It has been suggested that the prevalence of psychiatric disorders is much higher in individuals with an intellectual disability than in the general population. Reference Cutajar and Wilson1-Reference Aziz, Maixner, DeQuardo, Aldridge and Tandon3 A wide range of psychiatric treatments for this patient group are being used successfully in practice. However, electroconvulsive therapy (ECT), a treatment that has been proved beneficial in certain conditions in the general adult population, Reference Cutajar and Wilson1,4,Reference Scott5 appears to be underused in patients with an intellectual disability. Reference Cutajar and Wilson1 At the Royal College of Psychiatrists Faculty of the Psychiatry of Learning Disability's annual conference in 2010, we discussed this with some psychiatrists in this field who were unaware that ECT has ever been used in this group of patients.
Moreover, despite thorough guidance on the recommended use of ECT, the National Institute for Health and Clinical Excellence has not made any recommendations on its use in patients with an intellectual disability, 4 and the evidence of its efficacy in the literature is sparse. In the Royal College of Psychiatrists The ECT Handbook, the use of ECT in people with intellectual disabilities was thus reviewed: Reference Scott5,Reference Muir and Scott6
‘It would be good practice to use ECT only in carefully selected cases, usually where the psychiatric illness has proved refractory to medical treatment or where there are intolerable adverse effects of medication, or where the clinical condition of the sufferer has severely deteriorated… There are no absolute contraindications to the use of ECT in patients with a learning disability’ (p. 65-6).
Owing to the apparent lack of guidelines and clinicians’ uncertainty over whether ECT is used in this population, we decided to carry out a literature review to assess the current practice. We discovered that the most recent review on this subject was conducted over a decade ago by van Waarde et al. Reference van Waarde, Stolker and van der Mast7 We aimed to further this work by reviewing more recent published literature, along with evidence already previously reviewed, and answer the following questions.
-
1 To what extent has, or is, ECT being carried out in people with an intellectual disability?
-
2 Which conditions has ECT been used to treat in this population?
-
3 How successful has ECT treatment been for these patients and has it resulted in any complications or side-effects?
-
4 What factors influenced the decision to prescribe ECT for these patients?
Method
An online literature search for national and international journal articles published before March 2010 was conducted using the following databases: PubMed, MEDLINE, PsycINFO, AMED, ProQuest British Nursing Index, CINAHL, Embase, Health Business™ Elite, NHS Health Evidence Information Consortium. The search terms were: ‘ECT and’, ‘electroconvulsive therapy and’, ‘electric shock therapy and’, ‘learning disabilities’, ‘intellectual disability’, ‘mental retardation’, ‘mental deficiency’, ‘developmental disability’, ‘learning difficulty’, ‘developmental difficulty’. The eligibility criteria included any study (from individual case reports to randomised controlled trials) that included adults and children of any age with any severity of intellectual disability, as identified by the ICD-10, 8 undergoing treatment for any reason. A thorough check of references in the articles was also conducted to make sure that other sources had not been missed.
As there was only one reviewer, all reports were read and analysed in a standardised manner. The PRISMA guidelines were used to inform the methods and write-up at all stages of the study. Reference Moher, Liberati, Tetzlaff and Altman9
Results
A total of 72 cases of ECT use in patients with an intellectual disability were found in the literature. Reference Cutajar and Wilson1-Reference Aziz, Maixner, DeQuardo, Aldridge and Tandon3,Reference Bates and Smeltzer10-Reference Everman and Stoudemire44 Many studies were case reports; others were case-series reviews or were part of other literature reviews. No prospective, case-controlled or randomised controlled studies were identified.
