The extent of problem drinking and drug use in pregnancy is difficult to estimate accurately owing to associated stigma and secrecy, and it is probably underestimated. A quarter of those presenting to drug misuse agencies are women of childbearing age. 1 A national household survey in the USA on drug use and health (2007-2008) showed 5.1% of pregnant women using illicit drugs in the past month (including cocaine). 2 The recent confidential enquiry into maternal deaths highlighted drug- and/or alcohol-related deaths in this population. Reference Lewis3 Substance misuse was directly or indirectly related to death in 57 out of 295 reported deaths (12 alcohol dependent; 45 illicit drugs dependent). The report concluded that more women were dying from direct/indirect consequence of substance misuse than other psychiatric causes. The majority died from the physical consequences of misuse rather than overdose or suicide. The majority of them did not receive care from integrated drug addiction services or were poorly managed, with significant interagency communication failures. Reference Lewis3 Studies looking at the care received by pregnant drug users have highlighted: ineffective interagency working and the importance of effective liaison between professionals in different agencies; Reference Klee4,Reference Brent5 sharing of experience; and training between organisations. Reference Morrison and Siney6
The aim of the audit was to compare local practice within substitution treatment services against the following national standards: (a) treatment aim is to achieve stability; (b) detoxification should be offered when it is client's choice and should take place in the second trimester; (c) evidence of good interagency liaison; and (d) discussion and documentation of risk-benefit analysis in the client's notes. 7
Method
A retrospective case-note review was conducted of all female clients referred or attending community drug and alcohol teams (CDATs) in Hertfordshire in the calendar year 2008 (from 1 January 2008 to 31 December 2008). Pregnant women were identified by professionals within each CDAT. Notes (hard copies and electronic notes) were assessed. Data were collected on a data-collection form to capture the characteristics of the sample and compare local practice with the above agreed standards. Descriptive statistics were used to analyse results. The results of the first cycle generated recommendations to enhance service delivery. The second cycle of the audit was conducted retrospectively for the calendar year 2010. In the second cycle, quality of services and the implementation of the recommendations generated following the first cycle were examined.
Results
During the first cycle, 21 women were identified. All but 1 used opioids, either alone (6 women) or with other drugs (14 women) and they were on substitute prescribing. One woman used only benzodiazepines. Methadone was prescribed to the majority of women (n = 17). One woman dropped out of treatment. New clients presented to CDAT late in pregnancy (average of 21.6 weeks), whereas for existing clients pregnancy was confirmed at an average of 11 weeks.
All treatment plans were agreed with the woman and reflected her choice. The treatment aim for 12 women was detoxification and for 8 it was stability (first standard). All detoxifications had taken place during the second trimester (second standard). Liaison with other services (general practitioner and midwife/antenatal services) has been documented in 19 cases (90%, third standard). Documentation of risk-benefit analysis existed in 14 cases (67%, fourth standard). The significant gaps in the interagency liaison and risk-benefit analysis have generated six recommendations, which were agreed in clinical governance and were implemented in all CDATs (Table 1).
TABLE 1 Implementation of recommendations in the second cycle (n = 25)Footnote a

| Recommendations | n (%) |
|---|---|
| Obtaining consent to liaise with other services | 17 (68) |
| Contact established by keyworker with other services | 25 (100) |
| Assertive management in pregnancy reflected in care plan | 21 (84) |
| Identification within each CDAT of a specialist team member | 25 (100) |
| Provision of information leaflets/posters to women of childbearing age | 25 (100) |
| At least one medical review during pregnancy | 23 (92) |
a. Number of pregnant women attending community drug and alcohol team (CDAT) services in Hertfordshire Partnership NHS Foundation Trust between January 2010 and December 2010.
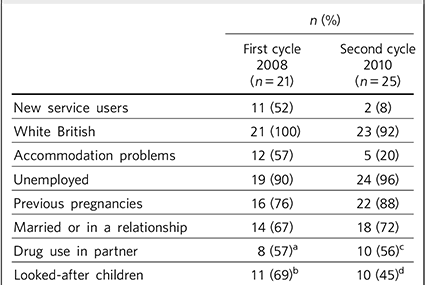
During the second audit cycle, 25 women were identified. Demographic details and comparison between the two samples are presented in Table 2. In contrast with the sample in the first cycle, only two women were new to the services. Treatment preference for stability or detoxification, time of detoxification and liaison with other services met national standards in all cases. Documentation of risk-benefit analysis has improved from 67% to 96% (present in all but one woman's notes).
TABLE 2 Comparison of the characteristics of the participants in the first and second cycle
| n (%) | ||
|---|---|---|
| First cycle 2008 (n = 21) |
Second cycle 2010 (n = 25) |
|
| New service users | 11 (52) | 2 (8) |
| White British | 21 (100) | 23 (92) |
| Accommodation problems | 12 (57) | 5 (20) |
| Unemployed | 19 (90) | 24 (96) |
| Previous pregnancies | 16 (76) | 22 (88) |
| Married or in a relationship | 14 (67) | 18 (72) |
| Drug use in partner | 8 (57)Footnote a | 10 (56)Footnote c |
| Looked-after children | 11 (69)Footnote b | 10 (45)Footnote d |
a. Total n = 14 for this variable.
b. Total n = 16 for this variable.
c. Total n = 18 for this variable.
d. Total n = 22 for this variable.
The extent of adherence to our recommendations was variable. Four recommendations were implemented in 90% and above. Obtaining consent for liaison with other services was implemented only in 68%, although liaison has taken place in all cases. The required assertive management was reflected in 84% of care plans (Table 1).
Discussion
Overall there was good adherence with the recommendations arising out of the action plan of the first cycle. A possible explanation for not having consent to liaise with other services could be explained by a verbal consent being obtained but not documented in a separate consent form. Most care plans (84%) had detailed plans to appropriately manage the client during the pregnancy. In the rest, generic plans not specific to pregnancy were found. This reflects a failure to update existing care plans, which might be a cause for concern and relevant improvement. Two women did not have a medical review at CDAT during their pregnancy, one of whom was offered appointments with the CDAT doctor but did not attend these appointments.
All the teams had identified a team member who was involved in the management of pregnant service users and who was the key liaison member for their respective teams. This has helped maintain a good relationship with other services. This member of staff had the responsibility of attending monthly liaison meetings with Social Services and maternity services to discuss this client group. Leaflets about illicit drug use, effects on menstruation, pregnancy and substitute prescription can improve education among this group. It might be a good idea for all women of childbearing age who are on substitute prescription to be given a leaflet by their keyworkers irrespective of pregnancy status. The above two recommendations might help in the early identification of pregnancy in existing CDAT clients and earlier access to substitution services for new clients.
There are several biopsychosocial factors that affect the course of a pregnancy and it is sometimes easy to forget that drug use is only one of them. It is also easy to assume that drug use by itself would make a woman incapable of caring for a baby, which is an incorrect assumption. The basic principles underlying good treatment of substance misuse problems in general apply to pregnant women, with special emphasis on the health of the unborn child. However, it should be emphasised that treatment guidelines are just guidelines and they provide a framework of good and evidence-based practice that needs to be adapted to the particular needs of each individual. Therefore, diversion from guidelines might be justifiable but this should be well supported and documented. It is difficult to measure the specific effect of the above recommendations on the improved quality of the services observed. We hope though that other service providers might find them relevant and helpful to ensure the delivery of high-quality care to a client group who are vulnerable and have complex needs.







eLetters
No eLetters have been published for this article.