Stigma is a social construction that devalues people as a result of a distinguishing characteristic or mark. Reference Biernat, Dovidio, Heatherton, Kleck and Hebl1 The World Health Organization and the World Psychiatric Association recognise that the stigma and discrimination attached to mental disorders is strongly associated with suffering, disability and poverty. Reference Corrigan, Markowitz, Watson, Rowan and Kubiak2 The National Health Service Safer Services report observed stigma to be a major barrier to treatment seeking and suicide prevention. Reference Appleby3 Concern about the stigma of mental illness has culminated in the Royal College of Psychiatrists’ 5-year ‘Changing Minds’ campaign whose aim was to promote positive images of mental illness, challenge misrepresentations and discrimination, encourage patient advocacy, and educate the public to the real nature and tractability of mental disorder. Reference Crisp, Gelder, Rix, Meltzer and Rowlands4
The Royal College of Psychiatrists’ survey for the ‘Changing Minds’ campaign showed that people with alcoholism and drug addiction are the most stigmatised groups among people with mental illness. Reference Crisp, Gelder, Goddard and Meltzer5 Most respondents thought they were dangerous, unpredictable and hard to talk with and three out of five thought they were to blame for their condition, an opinion endorsed by only 6% of respondents in relation to schizophrenia. We therefore chose to study methods of reducing stigma towards the conditions that clearly evoked the most negative attitudes.
One method of addressing stigmatised attitudes in the interviewee is motivational interviewing, which involves the participant by providing a list of problems that their attitudes may cause to themselves and other people and giving the reasons why they may want to change their own views. Reference Miller and Rollnick6 Motivational interviewing is a brief intervention and it has been adopted for treatment of people with alcohol dependency in primary care. It can be delivered in a single 5 min consultation and is particularly useful for people who have little insight or interest in further treatment. This interview method has been widely used in individuals with a number of problems including low-self esteem, obesity, eating disorders, psychosis, non-adherence to medication and substance use disorders. It would be an ideal option for changing attitudes towards people with mental illness, especially where the participant's motivation to change is questionable, for example members of the general public.
The objective of our study was to determine whether the motivational interview technique can help reduce stigmatised attitudes of members of the general public towards those with mental illness (schizophrenia) and drug use.
Method
Participants
We recruited the participants from the general population in south Essex by direct mail-shots, newspaper advertisements and word of mouth. There were no specific inclusion or exclusion criteria other than the ability to give written informed consent. The project was approved by the local research ethics committee.
Instruments
The 5-item Attitude to Mental Illness Questionnaire (AMIQ) is a brief, self-completion questionnaire with good psychometric properties that can be used in most situations. The questionnaire was adapted from Cunningham et al Reference Cunningham, Sobell and Chow7 and validated in 879 adult volunteers. Reference Luty, Fekadu, Umoh and Gallagher8 Respondents were asked to read a short vignette describing an imaginary patient and then answer five questions (the questionnaire can be obtained from the authors on request). The individual questions were scored on a 5-point Likert scale (maximum +2, minimum –2; blank questions, ‘neutral’ and ‘don't know’ were scored 0). The scores for the five questions were added giving a total score for each vignette (between –10 and +10). Test–retest reliability at 2–4 weeks was P = 0.702 (n = 256), construct validity was α = 0.933 (n = 879) and alternate test reliability compared with Corrigan et al's Attributions Questionnaire Reference Corrigan, Markowitz, Watson, Rowan and Kubiak2 was ρ = 0.704 (n = 102).
Motivational interview
Each person was interviewed in isolation from both the other family member and other participants. The interview was composed of 20 questions adapted from a widely used manual. Reference Miller and Rollnick6 It was piloted by the lead author (a consultant psychiatrist) in 20 volunteers. He then trained the three other interviewers, who conducted two interviews with each participant, observed by the lead author. The interview was manualised to 20 short stems (the interview schedule is available on request).
Two participants were recruited from each household so that they could act as controls for each other. They were randomly assigned to receive each of the two interviews and asked to complete one version of the AMIQ for either schizophrenia or alcoholism before the motivational interview. The interview was conducted and participants then completed the second AMIQ questionnaire directed to the disorder that had been addressed in the motivational interview. For example, the AMIQ was completed in respect to alcoholism. A motivational interview was conducted regarding attitudes towards schizophrenia. A second AMIQ was then completed in respect to schizophrenia. As many questions were asked from the list of 20 as the 10-minute time period would permit. We reasoned that participants from within a household would be subject to the same socioeconomic factors that might influence their views. Interviews were performed between August 2004 and December 2005.
Data analysis
Correlation coefficients and non-parametric tests were used to compare differences in subgroups. The Wilcoxon's matched-pairs signed-ranks test was used to calculate statistical significance. The measurements were not normally distributed, although the means, standard errors and effect sizes have been quoted for convenience. These were performed using the Stats Direct statistical package for social scientists (version 2.1) for Windows.
Results
There was no difference in demographic characteristics between the control and experimental groups. For the alcohol control group and schizophrenia control group respectively the measured indices were: age (mean = 44.6 years, s.d. = 18.1 v. mean = 40.2 years, s.d. = 14.9), gender (39 v. 32% male), employment status (76 v. 78% in paid employment), ethnic origin (94 v. 92% White British) and age when leaving formal education (mean = 16.9 years, s.d. = 3.2 v. mean = 16.8 years, s.d. = 2.1; 65% of both groups left full-time education at 16 or younger).
