The White Paper Choosing Health: Making Healthier Choices Easier (Department of Health, 2004) made a commitment to a smoke-free National Health Service (NHS) by the end of 2006. The Health Act 2006 introduced a smoking ban in public spaces across England and Wales from 1 July 2007. However, mental health units were given an exemption of 12 months for implementing this Act (Office for Public Sector Information, 2007). In the interim, the ban was partial in these units and smoking was allowed only in designated areas.
In the UK, prevalence of smoking in general population is estimated at 26% (Reference Rickards, Fox and RobertsRickards et al, 2004). Many studies have reported higher rates of smoking among service users in psychiatric hospitals at 63-72% (Reference Meltzer, Gill and HindsMeltzer et al, 1996; Reference Kelly and McCreadieKelly & McCreadie, 1999; Reference Coulthard, Farrell and SingletonCoulthard et al, 2002; Reference McCreadieMcCreadie, 2003). However, previous studies have reported variable rates of smoking among mental health professionals. A study in the UK found smoking prevalence rate among psychiatric nurses twice that found among other groups of nurses (Reference GubbayGubbay, 1992), whereas another survey in Israel reported a 48% smoking rate among staff members in mental health units (Reference Mester, Toren and Ben-MosheMester et al, 1993). In a recent study by Stubbs et al (Reference Stubbs, Haw and Garner2004), all in-patient staff working in a large private psychiatric hospital in the UK were surveyed about their smoking habits and attitudes. In this survey, 22% of respondents were smokers, 6% favoured a total smoking ban, 21.5% believed that cigarettes should be given to service users to achieve therapeutic goals, 40.2% believed that they should not be allowed to smoke with service users, 54.3% believed that smoking with service users can help create therapeutic relationships and 93.2% believed that service users would deteriorate if they couldn't have cigarettes. Staff who were smokers were more permissive towards smoking than non-smokers (Reference Stubbs, Haw and GarnerStubbs et al, 2004). In a similar survey of psychiatric units in 2006, staff feared that a smoking ban would lead to an increase in stress, aggressive and agitated behaviour, verbal abuse and serious violence from service users. Staff argued that a ban infringed on service users’ human rights and many staff who were smokers believed that it was therapeutic to smoke with service users (Reference Jochelson and MajrowskiJochelson & Majrowski, 2006).
In light of the total smoking ban from July 2008, we felt the need to study any change in attitudes about smoking among staff in NHS mental health units. We also felt that such a study could provide valuable information to guide hospitals in supporting staff and service users with the implementation of the ban.
Method
A questionnaire was drafted using themes from a previous study, after obtaining permission from the authors (Reference Stubbs, Haw and GarnerStubbs et al, 2004). The questionnaire included the following themes: occupation, gender, age, smoking status, awareness of smoking ban, views on service users smoking on the ward, views on staff smoking with service users, anticipated difficulties with the smoking ban, current support available for managing the smoking ban and views on effects of the smoking ban on staff work efficiency. Most questions had tick-box options and some had an option for additional comments (questionnaire available from the authors on request).
We distributed the questionnaire to staff (n=450) in in-patient mental health units where we worked. Data were collected between December 2006 and February 2007. The units were acute adult wards, rehabilitation wards, elderly wards and low secure units in Birmingham, Buckinghamshire and central London. The clinical staff included doctors, nurses, healthcare assistants, occupational therapists and pharmacists.
Results
We received the total of 308 responses, with a response rate of 68.4%. Respondent characteristics are shown in Table 1.
