Since the turn of the millennium there has been a drive to design and implement early intervention services to improve the experience of care encountered by individuals aged 14-35 who develop psychotic illness. The Department of Health Policy Implementation Guide recommended that each early intervention service should receive dedicated input from at least 0.1 whole time equivalent child and adolescent mental health service (CAMHS) professional. 1 In reality, both coverage of the adolescent client group and input from CAMHS has been highly variable as early intervention has been implemented; a 2005 survey of early intervention teams in England reported that only one in six had any dedicated input from a CAMHS professional. Reference Pinfold, Smith and Shiers2 However, a survey utilising subsequent data reported that only 26% of services failed to provide input to the lower age range of 14- to 18-year-olds. Reference Tiffin and Glover3 In addition, there are also examples of early intervention models where a high degree of integration between CAMHS and adult mental health services (AMHS) has been achieved. Reference Tiffin and Hudson4 Thus, it is likely that most early intervention teams rely on some input from child and adolescent psychiatrists when assessing and managing younger service users affected by first-episode psychosis.
Historically, managing the psychosis spectrum of illnesses has been viewed as the core business of many adult psychiatrists, whereas CAMHS predominantly maintain a focus on the assessment and management of developmental problems such as hyperkinesis and the autism-spectrum disorders. Consequently, many psychiatrists working in CAMHS encounter psychosis relatively infrequently in their practice, and may lack recent experience and expertise in recognising or managing severe mental illness presenting during adolescence. Moreover, at the time of writing the National Institute for Health and Clincial Excellence (NICE) has confined any specific recommendations in relation to ‘schizophrenia’ to adults, 5 although some guidance on the assessment and treatment of bipolar affective disorder in under-18s has been published. 6
The factors outlined above could lead to differences in the attitudes or practice of CAMHS v. adult psychiatrists dealing with first-episode psychosis. This could create differences in the experience of young people with emerging severe mental illness, depending on whether they are over 18 or not and thus is a potential source of healthcare inequity. Hence, the aims of this study were to explore whether psychiatrists working in CAMHS reported significantly different attitudes or practices in relation to first-episode psychosis when compared with a sample of adult psychiatrists working in the same organisation. The findings were intended to contribute to early intervention service development and identify any potential training needs for psychiatric staff.
Method
A self-report postal questionnaire was composed in order to gather information from psychiatrists regarding their professional characteristics, practices and attitudes in relation to first-episode psychosis. A separate group of ten psychiatrists were consulted on the draft version before the final version was distributed. The questionnaire collected information on three broad areas:
-
(a) professional characteristics (post, years in practice, number of individuals with first-episode psychosis seen);
-
(b) views and attitudes towards individuals affected by first-episode psychosis (e.g. categorisation, treatability, comorbidity, utility of prognostic factors);
-
(c) practice (e.g. psychosocial and medical interventions used and views on relative effectiveness).
A variety of response formats were utilised, including four-point Likert scales, matrices and ranked choices. Statistical analysis was conducted using chi-squared tests to compare responses between groups.
Tees, Esk and Wear Valleys is a NHS trust in an organisation that provides mental health services to a population of 1.4 million living in Teesside, County Durham and part of North Yorkshire in northern England. The questionnaire was posted to all psychiatrists working in either the adult or child and family directorates during October 2007. Three months later a follow-up letter and copy of the questionnaire was sent in order to maximise response rates. In total the questionnaire was sent to 26 CAMHS psychiatrists and 71 adult psychiatrists. Doctors working in forensic, learning disability or older people's services were not included. Psychiatrists who were undergoing basic specialist training (equivalent to senior house officer or below) were also excluded from the study as some may have had held posts in CAMHS but have lacked experience of working with young people with first-episode psychosis. Approval to conduct the staff survey as part of service evaluation and development was granted by the Tees, Esk and Wear Valleys Trust research and development department and considered exempt from external ethical review.