In the cases identified, ECT was used in both male and female patients between the ages of 14 and 69. Out of the 72 cases, 51% (n = 37) of individuals had mild intellectual disability, 29% (n = 21) had moderate disability, 4% (n =3) severe and 2% (n = 2) profound; in 12.5% (n = 9) the severity of intellectual disability was not stated. We used the IQ levels as given in the ICD-10 to categorise the severity of intellectual disability. 8
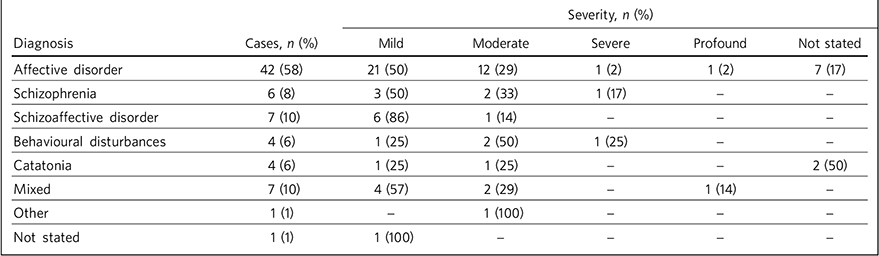
Indications for ECT were wide ranging (Table 1). Affective disorders were by far the most commonly diagnosed both in total (59%) and in each level of severity of intellectual disability. Some patients had no documented diagnosis (10%), but presented with varied/mixed symptoms.
TABLE 1 Psychiatric diagnoses and levels of intellectual disability in the reviewed studies
| Severity, n (%) | ||||||
|---|---|---|---|---|---|---|
| Diagnosis | Cases, n (%) | Mild | Moderate | Severe | Profound | Not stated |
| Affective disorder | 42 (58) | 21 (50) | 12 (29) | 1 (2) | 1 (2) | 7 (17) |
| Schizophrenia | 6 (8) | 3 (50) | 2 (33) | 1 (17) | — | — |
| Schizoaffective disorder | 7 (10) | 6 (86) | 1 (14) | — | — | — |
| Behavioural disturbances | 4 (6) | 1 (25) | 2 (50) | 1 (25) | — | — |
| Catatonia | 4 (6) | 1 (25) | 1 (25) | — | — | 2 (50) |
| Mixed | 7 (10) | 4 (57) | 2 (29) | — | 1 (14) | — |
| Other | 1 (1) | — | 1 (100) | — | — | — |
| Not stated | 1 (1) | 1 (100) | — | — | — | — |
The majority of patients had undergone several trials of multiple medications before ECT was prescribed. Only in 45 cases the exact medications that had been trialled prior to ECT were reported, but of these, an average number of 5 different medications were tried, including various antidepressants, antipsychotics, benzodiazepines, sedatives, anxiolytics and mood stabilisers. Four patients had been treated with ECT in the past and two had received behaviour therapy.
There was a wide range in the total number of ECT treatments received by patients and the course given did not seem to correlate to the severity of intellectual disability (Table 2). This may partly be due to the small numbers of patients with severe and profound intellectual disability in the studies. Overall, bilateral electrode placement was far more commonly used than unilateral placement.
TABLE 2 Range of treatments given within each category of intellectual disability

| Level of intellectual disability | Average, n (range) |
|---|---|
| Mild | 8 (1—18) |
| Moderate | 9 (3—21) |
| Severe | 7 (1—12) |
| Profound | 8 (6—10) |
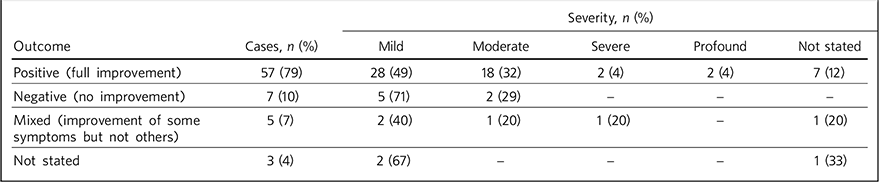
The therapy resulted in a positive outcome in the majority of cases (79%) and most patients in each level of severity of intellectual disability had a positive outcome (Table 3). Only in seven cases (10%) was a negative outcome or no improvement at all reported; 20 patients (28%) required continuation/maintenance ECT and 51 (71%) required medication during the follow-up. One patient also received occupational and art therapy after she completed her ECT treatment.