Table 1. Respondents’ characteristics

| All respondents (n=308) n (%) | Smokers (n=71) n (%) | Non-smokers (n=235)a,b n (%) | |
|---|---|---|---|
| Occupation | |||
| Manager | 17 (5.5) | 6 (1.9) | 11 (3.6) |
| Registered nurse | 116 (37.7) | 26 (8.4) | 90 (29.2) |
| Doctor | 41 (13.3) | 9 (2.9) | 32 (10.4) |
| Other | 120 (38.9) | 29 (9.4) | 90 (29.2) |
| No response | 14 (4.5) | 1 (0.3) | 12 (3.9) |
| Gender | |||
| Male | 115 (37.3) | 22 (7.1) | 93 (30.2) |
| Female | 171 (55.5) | 47 (15.3) | 122 (39.6) |
| No response | 22 (7.1) | 2 (0.6) | 20 (6.5) |
| Age group, years | |||
| 16–25 | 31 (10.1) | 11 (3.6) | 20 (6.5) |
| 26–35 | 101 (32.8) | 24 (7.8) | 77 (25.0) |
| 36–45 | 80 (25.9) | 21 (6.8) | 59 (19.2) |
| 46–55 | 59 (19.2) | 12 (3.9) | 47 (15.3) |
| 56–65 | 27 (8.8) | 2 (0.6) | 25 (8.1) |
| No response | 10 (3.2) | 1 (0.3) | 7 (2.3) |
Almost all staff (95.4%) were aware of the proposed smoking ban and 92.9% felt that passive smoking was dangerous. Less than half (46.4%) had smoked at least once in their lifetime, whereas only 23.1% were current smokers. Two-thirds of the smokers (62%) had attempted to quit smoking at least once; 52.1% felt that seeing other people smoke made it difficult to quit smoking; only 7.0% were heavy smokers (smoking more than 20 cigarettes/day).
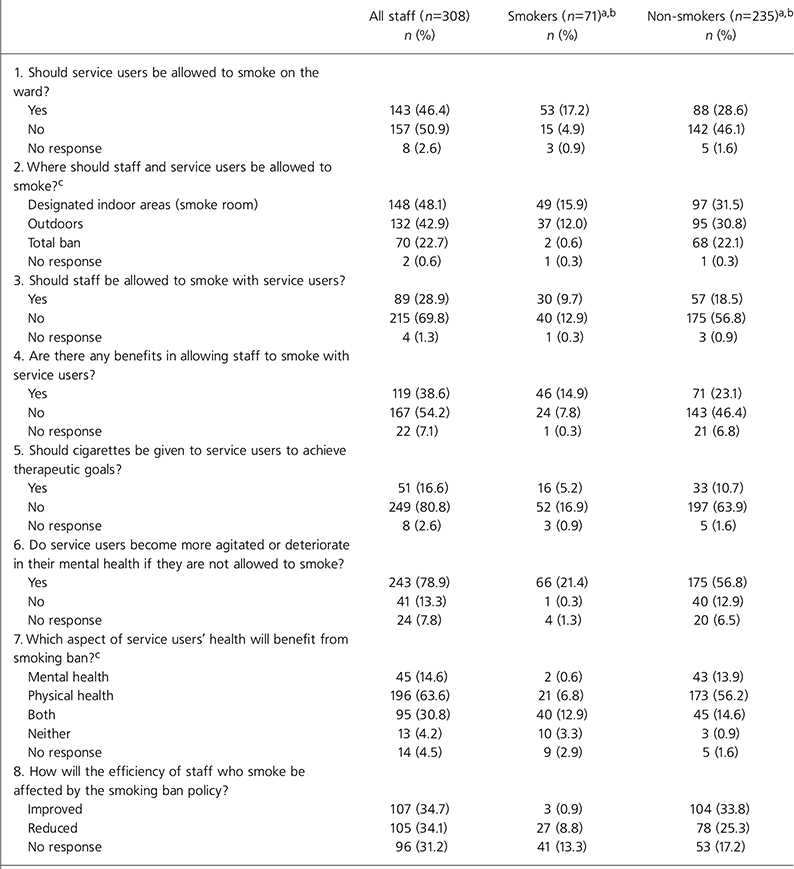
Staff views on smoking and the smoking ban are presented in Tables 2 and 3.