Results
Overall, 17 (65% completion rate) CAMHS psychiatrists (all consultant level except for 1 staff grade psychiatrist) returned a completed questionnaire as did 47 psychiatrists working in adult services (41 consultants, 2 specialist registrars and 4 staff grades) (66% completion rate). There was no significant inter-group difference between the groups in terms of years spent in practice (mean 15.7 years for AMHS v. 16.5 years for CAMHS). Most of those working in AMHS reported seeing between 5 and 20 individuals with first-episode psychosis over the past 2 years. This figure was usually cited as between two and five for the CAMHS psychiatrists, although five reported seeing ten or more such individuals.
Attitudes to first-episode psychosis
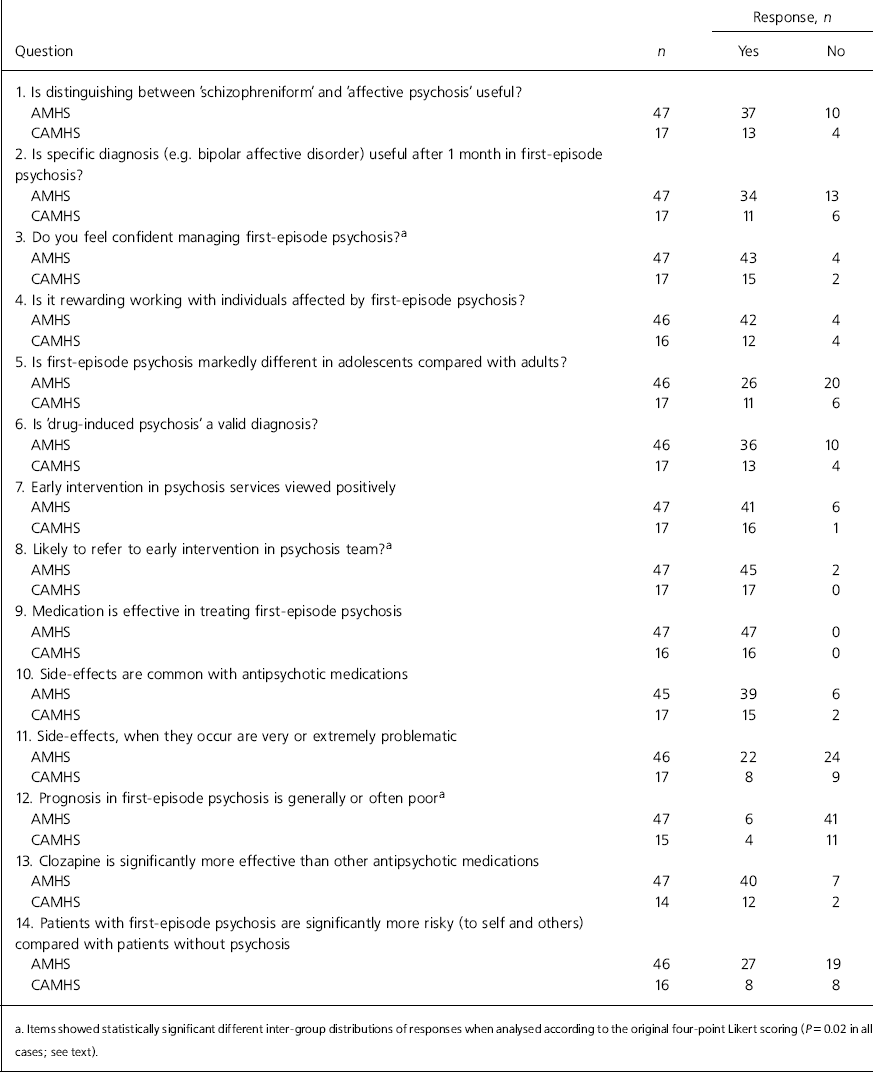
Table 1 depicts the responses to the questions relating to attitudes towards first-episode psychosis: when analysed as dichotomised positive or negative responses to the stems, there were no statistically significant inter-group differences. However, in the case of three items there were significant inter-group trends observed when the original four-point Likert responses were utilised: for item 3 (confidence in dealing with first-episode psychosis) 19 (of 47) adult psychiatrists reported feeling ‘very confident’ whereas only 1 (of 17) of the CAMHS group indicated this level of confidence (χ2 = 9.7, P = 0.02) (data not shown in Table 1). Similarly, although most adult psychiatrists (32/47) indicated they were ‘very likely’ to refer to early intervention psychosis services, only 6 (of 17) of the CAMHS group made this response to item 8 (χ2 = 7.6, P = 0.02) (data not shown in Table 1). Lastly, CAMHS psychiatrists took a mildly more pessimistic view of prognosis in first-episode psychosis; only 1 (of 15) reported the view that outcome from first-episode psychosis was ‘usually good’ for item 12 (on the four-point Likert scale). This contrasted with the adult psychiatrists where 15 (of 47) reported this view of outcome (χ2 = 9.5, P =0.02).