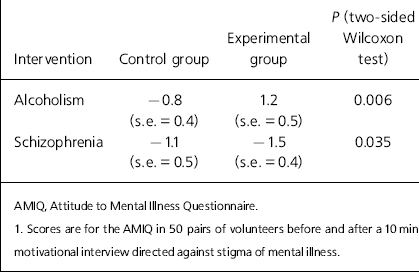
An improvement in stigma scores was observed in attitudes towards people with alcoholism (Table 1; AMIQ scores = 1.2, s.e. = 0.5 v. AMIQ = –0.8, s.e. = 0.4 in controls; P = 0.006; two-sided Wilcoxon signed-rank test adjusted for ties) but not towards those with schizophrenia (AMIQ score = –1.1, s.e. = 0.4 v. AMIQ = –1.5, s.e. = 0.4 in controls; P = 0.035). The median difference in scores for the attitude towards alcoholism was two units (95% CI 3–0.5) that translated into an effect size of 0.43.
Table 1. Results of motivational interviewing, AMIQ scores1
| Intervention | Control group | Experimental group | P (two-sided Wilcoxon test) |
|---|---|---|---|
| Alcoholism | -0.8 (s.e. = 0.4) | 1.2 (s.e. = 0.5) | 0.006 |
| Schizophrenia | -1.1 (s.e. = 0.5) | -1.5 (s.e. = 0.4) | 0.035 |
Each researcher interviewed 20–40 participants. There was no difference in outcomes between the three interviewers (a psychiatrist, a social worker and a support worker). The results of the trial are comparable with those from the large study that was used to validate the AMIQ. Reference Luty, Fekadu, Umoh and Gallagher8 Participants from both studies were self-selecting volunteers drawn from the general public.
Discussion
Attitudes to Mental Illness Questionnaire
We used the AMIQ as it is convenient and has been well validated. Other instruments are available, although these tend to be much longer, involve interviews or tend to address the experience of stigma by people with mental illness (e.g. the Internalised Stigma of Mental Illness scale), Reference Ritsher, Otilingam and Grajales9 rather than members of the general public.
Other methods to reduce stigma
Anti-stigma methods, such as the ‘Changing Minds’ campaign, Reference Crisp, Gelder, Rix, Meltzer and Rowlands4 provide factual information addressing misconceptions about people with mental illness. These have been reported to reduce stigma regardless of whether they comprise brief fact sheets or more extensive interventions such as educational courses on mental illness. Reference Mayville and Penn10,Reference Penn and Martin11 Unfortunately, their effects tend to be small, especially if the negative consequences of a mental illness are also disseminated. Although Holmes & River discuss some cognitive–behavioural methods to deal with self-stigma, the technique was not devised to exercise changes in other people's negative attitudes to those with mental illness. Reference Holmes and River12
There is a well-known report from a controlled study of the effect of a public education campaign on community attitudes towards people with mental illness following the closure of Tooting Bec Hospital in London. Reference Wolff, Pathare, Craig and Leff13 Public attitudes in the experimental area improved and patients’ social integration was enhanced. However, this was probably caused by the increased contact with patients in the experimental area rather than the dissemination of the information. Two earlier studies of a public education campaign were ineffective. Reference Cummings and Cummings14,Reference Gatherer and Reid15
Motivational interviewing used to reduce stigma towards mental illness
Motivational interviewing avoids generating resistance in the participants by having them, rather than the therapist, giving reasons for a change in attitude. It is the best described example of a brief intervention and it has been used widely among people with alcohol problems, including in two very large trials: Project MATCH and the UK Alcohol Treatment Trial (UKATT). 16,17 It can be delivered in a small number of sessions (four sessions were used in Project MATCH and UKATT).
In our study, motivational interviewing produced a small but statistically significant (10%) improvement in the AMIQ stigma score towards people with alcohol dependence; the effect size of 0.43 is conventionally regarded as modest. A smaller, insignificant improvement (2%) in attitudes towards people with schizophrenia was seen. It is possible that attitudes towards alcoholism are more flexible than those towards schizophrenia because of the negative media presentation of schizophrenia. Another factor may be that people are more likely to have personal experience of alcoholism than schizophrenia, owing to its far higher prevalence. 18 Also, Crisp et al Reference Crisp, Gelder, Rix, Meltzer and Rowlands4 showed that, unlike schizophrenia, alcoholism is regarded as self-inflicted by many people.
Conclusions
Motivational interviewing produced a modest improvement in stigmatised attitudes of members of the public towards people with alcohol dependence. Although it is unlikely that personal interviews could be performed on large population samples, the technique could be targeted to key personnel such as employers, landlords or family members (e.g. to reduce hostility and high expressed emotion within family households). This would justify further research and refinement of this brief intervention, as it can be delivered with minimal training on a large scale.
Declaration of interest
None.
Acknowledgements
The research was supported by British Academy Grant no. SG-35479.






eLetters
No eLetters have been published for this article.