TABLE 3 Outcome of electroconvulsive therapy in the sample
| Severity, n (%) | ||||||
|---|---|---|---|---|---|---|
| Outcome | Cases, n (%) | Mild | Moderate | Severe | Profound | Not stated |
| Positive (full improvement) | 57 (79) | 28 (49) | 18 (32) | 2 (4) | 2 (4) | 7 (12) |
| Negative (no improvement) | 7 (10) | 5 (71) | 2 (29) | - | - | - |
| Mixed (improvement of some symptoms but not others) | 5 (7) | 2 (40) | 1 (20) | 1 (20) | - | 1 (20) |
| Not stated | 3 (4) | 2 (67) | - | - | - | 1 (33) |
Despite the large number of apparent successes, there were also a large number of relapses: 23 patients (32%) experienced at least one relapse following the reported course of ECT and 16 of those patients required further ECT treatments.
Complications
Complications following ECT arose in nine cases (12%) and included: transient mild memory impairment, Reference Lazarus, Jaffe and Dubin12 drowsiness for 24 h, Reference Friedlander and Solomons35 delirium in a man with autism receiving ECT for severe depression, catatonia and self-injury, Reference Ligas, Petrides, Istafanous and Kellner40 and ‘flat facial expression’ after four treatments that resolved spontaneously 3 weeks later. Reference Friedlander and Solomons35 Several studies reported an increase in agitation, both in the postictal state Reference Slack and Stoudemire23 and following several treatments. Reference Friedlander and Solomons35 One patient, who had underlying chronic obstructive pulmonary disease, became agitated and hypoxic, requiring nebulisations of albuterol and beclomethasone. Reference Thuppal and Fink2 Seizures were noted in two cases, one of a person having two fits (not described) following an ECT session, Reference Cutajar and Wilson1 and another of a male with moderate intellectual disability who developed non-convulsive status epilepticus after his ninth ECT session for catatonic psychosis. Reference Jyoti Rao, Gangadhar and Janakiramaiah26
Objective measurements of outcome used
Two retrospective chart review studies that objectively measured the outcome of ECT using standardised rating scales were also found in the literature. Out of the total 72 cases, 10 had been reviewed retrospectively by Friedlander & Solomons, Reference Friedlander and Solomons35 who assessed the outcome of ECT using the Clinical Global Impressions (CGI) scale. Out of the 10 patients they reviewed, 7 had ‘much improved or very much improved’, indicated by a CGI score of either 1 or 2, and this improvement was ‘rapid and dramatic’. The remaining three patients had an ‘equivocal response’, indicated by a CGI score of 3 or 4. None of the patients deteriorated during the course of treatment.
Similarly, Reinblatt et al Reference Reinblatt, Rifkin and Freeman45 reviewed 20 in-patients to assess symptoms and clinical improvement after ECT treatment, using the CGI scale and Aberrant Behaviour Checklist (ABC). This was then compared with patients’ initial diagnoses to determine whether ECT may be more efficacious for certain diagnoses in this patient population. This study showed that most patients had a good response to ECT, but also concluded that ECT was most useful for ‘mood disorders and psychotic disorders, after adequate pharmacological trials have failed’. Out of the five subscales of the ABC, ECT was most effective in treating irritability and hyperactivity. The study found no side-effects and, although not formally tested for, signs of cognitive impairment or deterioration were not observed.
A further 3 cases (out of the 72) objectively measured the outcome of ECT using similar scales to the studies above. Puri et al Reference Puri, Langa, Coleman and Singh15 used the Adaptive Behaviour Scale (ABS) in a male with mild intellectual disability treated for chronic relapsing depression. The patient showed improvement in all ten areas of the ABS and had fewer maladaptive behaviours. Gabriel Reference Gabriel29 used the Brief Psychiatric Rating Scale (BPRS) and the Global Assessment of Functioning scale (GAF) for a female patient with moderate intellectual disability treated for refractory psychosis. The patient's score on the BPRS decreased from 85 to 42 and her score on the GAF increased from 25 to 40, indicating significant clinical improvement. Mackay & Wilson Reference Mackay and Wilson39 reported a dramatic improvement in the mental state of a female with mild intellectual disability after she received treatment for depression. This was measured using the Glasgow Depression Scale for people with Learning Disability (GDS-LD).
