General hospital doctors are often faced with the challenge of managing incapacitated or mentally disordered patients on general wards. All doctors should be proficient in assessing capacity and managing incapacitated patients. 1 However, research suggests that there are gaps in knowledge of this area among doctors across the specialties. Reference Hill, Mather and James2,Reference Jackson and Warner3 Until the recent introduction of the Mental Capacity Act 2005, common law permitted the treatment and care of incapacitated patients. Practice under common law has now been incorporated into the legislation laid out in the Mental Capacity Act. 4
A survey conducted by the Mental Health Act Commission found that general hospitals make use of the Mental Health Act 1983 for a relatively small but not insignificant number of patients. 5 Section 5(2) is perhaps the most commonly used order in general hospitals, particularly in acute situations or out of hours. The patient's medical or surgical team have a central role in implementing the Act, with the responsible medical officer (RMO) usually being the consultant in charge of the patient's physical care. In practice, the application is often carried out by a nominated deputy of the RMO, usually a junior hospital doctor. Documentation of the decision-making process and mental state of patients detained under section 5(2) on general wards can be poor, with no evidence that decisions have been discussed with the RMO. Reference Hardern and Protheroe6
Evidence from England, Scotland and Ireland suggests that there are significant gaps in knowledge of mental health legislation among psychiatric doctors. Reference Bhatti, Kenney-Herbert, Cope and Humphreys7-Reference Swift, Nasir, Sheehan and Casey10 However, remarkably few studies have addressed levels of knowledge of the Mental Health Act or of capacity and consent in our general hospital colleagues. Reference Lynch, Simpson, Higson and Grout11 The Mental Health Act Commission has highlighted the importance of training in its guidance notes on this matter and has suggested that this might well be provided in conjunction with a local mental health unit. 5
This study aimed to find out the level of knowledge and confidence of a cross-section of general hospital doctors regarding section 5(2), assessment of capacity and treatment of incapacitated patients under common law (as the investigation took place prior to the introduction of the Mental Capacity Act). The study also aimed to ascertain whether a simple training intervention, devised and delivered by the authors, could significantly improve knowledge and confidence.
Method
Sample
A pre-/post-intervention questionnaire survey was conducted in January 2005 of all the medical and surgical doctors attending an educational meeting at a district general hospital in the West Midlands.
Questionnaire
The anonymous, self-completed baseline questionnaire asked for demographic details and information about previous training and experience of using section 5(2), treating patients under common law and the assessment of capacity. A series of questions tested participants’ current knowledge and confidence about various aspects of treatment under common law and section 5(2). Following the training intervention, participants were asked to complete a second questionnaire with the same series of knowledge-based questions, along with additional questions asking for feedback about the training session. A code was used to match the pre- and post-training questionnaires.
Training intervention
The intervention consisted of a 1 h lecture and workshop giving information regarding the framework of capacity, common law and the Mental Health Act 1983, with particular attention to the use of section 5(2). The participants were presented with clinical scenarios and there was opportunity for discussion.
Statistical analysis
The data were analysed using the Statistical Package for the Social Sciences (SPSS version 12 for Windows). McNemar's test was used to identify any significant net improvement in knowledge for individual questions. Owing to multiple testing, Bonferroni correction was applied (adjusted significance level P<0.005).
Results
Participants
A total of 19 doctors attended the educational meeting. Of these, 18 participated by completing the pre-training and post-training questionnaires, giving a response rate of 95%. Only 2 participants returned their 1-year follow-up questionnaires so these follow-up data were not included in the analysis. Of the 18 doctors, 17 (94%) were based on medical wards and 1 (6%) was based on a surgical ward. Length of time since qualification ranged from 3 months to 26 years (mean 7.4 years) and length of time working in the UK also ranged from 3 months to 26 years (mean 6.8 years). Of the 18 participants, 8 (44%) were senior house officers (FY2 and ST1-3 equivalent), 4 (22%) were consultants, 3 (17%) were specialist registrars (ST4-6 equivalent), 2 (11%) were pre-registration house officers (FY1 equivalent) and 1 (6%) was a staff grade doctor.