Table 1. The dichotomised responses of psychiatrists working in adult mental health services (AMHS) and child and adolescent mental health services (CAMHS) to the attitudinal questions
| Response, n | |||
|---|---|---|---|
| Question | n | Yes | No |
| 1. Is distinguishing between ‘schizophreniform’ and ‘affective psychosis’ useful? | |||
| AMHS | 47 | 37 | 10 |
| CAMHS | 17 | 13 | 4 |
| 2. Is specific diagnosis (e.g. bipolar affective disorder) useful after 1 month in first-episode psychosis? | |||
| AMHS | 47 | 34 | 13 |
| CAMHS | 17 | 11 | 6 |
| 3. Do you feel confident managing first-episode psychosis?a | |||
| AMHS | 47 | 43 | 4 |
| CAMHS | 17 | 15 | 2 |
| 4. Is it rewarding working with individuals affected by first-episode psychosis? | |||
| AMHS | 46 | 42 | 4 |
| CAMHS | 16 | 12 | 4 |
| 5. Is first-episode psychosis markedly different in adolescents compared with adults? | |||
| AMHS | 46 | 26 | 20 |
| CAMHS | 17 | 11 | 6 |
| 6. Is ‘drug-induced psychosis’ a valid diagnosis? | |||
| AMHS | 46 | 36 | 10 |
| CAMHS | 17 | 13 | 4 |
| 7. Early intervention in psychosis services viewed positively | |||
| AMHS | 47 | 41 | 6 |
| CAMHS | 17 | 16 | 1 |
| 8. Likely to refer to early intervention in psychosis team?a | |||
| AMHS | 47 | 45 | 2 |
| CAMHS | 17 | 17 | 0 |
| 9. Medication is effective in treating first-episode psychosis | |||
| AMHS | 47 | 47 | 0 |
| CAMHS | 16 | 16 | 0 |
| 10. Side-effects are common with antipsychotic medications | |||
| AMHS | 45 | 39 | 6 |
| CAMHS | 17 | 15 | 2 |
| 11. Side-effects, when they occur are very or extremely problematic | |||
| AMHS | 46 | 22 | 24 |
| CAMHS | 17 | 8 | 9 |
| 12. Prognosis in first-episode psychosis is generally or often poora | |||
| AMHS | 47 | 6 | 41 |
| CAMHS | 15 | 4 | 11 |
| 13. Clozapine is significantly more effective than other antipsychotic medications | |||
| AMHS | 47 | 40 | 7 |
| CAMHS | 14 | 12 | 2 |
| 14. Patients with first-episode psychosis are significantly more risky (to self and others) compared with patients without psychosis | |||
| AMHS | 46 | 27 | 19 |
| CAMHS | 16 | 8 | 8 |
Perceptions of prognostic factors
The groups were remarkably similar in their ratings of the relative importance of the list of potential prognostic factors listed (premorbid functioning, substance misuse, family functioning, other social support, concordance with medication, engagement with services, gender, personality factors, persistent positive symptoms and persistent negative symptoms). The factors felt to be most predictive were substance misuse and concordance with medication with around two-thirds of both groups placing these in their top three prognostic factors. Only about a third of respondents viewed persistent negative symptoms or family functioning as relatively important. Only ten psychiatrists placed gender or personality factors in their top three.