Discussion
The results of this review show that ECT has been used effectively and with few serious side-effects for a wide range of psychiatric disorders in individuals with an intellectual disability. In particular, it has been used for those patients whose illness is treatment resistant and whose condition has severely deteriorated. There was no reported evidence of further cognitive decline in any of the case studies. Relapses following ECT treatment were noted, but this also often occurs in the general adult population. Reference van Waarde, Stolker and van der Mast7 This suggests that ECT may be a particularly useful treatment for this patient group, especially when used as an adjunct to other treatments, and so could potentially be applied more frequently, particularly in challenging cases. Reid, Reference Reid46 who reviewed 21 patients with an intellectual disability and ‘manic depressive psychosis’, concluded that a combination of antidepressants and ECT was effective in most patients with mild and borderline disability.
Despite the positive nature of the results, we also found several reported obstacles to the use of ECT in patients with intellectual disabilities, which are summarised below.
Diagnostic uncertainty
Diagnostic problems are quoted frequently in the literature. In the survey by Cutajar & Wilson Reference Cutajar and Wilson1 of consultant opinions on the use of ECT in intellectual disability, difficulties with diagnosis was a frequently quoted reason as to why consultants believe ECT is underused in these patients. Sayal & Bernard Reference Sayal and Bernard47 also quoted ‘diagnostic overshadowing’ as a problem in which ‘the knowledge of the presence of a learning disability reduces the likelihood that emotional or behavioural disturbance is appropriately diagnosed’. This can result in delayed use of ECT. Reference Kessler37
The impact of diagnostic difficulties in prescribing ECT to patients with an intellectual disability was first raised as an issue for discussion in 1996 Reference Bebchuk, Barnhill and Dawkins16 and was still being discussed in 2010. Reference Wachtel, Griffin and Reti41 This highlights the need for further improvements in diagnostic acuity in this patient group.
Consent and agreement among key groups
Many individuals with intellectual disability lack the capacity to give informed consent, Reference Muir and Scott6 although, in keeping with the Mental Capacity Act 2005, every effort must be made before this conclusion is reached. Reference Barnes, Dyer, McClelland, Scott and Scott48 Mackay & Wilson Reference Mackay and Wilson39 reported the case of a young female with mild intellectual disability who was able to give informed consent for ECT for major depression through the use of a communication tool provided by speech and language therapists, ‘Talking Mats’, which uses pictures to help patients understand treatments and their implications. Reference Mackay and Wilson39 It is possible that professionals from key groups who are involved in the care of these patients could be trained to use such tools to improve ways of gaining consent in the future.
Problems with obtaining informed consent are a recurring theme in the literature and clinicians seem to view this as a major stumbling block. Reference Cutajar and Wilson1,Reference Thuppal and Fink2,Reference Muir and Scott6,Reference van Waarde, Stolker and van der Mast7,Reference Bates and Smeltzer10,Reference Little, McFarlane and Ducharme36,Reference Mackay and Wilson39,Reference Reinblatt, Rifkin and Freeman45 Cutajar & Wilson Reference Cutajar and Wilson1 quoted ‘obtaining informed consent’ as a practical difficulty in ECT administration. Legal issues surrounding consent can be complex, and inevitably differ across the world and even in different areas in the UK. Reference Muir and Scott6,Reference van Waarde, Stolker and van der Mast7 If a patient is incapacitated but complies, in most settings a ‘best interests’ meeting is held in which carers, professionals and practitioners involved in different aspects of the patient's care and support will discuss the best way to proceed. 49 This is in concordance with the Mental Capacity Act 2005, which in Part 1.1 states that ‘An act done, or decision made, under this Act for or on behalf of a person who lacks capacity must be done, or made, in his best interests.’ The Act outlines the principles of ‘best interests’ in Part 1.4.