Table 2. Staff views on smoking and the smoking ban
| All staff (n=308) n (%) | Smokers (n=71)a,b n (%) | Non-smokers (n=235)a,b n (%) | |
|---|---|---|---|
| 1. Should service users be allowed to smoke on the ward? | |||
| Yes | 143 (46.4) | 53 (17.2) | 88 (28.6) |
| No | 157 (50.9) | 15 (4.9) | 142 (46.1) |
| No response | 8 (2.6) | 3 (0.9) | 5 (1.6) |
| 2. Where should staff and service users be allowed to smoke?c | |||
| Designated indoor areas (smoke room) | 148 (48.1) | 49 (15.9) | 97 (31.5) |
| Outdoors | 132 (42.9) | 37 (12.0) | 95 (30.8) |
| Total ban | 70 (22.7) | 2 (0.6) | 68 (22.1) |
| No response | 2 (0.6) | 1 (0.3) | 1 (0.3) |
| 3. Should staff be allowed to smoke with service users? | |||
| Yes | 89 (28.9) | 30 (9.7) | 57 (18.5) |
| No | 215 (69.8) | 40 (12.9) | 175 (56.8) |
| No response | 4 (1.3) | 1 (0.3) | 3 (0.9) |
| 4. Are there any benefits in allowing staff to smoke with service users? | |||
| Yes | 119 (38.6) | 46 (14.9) | 71 (23.1) |
| No | 167 (54.2) | 24 (7.8) | 143 (46.4) |
| No response | 22 (7.1) | 1 (0.3) | 21 (6.8) |
| 5. Should cigarettes be given to service users to achieve therapeutic goals? | |||
| Yes | 51 (16.6) | 16 (5.2) | 33 (10.7) |
| No | 249 (80.8) | 52 (16.9) | 197 (63.9) |
| No response | 8 (2.6) | 3 (0.9) | 5 (1.6) |
| 6. Do service users become more agitated or deteriorate in their mental health if they are not allowed to smoke? | |||
| Yes | 243 (78.9) | 66 (21.4) | 175 (56.8) |
| No | 41 (13.3) | 1 (0.3) | 40 (12.9) |
| No response | 24 (7.8) | 4 (1.3) | 20 (6.5) |
| 7. Which aspect of service users’ health will benefit from smoking ban?c | |||
| Mental health | 45 (14.6) | 2 (0.6) | 43 (13.9) |
| Physical health | 196 (63.6) | 21 (6.8) | 173 (56.2) |
| Both | 95 (30.8) | 40 (12.9) | 45 (14.6) |
| Neither | 13 (4.2) | 10 (3.3) | 3 (0.9) |
| No response | 14 (4.5) | 9 (2.9) | 5 (1.6) |
| 8. How will the efficiency of staff who smoke be affected by the smoking ban policy? | |||
| Improved | 107 (34.7) | 3 (0.9) | 104 (33.8) |
| Reduced | 105 (34.1) | 27 (8.8) | 78 (25.3) |
| No response | 96 (31.2) | 41 (13.3) | 53 (17.2) |
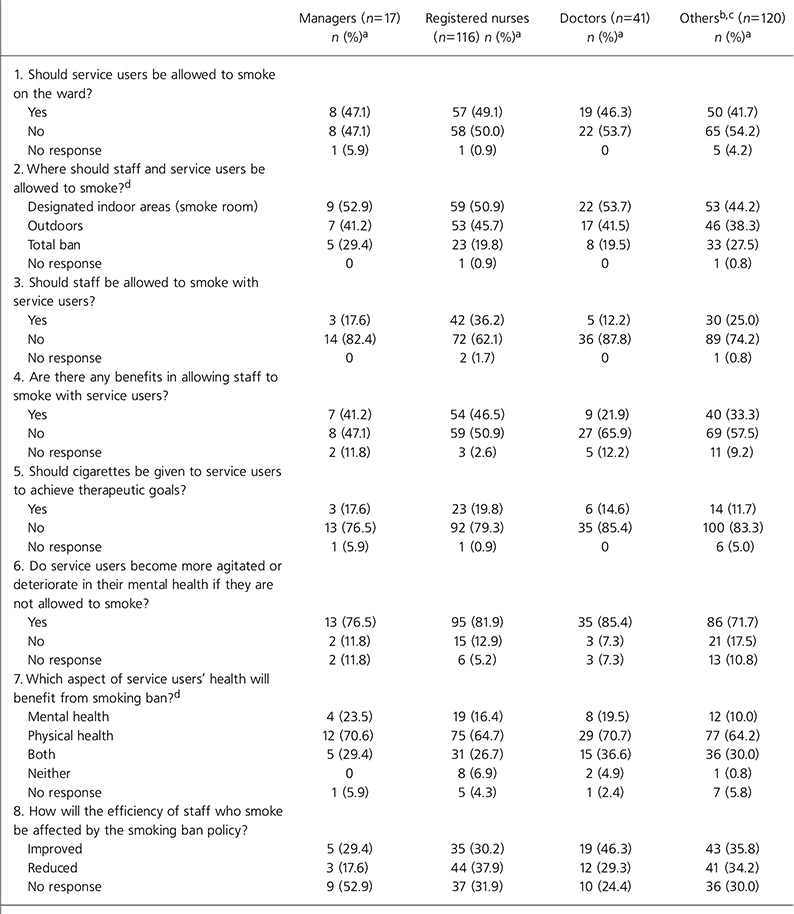
Table 3. Responses from different mental health professionals
| Managers (n=17) n (%)a | Registered nurses (n=116) n (%)a | Doctors (n=41) n (%)a | Othersb,c (n=120) n (%)a | |
|---|---|---|---|---|
| 1. Should service users be allowed to smoke on the ward? | ||||
| Yes | 8 (47.1) | 57 (49.1) | 19 (46.3) | 50 (41.7) |
| No | 8 (47.1) | 58 (50.0) | 22 (53.7) | 65 (54.2) |
| No response | 1 (5.9) | 1 (0.9) | 0 | 5 (4.2) |