Perceived comorbidities
Participants were invited to record their perceptions of the five most common comorbidities in first-episode psychosis using a matrix (only those rated as in the top three were analysed). On one side was a list of conditions (specific developmental disorders; autism-spectrum disorder; learning disability; emerging/borderline personality disorder; antisocial personality disorder; social phobia; other anxiety disorders; repeated self-harm; obsessive-compulsive disorder; post-traumatic stress disorder (PTSD); depression; and epilepsy). Respondents recorded the frequency that they felt the conditions co-occurred with first-episode psychosis. Child and adult psychiatrists rated the frequency of different categories of comorbid conditions in a similar way with only three exceptions; child psychiatrists felt that specific developmental disorders (χ2 = 5.1, P =0.02) and obsessive-compulsive disorder (χ2 = 9.2, P = 0.002) more frequently co-existed with first-episode psychosis compared with the adult psychiatrists. Conversely, adult psychiatrists perceived more comorbid substance misuse compared with the child psychiatrists (χ2 =4.5, P<0.03).
Treatment strategies
Antipsychotic prescribing habits
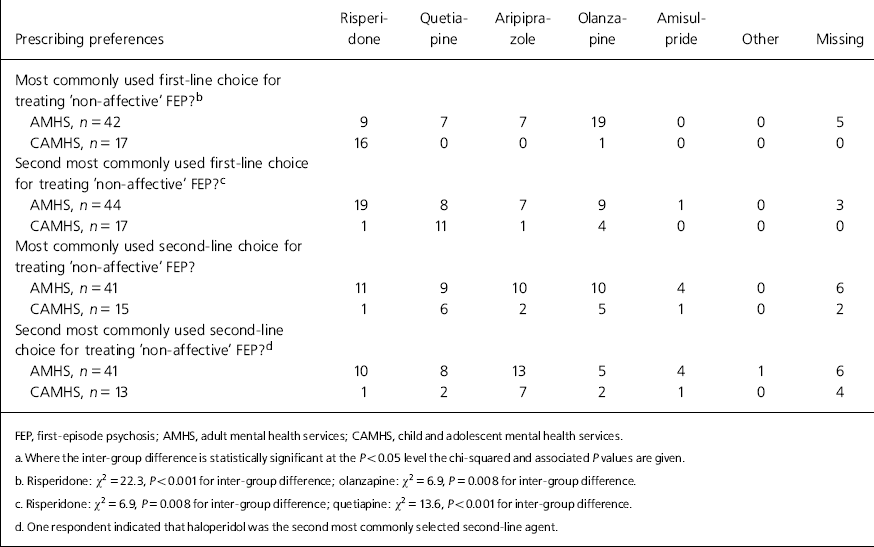
Respondents were presented with a selection of antipsychotics (risperidone, olanzapine, quetiapine, aripiprazole, amisulpride and other (to be specified), and asked which would be their most common choice for a first-line medication to use in ‘non-affective’ first-episode psychosis. This exercise was repeated for ‘second most common choice for first-line medication’, ‘most common choice as a second-line medication’ and ‘second most common choice as a second-line medication’. The results are shown in Table 2. Child psychiatrists were significantly more likely to express a preference for risperidone as a first-line agent (χ2 =22.3, P<0.001). Conversely, adult psychiatrists more frequently cited risperidone as their second most common choice as a first-line agent (χ2 =6.9, P = 0.008) and were more likely to report olanzapine as either a favourite first- or second-line treatment compared with child psychiatrists (χ2 =6.9, P =0.008).