In general adult psychiatry, if ECT is deemed appropriate and the best treatment option for a patient who is unable to consent and unwilling to comply with treatment, Section 58A of the Mental Health Act 1983 (2007 amendment) can be applied to prescribe ECT and medication given as part of ECT. This principle applies in people with an intellectual disability as it does in the mainstream population.
Given the often negative perception of ECT as a treatment, the process of reaching a decision may be even more challenging if carers, relatives and support workers are not properly educated about its indications, procedure and effects. Reference van Waarde, Stolker and van der Mast7,Reference Reinblatt, Rifkin and Freeman45 Consultant psychiatrists identified ‘resistance by carers/staff’ as a reason why ECT is underused in this population. Reference Cutajar and Wilson1 It has also been described that in some countries patients have been undertreated with ECT due to lobbying by advocacy groups against continuing the treatment. Reference Friedlander and Solomons35 This shows that more work needs to be done to educate and allay fears in these key groups as well as in the wider population.
Adverse cognitive effects
One of the main fears of using ECT in patients with intellectual disability is that it will cause a further degree of cognitive decline or brain damage. Reference van Waarde, Stolker and van der Mast7 Sayal & Bernard Reference Sayal and Bernard47 stated that this could have been a reason as to why trainees in their study were less likely to agree to the use of ECT in a case vignette of a patient with an intellectual disability. Previous studies demonstrate that consultants gave ‘irrational fear of worsening pre-existing organic damage’ as a reason why ECT is underused in those patients. Reference Cutajar and Wilson1
Although there is evidence to support cognitive side-effects of ECT such as amnesia, there is no evidence in the ECT literature that it causes actual brain damage, Reference Thuppal and Fink2,Reference Weiner50-Reference Puri, Oatridge, Saeed, Ging, McKee and Lekh52 and in all of the cases studied in this review, none reported any serious cognitive decline or adverse cognitive side-effects following ECT. Friendlander & Solomons Reference Friedlander and Solomons35 stated that ‘this finding is not unexpected, as other at-risk populations, such as geriatric patients with dementia or adolescents with severe mental illness have not been shown to be at increased risk of cognitive side effects.’ Similarly, van Waarde et al Reference van Waarde, Stolker and van der Mast7 noted that ECT has been used safely in patients who have central nervous system disorders. However, since there have been no controlled studies that look particularly at the effects of ECT in patients with an intellectual disability, it cannot be said that ECT is completely safe in this population, and because there is no firm guidance on how it should be used in these patients, it is understandable why most clinicians are reluctant to try it.
Pharmacology
The majority of patients in this review who eventually received ECT had first been tried on multiple psychotropic medications, whereas it has been reported that individuals with intellectual disabilities are more biologically and cognitively sensitive to medications and are also at a greater risk of adverse side-effects. Reference Aziz, Maixner, DeQuardo, Aldridge and Tandon3,Reference van Waarde, Stolker and van der Mast7,Reference Wachtel, Griffin and Reti41,Reference Wachtel, Hermida and Dhossche42 This is thought to be due to structural brain differences and coexistence of other somatic disorders. Reference van Waarde, Stolker and van der Mast7 If patients with intellectual disability are likely to suffer more because of these medications and their inability to report somatic side-effects, it may be that ECT would benefit them by reducing the need for multiple medications. Reference Aziz, Maixner, DeQuardo, Aldridge and Tandon3 Therefore, in specific patients, ECT may actually be the more conservative treatment option. Reference van Waarde, Stolker and van der Mast7 Reducing the number of unnecessary medications would also inevitably result in cost savings; still, such savings would have to be balanced against the cost of prescribing ECT. As currently there are no studies that compare the efficacy, safety and cost-efficiency of ECT with that of medications in patients with an intellectual disability, Reference van Waarde, Stolker and van der Mast7 one can only speculate on this point.