Confidence and experience
Of the 18 participants, 5 (28%) said they had received formal training about section 5(2) or treatment under common law. Five (28%) said they had previous experience of using section 5(2). Six (33%) said they had previous experience of treating patients under common law. Eleven (61%) felt they would benefit from training on treatment under common law and section 5(2). The number of participants who stated they felt confident about assessing capacity increased from 8 (44%) pre-training to 15 (83%) post-training (P=0.016, not significant). The number of participants who stated they felt they had an adequate understanding of treatment under common law rose from 4 (22%) to 12 (66%) (P=0.008, not significant).
Knowledge of treatment under common law and section 5(2)
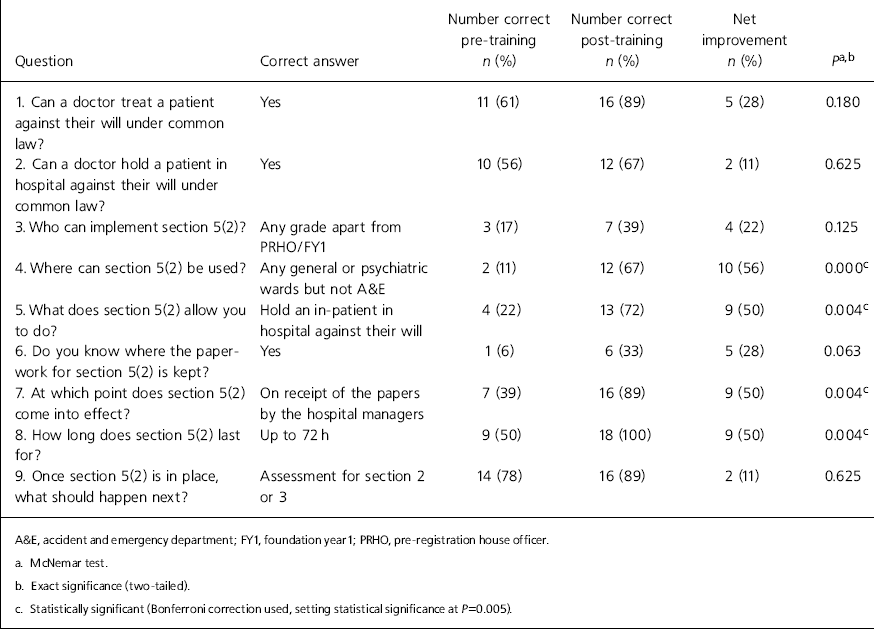
The baseline performance on the nine knowledge-based questions showed gaps in knowledge, with fewer than half of the participants answering correctly on five of the nine items (Table 1). There were net improvements in answers to all of the nine knowledge-based questions after the training, with statistical significance being achieved for four of the items.
Table 1. Participants’ knowledge before and after the training session
| Question | Correct answer | Number correct pre-training n (%) | Number correct pre-training n (%) | Net improvement n (%) | P a,b |
|---|---|---|---|---|---|
| 1. Can a doctor treat a patient against their will under common law? | Yes | 11 (61) | 16 (89) | 5 (28) | 0.180 |
| 2. Can a doctor hold a patient in hospital against their will under common law? | Yes | 10 (56) | 12 (67) | 2 (11) | 0.625 |
| 3. Who can implement section 5(2)? | Any grade apart from PRHO/FY1 | 3 (17) | 7 (39) | 4 (22) | 0.125 |
| 4. Where can section 5(2) be used? | Any general or psychiatric wards but not A&E | 2 (11) | 12 (67) | 10 (56) | 0.000c |
| 5. What does section 5(2) allow you to do? | Hold an in-patient in hospital against their will | 4 (22) | 13 (72) | 9 (50) | 0.004c |
| 6. Do you know where the paperwork for section 5(2) is kept? | Yes | 1 (6) | 6 (33) | 5 (28) | 0.063 |
| 7. At which point does section 5(2) come into effect? | On receipt of the papers by the hospital managers | 7 (39) | 16 (89) | 9 (50) | 0.004c |
| 8. How long does section 5(2) last for? | Up to 72 h | 9 (50) | 18 (100) | 9 (50) | 0.004c |
| 9. Once section 5(2) is in place, what should happen next? | Assessment for section 2 or 3 | 14 (78) | 16 (89) | 2 (11) | 0.625 |
Feedback
Of the 18 participants, 16 (88%) said they found the teaching session useful. One felt that the session had not been useful and one gave no response. Sixteen (88%) felt that their knowledge had improved as a result. One participant said that their knowledge had not improved (this respondent added a comment stating that ‘Section 5(2) should be left to the psychiatrists’) and one gave no response. Eleven participants (61%) stated that their practice would change as a result of the teaching session. Eight participants (44%) felt that the teaching could be improved, all of them stating that the use of more clinical scenarios would be helpful.