Table 2. Respondents’ reports of their antipsychotic prescribing preferences (by proportion) for a ‘non-affective’ first episode of psychosisa
| Prescribing preferences | Risperidone | Quetiapine | Aripiprazole | Olanzapine | Amisulpride | Other | Missing |
|---|---|---|---|---|---|---|---|
| Most commonly used first-line choice for treating ‘non-affective’ FEP?b | |||||||
| AMHS, n = 42 | 9 | 7 | 7 | 19 | 0 | 0 | 5 |
| CAMHS, n = 17 | 16 | 0 | 0 | 1 | 0 | 0 | 0 |
| Second most commonly used first-line choice for treating ‘non-affective’ FEP?c | |||||||
| AMHS, n = 44 | 19 | 8 | 7 | 9 | 1 | 0 | 3 |
| CAMHS, n = 17 | 1 | 11 | 1 | 4 | 0 | 0 | 0 |
| Most commonly used second-line choice for treating ‘non-affective’ FEP? | |||||||
| AMHS, n = 41 | 11 | 9 | 10 | 10 | 4 | 0 | 6 |
| CAMHS, n = 15 | 1 | 6 | 2 | 5 | 1 | 0 | 2 |
| Second most commonly used second-line choice for treating ‘non-affective’ FEP?d | |||||||
| AMHS, n = 41 | 10 | 8 | 13 | 5 | 4 | 1 | 6 |
| CAMHS, n = 13 | 1 | 2 | 7 | 2 | 1 | 0 | 4 |
Respondents were asked how long they would wait before changing the first-line antipsychotic drug if it appeared ineffective at the maximum (British National Formulary 7 or tolerated dose) and presented with a selection of 2-week time bands ranging from ‘<2 weeks’ to ‘>10 weeks’. The distribution of responses was remarkably similar between the two groups with the median response for both groups being 4-6 weeks. When presented with a selection of indications for a trial of clozapine, almost all respondents selected ‘failure to respond to adequate trial of two antipsychotics’.
Treatment of affective symptoms
Participants were asked what their first-line approaches to depressive symptoms (of more than 2 weeks duration) in the context of a psychotic illness would likely be. Respondents could select more than one (if desired) of the following options: watchful waiting; cognitive-behavioural therapy (CBT); antidepressants; mood stabiliser; supportive psychotherapy; other (to be specified). Most psychiatrists included watchful waiting (30/47 for AMHS; 10/15 for CAMHS) and a similar proportion in each group selected the other approaches. However, CAMHS psychiatrists were significantly less likely to consider prescribing an antidepressant in this context when compared with their adult psychiatry colleagues (1/15 v. 26/47; χ2 =10.9, P = 0.001). This difference in reported practice disappeared when the prompt changed to ‘more persistent depressive symptoms lasting more than 2 months’. In this latter case the majority of both groups reported considering antidepressant treatment (36/46 for AMHS; 11/15 CAMHS).
The two groups also differed in some respects in their reports of treatments commonly prescribed during the acute phase of manic or mixed affective symptoms occurring in first-episode psychosis. Possible responses presented were: quetiapine, risperidone, olanzapine, ‘other atypical’ (to be specified); ‘typical’ antipsychotic, lithium, ‘the mood stabiliser’ (e.g. valproate or carbamazepine) and ‘other treatment’ (to be specified). Adult psychiatrists were more likely to consider olanzapine (39/47 v. 6/17; χ2 =13.6, P<0.001) and quetiapine (6/47 v. 0/17 χ2 =7.7, P = 0.005) compared with the CAMHS group. Conversely, more of the CAMHS group reported commonly using risperidone in this context compared with the AMHS group (14/17 v. 10/47, χ2 =19.9, P<0.001). Only a minority of both groups listed lithium or ‘typical antipsychotics’ as a commonly used treatment for mood elevation in acute psychosis (lithium: AMHS 9/47; CAMHS 1/17; typical antipsychotics: AMHS 3/47; CAMHS 1/17). Around a third of both groups reported using benzodiazepines in this context.