Ethical considerations
Because ECT was mainly used as a last resort, the condition of several patients before ECT treatment deteriorated to the extent that it was deemed life threatening. Many patients experienced multiple somatic symptoms such as food refusal, profound weight loss, urinary retention, incontinence and motor disturbances, and others displayed dangerous self-injurious behaviours, suicidality, aggression and violence towards carers, which resulted in them being kept in restraints for a large part of the day. Reference Wachtel, Griffin and Reti41 On the other hand, once ECT was commenced, many patients showed a dramatic and rapid improvement. We argue that it is not ethical to leave patients in such a state when there is an alternative treatment available that could be very successful. We agree with other authors who feel that ECT should be considered more promptly in severe cases rather than being seen as a treatment of last resort. Reference Little, McFarlane and Ducharme36,Reference Ligas, Petrides, Istafanous and Kellner40 Prompt treatment with ECT could also have implications for key individuals involved in the day-to-day care of these patients, as it could bring in cost savings through a reduction in levels of staffing and supervision required.
In their review of clinical and ethical issues, Little et al Reference Little, McFarlane and Ducharme36 put forward the argument that clinicians can use ethical justification to help them with the decision to prescribe ECT. They cite the literature describing the ethical justification for ECT in general psychiatry and propose that further ethical support be drawn from utilitarian-based and duty-based reasoning. Reference Little, McFarlane and Ducharme36 They also state that in the absence of guidance from the literature, the potential for causing adverse cognitive effects through the use of ECT can be justified under the rule of double effect. Reference Little, McFarlane and Ducharme36
The complex ethical arguments embedded in the issue of ECT use in people with an intellectual disability could fill a paper of their own, and they are unfortunately outside the scope of this review. Until further studies are conducted, clinicians will have to rely on other forms of support/guidance when considering this treatment option in patients with an intellectual disability.
The need for controlled and valid research into this field has been highlighted several times in this review; yet controlled studies with people with an intellectual disability are often complicated to conduct both methodologically and ethically. Reference Stalker53 Issues faced by researchers involve several we have already mentioned, such as problems with gaining informed consent, the lack of reliable measuring scales and attitudes of both professionals and lay groups. Other problems have also been reported, such as the need to obtain formal approval from agencies or service providers to gain access to potential participants, the time-consuming nature of designing and conducting studies in this population, and problems with dissemination after research is complete. Reference Stalker53,Reference Rodgers54 There is also much discussion in the literature about involving individuals with intellectual disability in the research process, giving rise to lengthy debates about participatory and emancipatory research designs. Reference Gilbert55 Such deliberations are outside the scope of this paper, yet they are pertinent to any research in this population.
In addition to the issues discussed, all researchers will have to gain ethical approval for their study, which can be a complex and lengthy process for any type of research, Reference Smajdor, Sydes, Gelling and Wilkinson56 but is even more so for a cohort with an intellectual disability, as such individuals are viewed as being vulnerable. Reference Hays, Murphy and Sinclair57 This may appear as a further barrier to potential researchers.
Despite these problems, it is evident in the literature that randomised controlled trials conducted in intellectual disability psychiatry are on the increase, Reference Hassiotis58 which is certainly a step in the right direction.
Study limitations
As we identified no controlled studies and this review is based mainly on case reports, in which there may have been elements of selective reporting, it is difficult to draw firm conclusions about the use of ECT in patients with an intellectual disability. Moreover, the sample is relatively small and there is a definite skew in the severity of intellectual disability represented, with the majority of case reports being of patients with mild and moderate disability.
All the reports were identified and reviewed in a standardised manner by one reviewer. Still, there remains the possibility of publication bias favouring positive results. Reference van Waarde, Stolker and van der Mast7,Reference Reudrich and Alamir17 This may affect the cumulative evidence and means that the results should be interpreted with caution. Only a handful of studies measured outcome and effects on cognitive function in an objective, standardised manner, using validated rating scales. Reference Lazarus, Jaffe and Dubin12,Reference Puri, Langa, Coleman and Singh15,Reference Chanpattana18,Reference Gabriel29,Reference Mackay and Wilson39 Most authors used subjective clinical observation and judgement to determine outcome, which makes it difficult to compare cases and interpret the outcomes objectively.
Finally, despite carrying out a thorough literature search, only English-language journals were searched.








eLetters
No eLetters have been published for this article.