Discussion
Our study revealed a marked baseline lack of knowledge and confidence regarding the use of section 5(2), common law and capacity in this group of general hospital doctors. Interestingly, only a third of the participants felt that they had any experience of treating patients under common law. This may have been a perceived (as opposed to actual) lack of experience, perhaps indicating that some participants had been treating patients under common law while being unaware that they were doing so. There were also remarkably few participants (less than half) who felt confident about assessing capacity. These findings may reflect a fundamental lack of understanding regarding treatment under common law and capacity among some participants. The apparent lack of basic knowledge and confidence in these areas is concerning, since the introduction of the Mental Capacity Act 2005 requires doctors to demonstrate clearly that they have assessed capacity fully, made efforts to improve capacity and are acting in the patient's best interest. 4
There was an overall improvement in knowledge and confidence following the training intervention. Items for which statistically significant improvements were achieved included aspects of the powers and application of section 5(2). The lack of statistically significant improvements in other items might have been due to relatively good baseline knowledge in certain areas or smaller levels of improvement, as well as small sample size. After the training intervention there were still some gaps in knowledge in spite of all the necessary information being provided. The reasons for this were unclear but might have been due to a lack of interest in the material or the complexity of the issues covered in the training. Overall, the training intervention was well received and the participants felt they would benefit from further training. The use of clinical scenarios as a training aid generated the most interest, and participants requested more of these. The informal feedback was particularly positive from junior doctors, but it was noted some of the more senior participants were reluctant to participate in the session.
Limitations
The findings from this study should be interpreted with caution because of the small sample size, the possibility of selection bias and the difficulty in generalising the results to other populations. Also, loss to follow-up at 1 year meant that we could not tell if the improvements in knowledge and confidence were maintained, or declined over time.
Implications of the study
In conclusion, this study has shown that some general hospital doctors have a poor understanding of the assessment and management of incapacitated patients and the use of section 5(2), indicating that there is a need for training and guidance in these areas. The study showed that a relatively brief training intervention, devised and delivered by trainee psychiatrists, improved levels of knowledge and confidence within the group. With the introduction of the Mental Capacity Act, doctors will need additional understanding of the legal framework surrounding these issues and the statutory requirements incumbent upon them. There are likely to be increased demands for training and significant anxiety among general hospital doctors regarding the new legislation. We would assert that psychiatrists are well placed to deliver this type of training, as not only do psychiatrists have clinical expertise in these areas, but sharing this knowledge and experience can foster good working relationships with our general hospital colleagues.
Declaration of interest
None.
Acknowledgements
We thank Dr Sayeed Haque (Statistician, Primary Care and General Practice, University of Birmingham) for his help with the statistical analysis, Dr Richard Pether (Consultant Psychiatrist, BSMHFT) and Dr Nick Brown (Consultant Psychiatrist, BSMHFT) for their help with this project.






eLetters
No eLetters have been published for this article.