Psychosocial interventions
Both groups were very similar in their view of psychosocial interventions. Around half of the psychiatrists reported using CBT and almost all family work/therapy or supportive psychotherapy. Only one respondent in each group reported using psychodynamic psychotherapy with first-episode psychosis, whereas 17 adult and 3 child psychiatrists reported practising interpersonal psychotherapy with patients affected by first-episode psychosis. Almost all those who used these interventions reported they were effective either ‘sometimes’ or ‘often’.
Discussion
This is the first study to explore potential difference in attitudes and practices between CAMHS and AMHS psychiatrists in relation to first-episode psychosis. A wide variety of attitudes were reported by the psychiatrists responding to this survey. Some differences may reflect reality; for example, outcome in earlier-onset psychosis may be poorer compared with adult-onset illness. However, some commonly reported views did not appear to be based on scientific knowledge: for example, most felt that ‘drug-induced psychosis’ was a valid diagnosis despite a lack of empirical evidence to support the utility of this construct. Reference Poole and Brabbins8 It is also worth noting that the prognostic factors given most weight by participants were those related to service user's behaviour (‘substance misuse’ and ‘concordance’). However, remarkably few inter-group differences in the views relating to first-episode psychosis between adult and child psychiatrists were elicited, despite working in markedly different subspecialties. Nevertheless, some notable trends in prescribing practice were reported. Adult psychiatrists were more likely to report using antidepressants for medium-term depressive symptoms in contrast to CAMHS prescribers, who were unlikely to prescribe an antidepressant unless the depression was more chronic. This is generally consistent with the NICE guidelines for the treatment of depression in children and adolescents, which stresses the cautious use of selective serotonin reuptake inhibitors only after psychosocial interventions have been ineffective. 9 More surprising was the CAMHS group's reported reluctance to use quetiapine in favour of risperidone for manic-type symptoms, given that the NICE bipolar disorder guidelines for under-18s state ‘… when considering an antipsychotic, the risk of increased prolactin levels with risperidone… should be considered…’. 6 These findings suggest that CAMHS psychiatrists are more familiar with the NICE guidance on depression compared with bipolar disorder. This would be unsurprising given the client mix of most child and adolescent psychiatrists.
A second possibility that may explain the reported affinity CAMHS psychiatrists have for prescribing risperidone for first-episode psychosis would be that this medication is frequently prescribed for externalising problems in youth, such as conduct disorder, and will be relatively familiar to psychiatrists working in CAMHS from this context. Reference Olfson, Blanco, Liu, Moreno and Laje10 Quetiapine is less likely than risperidone to cause hyperprolactinaemia Reference Keller and Mongini11 and extrapyramidal side-effects, Reference Srisurapanont, Maneeton and Maneeton12 and its more extensive use could potentially reduce the exposure of children and adolescents with first-episode psychosis to unnecessary adverse drug reactions.
The high proportion of psychiatrists reporting the practice of psychosocial interventions such as CBT is encouraging, with a trend to favour those with an evidence base in psychosis treatment. Further studies would be required to evaluate to what extent this is borne out in reality.
The principal limitation of this study was the relatively small number of participants, who all worked in the same organisation. However, the response rate, at around two-thirds of the target population, was relatively high for a postal survey, although response bias cannot be excluded. Although it is possible that some trends were undetected owing to type II error, there was sufficient power to demonstrate a number of differences in self-reported practice. Moreover, many of the findings were remarkably similar in both groups surveyed and this makes the presence of undetected differences unlikely. Further surveys would be required to assess the generalisability of the trends detected in this study.
Conclusion
More work is required to understand what factors underlie the marked variations in attitudes and practice of professionals when dealing with young people affected by psychotic symptoms. More national guidance, specific to young people, would be helpful in harmonising prescribing practice. However, care must also be taken in disseminating and implementing such advice if it is to impact on the care of service users and reduce treatment inequalities across the age divide.
Declaration of interest
None.







eLetters
No eLetters have been published for this article.