estimate contains some patients who have not completed their courses of treatment, an underestimate of the course length is likely and no firm conclusions should be drawn about the trend. A further limitation is the failure to include private clinics. However, the 2002 study only recorded 5% of treatments at private facilities. The exclusion of private clinic ECT data from this 2002 study would have still demonstrated a steep decline in the use of ECT between 2002 and 2006. Furthermore, there is no evidence to suggest that there has been a steep rise in the provision of ECT in private facilities; it is more likely that this too has declined (J. Cresswell, personal communication, 2007).
Although our method differed from those used by the Department of Health in 1999 and 2002, there is an indication of a downward trend in ECT use. The data demonstrate a steady reduction in the quantity of ECT administered. Data also show a corresponding decline since 1999 in the numbers of patients who received treatment.
The proportion of patients receiving ECT when detained under the Mental Health Act has increased over the period covered by the three studies. Electroconvulsive therapy is under a process of centralisation and rationalisation, which may reflect the lower numbers of patients treated and a need to concentrate resources and local expertise in driving up standards. The respondents predict this is likely to continue, with a decrease in the number of ECT clinics in the next 5 years.
The reasons for the decline in the use of ECT could not be addressed by this study, although they are likely to include the publication of more restrictive guidelines (National Institute for Health and Clinical Excellence, 2003), a recent service user-led study highlighting inadequacies in the consent procedures (Reference Rose, Wykes and BindmanRose et al, 2005), availability of a greater variety of safe alternative antidepressants, patient resistance and a reduction in in-patient bed numbers. There is a possibility that this study may have underestimated ECT activity. However, our prospective method of case identification would have been more likely to identify patients treated than the retrospective methods of the 1999 and 2002 studies.
It appears that whereas the administration of ECT is becoming an increasingly specialised field within psychiatry, psychiatrists are prescribing less of it and therefore gaining less experience of its use. An important consideration arising from this is the need for psychiatrists to keep up to date with advances in ECT, for example guidelines for informed consent, new research on longer-term and autobiographical memory loss and on the technical advances in ECT administration and monitoring. This decreasing experience of prescribing ECT may perpetuate a further decline in its use.
Declaration of interest
None.
Acknowledgements
The authors thank Joanne Cresswell, Lauren Rayner and Chloe Hood for help with the survey and the clinic staff that participated.






eLetters
No eLetters have been published for this article.