| 2. Where should staff and service users be allowed to smoke?d | ||||
| Designated indoor areas (smoke room) | 9 (52.9) | 59 (50.9) | 22 (53.7) | 53 (44.2) |
| Outdoors | 7 (41.2) | 53 (45.7) | 17 (41.5) | 46 (38.3) |
| Total ban | 5 (29.4) | 23 (19.8) | 8 (19.5) | 33 (27.5) |
| No response | 0 | 1 (0.9) | 0 | 1 (0.8) |
| 3. Should staff be allowed to smoke with service users? | ||||
| Yes | 3 (17.6) | 42 (36.2) | 5 (12.2) | 30 (25.0) |
| No | 14 (82.4) | 72 (62.1) | 36 (87.8) | 89 (74.2) |
| No response | 0 | 2 (1.7) | 0 | 1 (0.8) |
| 4. Are there any benefits in allowing staff to smoke with service users? | ||||
| Yes | 7 (41.2) | 54 (46.5) | 9 (21.9) | 40 (33.3) |
| No | 8 (47.1) | 59 (50.9) | 27 (65.9) | 69 (57.5) |
| No response | 2 (11.8) | 3 (2.6) | 5 (12.2) | 11 (9.2) |
| 5. Should cigarettes be given to service users to achieve therapeutic goals? | ||||
| Yes | 3 (17.6) | 23 (19.8) | 6 (14.6) | 14 (11.7) |
| No | 13 (76.5) | 92 (79.3) | 35 (85.4) | 100 (83.3) |
| No response | 1 (5.9) | 1 (0.9) | 0 | 6 (5.0) |
| 6. Do service users become more agitated or deteriorate in their mental health if they are not allowed to smoke? | ||||
| Yes | 13 (76.5) | 95 (81.9) | 35 (85.4) | 86 (71.7) |
| No | 2 (11.8) | 15 (12.9) | 3 (7.3) | 21 (17.5) |
| No response | 2 (11.8) | 6 (5.2) | 3 (7.3) | 13 (10.8) |
| 7. Which aspect of service users’ health will benefit from smoking ban?d | ||||
| Mental health | 4 (23.5) | 19 (16.4) | 8 (19.5) | 12 (10.0) |
| Physical health | 12 (70.6) | 75 (64.7) | 29 (70.7) | 77 (64.2) |
| Both | 5 (29.4) | 31 (26.7) | 15 (36.6) | 36 (30.0) |
| Neither | 0 | 8 (6.9) | 2 (4.9) | 1 (0.8) |
| No response | 1 (5.9) | 5 (4.3) | 1 (2.4) | 7 (5.8) |
| 8. How will the efficiency of staff who smoke be affected by the smoking ban policy? | ||||
| Improved | 5 (29.4) | 35 (30.2) | 19 (46.3) | 43 (35.8) |
| Reduced | 3 (17.6) | 44 (37.9) | 12 (29.3) | 41 (34.2) |
| No response | 9 (52.9) | 37 (31.9) | 10 (24.4) | 36 (30.0) |
Staff anticipated the following problems if service users were not allowed to smoke: use of illicit ways to smoke (67.5%), absconding to smoke (58.8%), use of leave from hospital to smoke (57.1%), increased use of as needed (PRN) medication (53.2%), discharge against medical advice (34.1%) and increased use of illicit substances (28.6%). Staff were managing agitated service users (when they were not allowed to smoke) in the following ways: relaxation/distraction techniques (44.5%), allowing ventilation of feelings (39.6%), smoking breaks at designated areas (39%) and with medication when needed (19.2%).
Discussion
This study reports a smoking rate of 23.1% among mental healthcare staff and 46.4% of respondents who had smoked at least once, which is less than in previous studies (Reference GubbayGubbay 1992; Reference Mester, Toren and Ben-MosheMester et al, 1993). There were more smokers among female staff (27%) than among male staff (19%), but the overall number of smokers decreased with increasing age group. The majority of staff were aware of the smoking legislation and dangers of passive smoking.
Staff were less permissive towards smoking than in previous studies (Reference Stubbs, Haw and GarnerStubbs et al, 2004). More staff favoured a total smoking ban (22.7% v. 6%) and more were against smoking with service users (69.8% v. 40.2%). Fewer staff believed that cigarettes should be given to service users to achieve therapeutic goals (16.6% v. 21.5%), that service users’ physical and/or mental health would deteriorate if not allowed to smoke (78.9% v. 93.2%) and that allowing staff to smoke with service users was beneficial (38.6% v. 54.3%).
Staff who were smokers were more permissive in their attitudes towards smoking when compared with non-smokers. The majority of smokers (three-quarters) believed that service users should be allowed to smoke on the ward and more than half believed that staff should be allowed to smoke with them, recognising the benefits in doing so. Only 1% of smokers favoured a total ban on smoking and the majority feared that service users would deteriorate if not allowed to smoke. The conclusions of Stubbs et al's (Reference Stubbs, Haw and Garner2004) study were similar. However, three-quarters of smokers believed that cigarettes should not be used to achieve therapeutic goals.
As shown in Table 3, staff from different professional backgrounds had similar views on smoking in in-patient units and about the smoking ban. However, in comparison with other professionals, more nurses (around a third) recognised benefits in allowing staff to smoke with service users and nearly half believed that staff should be allowed to smoke with service users. This probably reflects the variable roles and practical challenges faced by different professionals within a multidisciplinary setting. Similar observations were noted in previous studies where professionals differed in their views on benefits in staff smoking with service users (Reference Mester, Toren and Ben-MosheMester et al, 1993; Reference TarbuckTarbuck, 1996).
Limitations
Studies of this nature are subject to criticism. Random sampling was not used, which might have led to sampling bias. There might have been a self-report bias among respondents and it could be argued that staff with strong views on the smoking ban, or those affected by it, were more likely to respond. Also, some would argue that using a questionnaire with tick-box options might limit the range of responses. However, many questions in this study had an option for comments and several comments were received (reporting them is beyond the scope of this paper). Additionally, the extent of change in staff attitudes might be partly caused by different work environments in private and NHS psychiatric units.
Conclusions
This study found a small but noticeable change in staff attitudes to smoking on in-patient units and the smoking ban, which could be viewed as a response to initial reforms in smoking policy. This is in line with findings from studies in other countries (Reference Lawn and PolsLawn & Pols, 2005). However, there is a need for further significant change in staff attitudes, in light of the total smoking ban. To facilitate this change, mental health services would need to create an environment where multidisciplinary staff are involved in consultation, education and training to understand the need for change and its benefits. Alternative support to assist staff in managing potential problems identified with the total smoking ban could play an important role in bringing about this change. Staff who are smokers may particularly need support during the implementation of the total smoking ban from July 2008. It would also be interesting to study staff attitudes after implementation of the total smoking ban and the effects of the ban on service users’ mental and physical health.
Declaration of interest
None.
Acknowledgements
Thanks to Dr Sanju George for his valuable opinions and suggestions on the manuscript.








eLetters
No eLetters have been published for this article.